Vitamins and Coenzymes — MCQs

On this page
Which vitamin deficiency can cause rickets?
Thiamine deficiency in a chronic alcoholic can reduce energy production as a result of which of the following reasons?
Hypervitaminosis D may cause all of the following EXCEPT:
The deficiency of thiamine can be identified by measuring the red cell:
Which of the following is the synthetic vitamer of vitamin K?
Deficiency of which vitamin causes spinocerebellar ataxia?
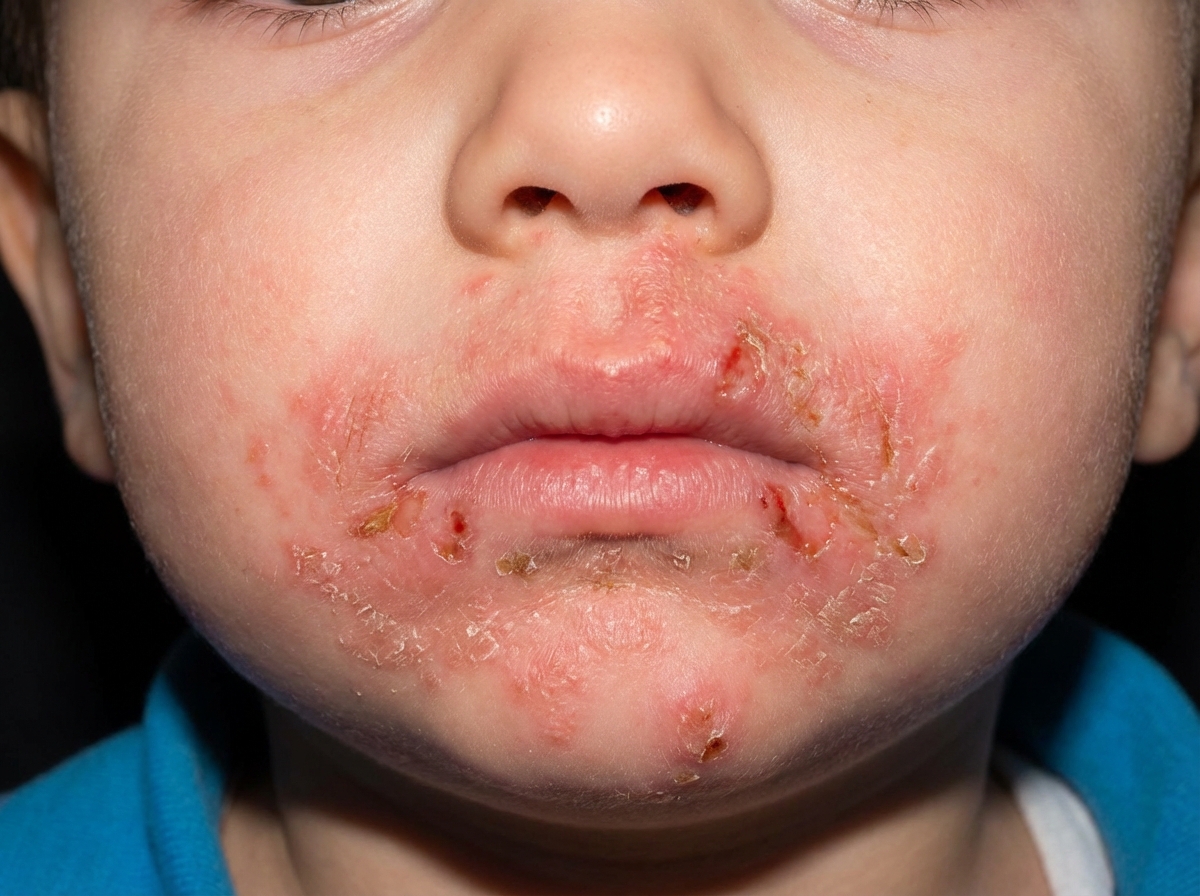
The given condition is caused due to deficiency of which of the following?
A constellation of neuropathy, muscle weakness and wasting, cardiomegaly, edema, and ophthalmoplegia strongly suggests which of the following deficiencies?
Thiamine status of an individual can be detected by which of the following tests/enzymes in erythrocytes?
Collagen formation is affected in the deficiency of which vitamin?
Practice by Chapter
Fat-Soluble Vitamins: A, D, E, K
Practice Questions
Vitamin A and Vision
Practice Questions
Vitamin D and Calcium Metabolism
Practice Questions
Vitamin E and Antioxidant Functions
Practice Questions
Vitamin K and Blood Coagulation
Practice Questions
Water-Soluble Vitamins: B Complex and C
Practice Questions
Thiamine (B1) and Pyruvate Dehydrogenase
Practice Questions
Riboflavin (B2) and Flavin Coenzymes
Practice Questions
Niacin and NAD/NADP
Practice Questions
Vitamin B6 and Transamination
Practice Questions
Folate and Vitamin B12 in One-Carbon Metabolism
Practice Questions
Vitamin C and Collagen Synthesis
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
