Nutrition and Health — MCQs

On this page
Which of the following pulses contains the highest amount of protein?
Which protein quality indicator was adopted by the Indian Council of Medical Research (ICMR) when recommending dietary protein requirements?
What is the recommended daily calorie intake during late pregnancy?
Amongst the following fats and oils, which has the highest proportion of polyunsaturated fatty acids (PUFA)?
Which of the following statements regarding the refining of oils is NOT TRUE?
Which type of milk among the following has the lowest protein content?
All of the following are used to assess the mid-upper arm circumference except?
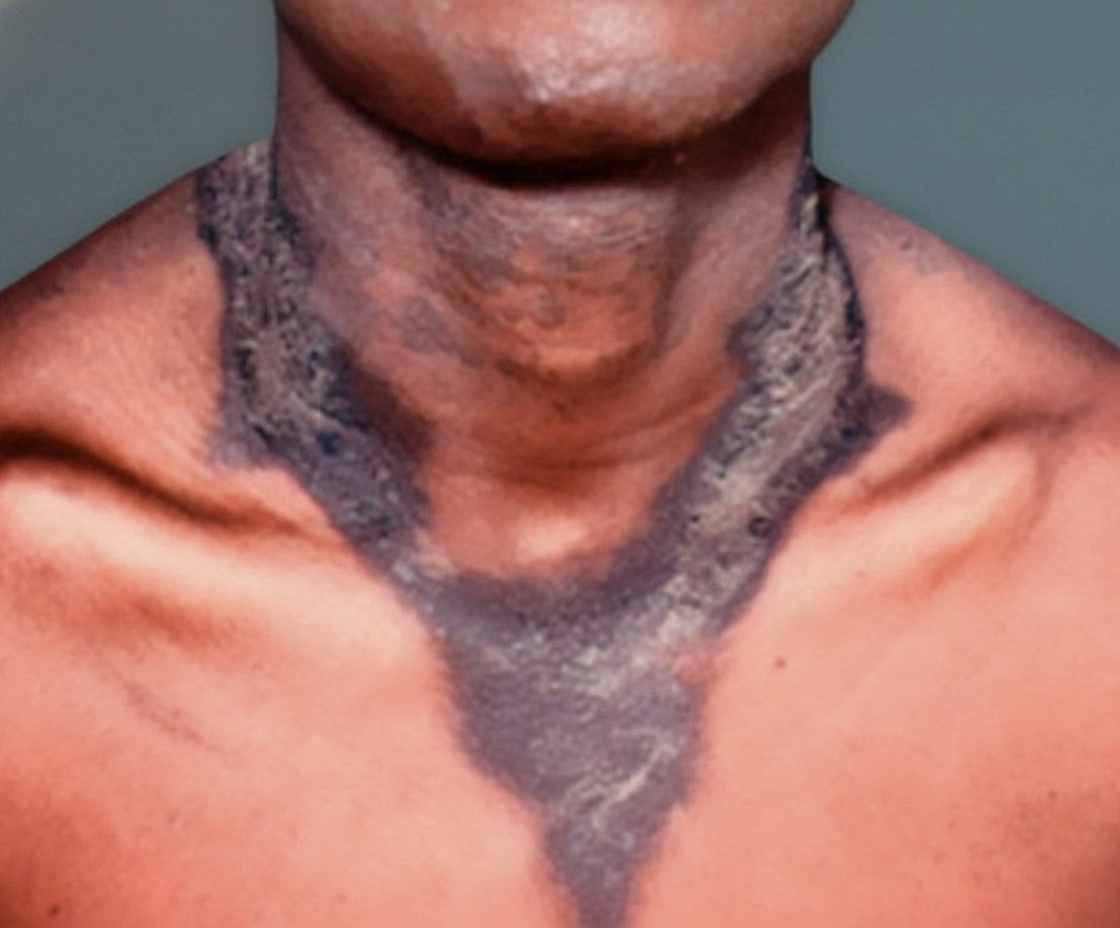
Clinical features presented below are due to deficiency of:
Which one of the following cooking oils contains the highest percentage of linoleic acid?
What is the total recommended amount of iron supplementation during pregnancy?
Practice by Chapter
Basic Nutritional Requirements
Practice Questions
Assessment of Nutritional Status
Practice Questions
Protein-Energy Malnutrition
Practice Questions
Micronutrient Deficiencies
Practice Questions
Nutritional Programs in India
Practice Questions
Dietary Guidelines
Practice Questions
Food Safety and Security
Practice Questions
Diet and Non-Communicable Diseases
Practice Questions
Nutrition in Pregnancy and Lactation
Practice Questions
Infant and Young Child Nutrition
Practice Questions
Nutrition in Emergencies
Practice Questions
Food Fortification and Supplementation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
