Infectious Diseases — MCQs

On this page
One of the following diseases has more than one route of transmission :
Universal precautions to be followed by the surgical team include all of the following except :
Which one of the following is a stomach poison for the larvae of insects of medical importance ?
The detection of sore throat cases in children and their treatment with Benzathine Penicillin in Community Control Programme of Rheumatic Fever/Rheumatic Heart Disease (RF/RHD) constitutes
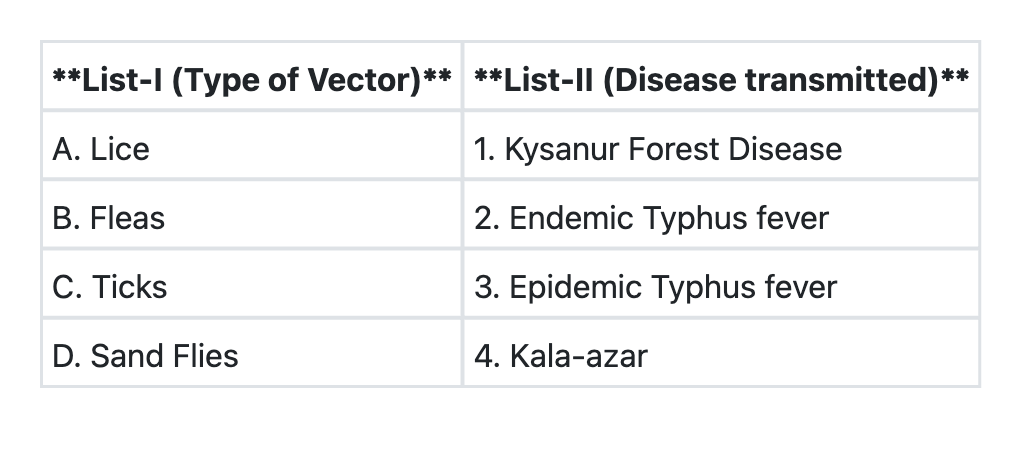
Match List-I with List-II and select the correct answer using the code given below the Lists:
The incubation period of mumps is
Consider the following statements : HIV can be transmitted to a healthcare worker from a patient through : 1. A needle stick injury 2. Contact with the patient's blood 3. External examination of the patient 4. Inhalation Which of the statements given above is/are correct ?
Which of the following will qualify as a Class III exposure to Rabies?
A 15-month-old child presents with fever and cough since the last two days, the respiratory rate is 55/min and there is no drawing of the chest. According to the National Programme for Acute Respiratory Infections, the line of management should be
Under the DOTS strategy of Revised National Tuberculosis Programme, the recommended line of management in Category I patients, if the sputum is positive after 2 months of Intensive Phase treatment with 4 drugs, is to
Practice by Chapter
Communicable Disease Control Principles
Practice Questions
Vector-Borne Diseases
Practice Questions
Water-Borne Diseases
Practice Questions
Air-Borne Diseases
Practice Questions
Zoonotic Diseases
Practice Questions
Sexually Transmitted Infections
Practice Questions
HIV/AIDS Control Program
Practice Questions
Tuberculosis Control
Practice Questions
Leprosy Elimination
Practice Questions
Emerging and Re-emerging Infections
Practice Questions
Hospital-Acquired Infections
Practice Questions
Integrated Disease Surveillance Project
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
