Infectious Diseases — MCQs

On this page
As per ICMR guidelines, which of the following are the criteria for SARS-COV-2 exposure for a pregnant female during the COVID-19 pandemic? 1. Travel to an affected country within previous 14 days 2. Close contact with a confirmed case within a distance of 1 metre for more than 15 minutes 3. Residing in a containment zone 4. Healthcare workers examining a confirmed case without adequate protection
Which one of the following mosquitoes is responsible for transmitting Japanese encephalitis?
Which of the following diseases has man as an incidental host with ‘Pig → Mosquito → Pig’ as the basic cycle of transmission?
What is the most important test to assess the prevalence of tuberculosis infection in a community?
What is the window period for HIV infection?
With reference to dengue virus, consider the following statements: 1. In India, all the four serotypes are found. 2. The reservoir of infection is both man and mosquito. 3. Adults usually have a milder disease than children. 4. Dengue hemorrhagic fever is caused by infection with more than one dengue virus. Which of the statements given above is/are correct?
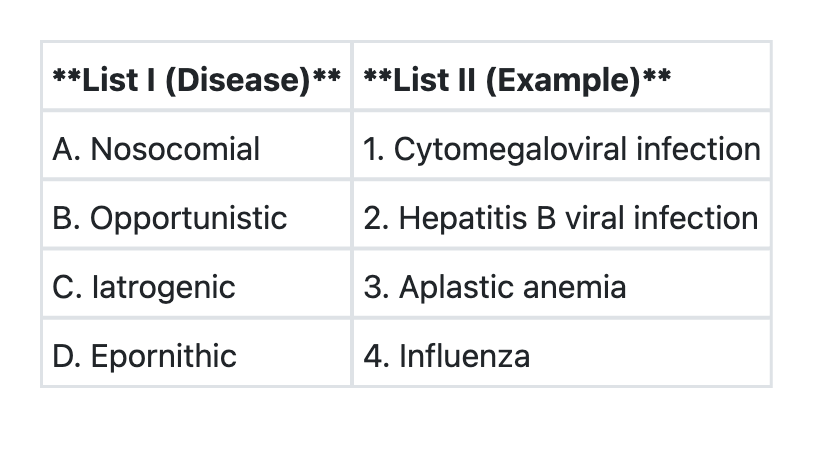
Match List I with List II and select the correct answer using the codes given below the lists:
Which of the following statements is true about hydatid disease?
Consider the following features of food poisoning: 'Incubation period less than 24 hours, source of infection is milk products, and symptoms include diarrhoea and vomiting.' To which of the following does the above description apply? 1. Staphylococcal food poisoning 2. Salmonella food poisoning 3. Botulism Select the correct answer using the code given below:
With reference to the Revised National Tuberculosis Control Programme, consider the following statements: 1. Active case finding is pursued under this Programme. 2. Microscopy centres are established in the districts for every one lakh population and in hilly and tribal areas for every 50,000 population. Which of these statements is/are correct?
Practice by Chapter
Communicable Disease Control Principles
Practice Questions
Vector-Borne Diseases
Practice Questions
Water-Borne Diseases
Practice Questions
Air-Borne Diseases
Practice Questions
Zoonotic Diseases
Practice Questions
Sexually Transmitted Infections
Practice Questions
HIV/AIDS Control Program
Practice Questions
Tuberculosis Control
Practice Questions
Leprosy Elimination
Practice Questions
Emerging and Re-emerging Infections
Practice Questions
Hospital-Acquired Infections
Practice Questions
Integrated Disease Surveillance Project
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
