Vitamins and Coenzymes — MCQs

On this page
A patient presents with an inability to convert pyruvate to Acetyl CoA. Which of the following can be used in treatment?
A 4-year-old boy whose diet consists mostly of cheese puffs and cola presents with nyctalopia, xerosis, and headache. Which of the following vitamin or trace element replacement therapies is most appropriate to treat this condition?
Ultrasound examination of a developing fetus demonstrates a fluid-filled sac at the base of the fetus' spine that connects to the spinal canal and apparently contains part of the spinal cord. A dietary deficiency of which of the following is most strongly associated with this type of lesion?
Wernicke's encephalopathy in alcohol consumption can be treated with?
Which of the following statements about Vitamin D is correct?
Deficiency of which one of the following dietary components is most likely to have caused this rash?
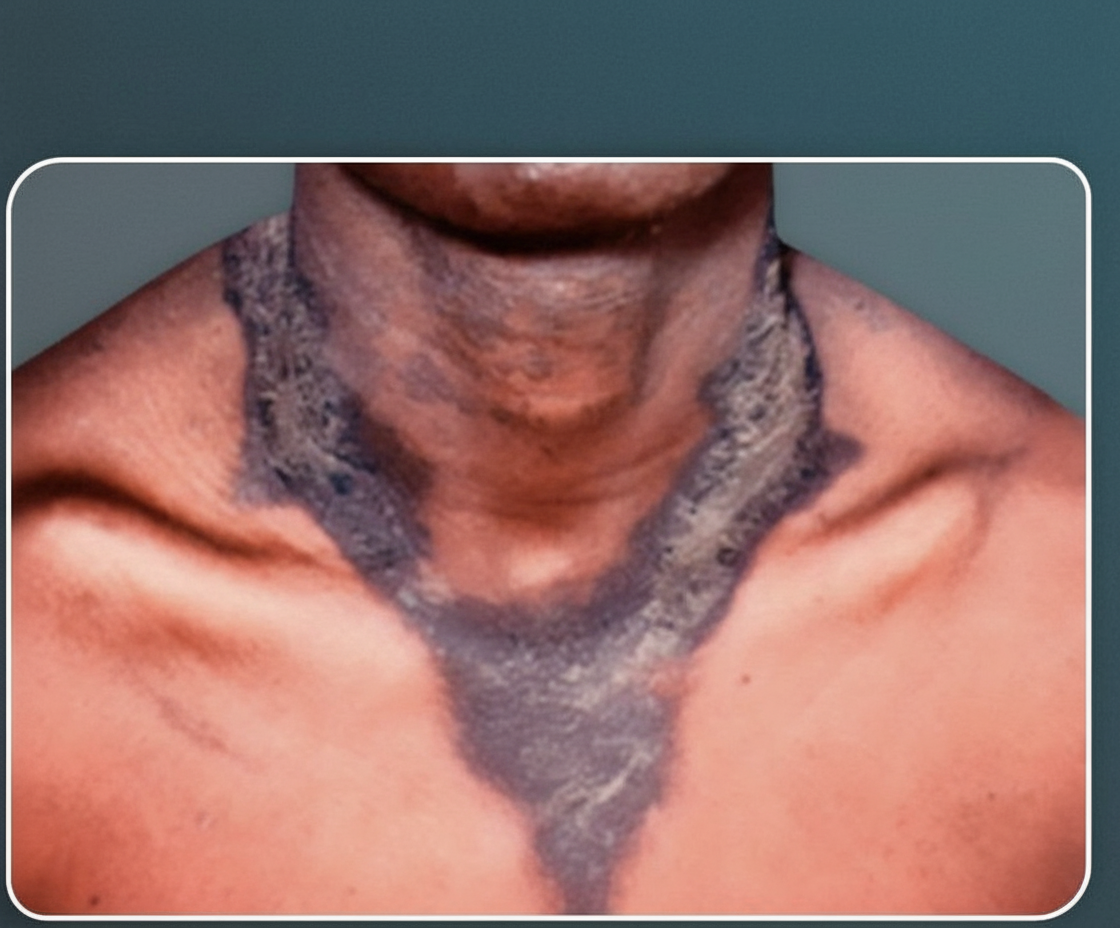
Absorption of vitamin A can be enhanced by giving the child a diet rich in which of the following?
Tryptophan is glucogenic and ketogenic by producing which of the following?
All of the following are antioxidants except?
Pellagra is a deficiency of which vitamin?
Practice by Chapter
Fat-Soluble Vitamins: A, D, E, K
Practice Questions
Vitamin A and Vision
Practice Questions
Vitamin D and Calcium Metabolism
Practice Questions
Vitamin E and Antioxidant Functions
Practice Questions
Vitamin K and Blood Coagulation
Practice Questions
Water-Soluble Vitamins: B Complex and C
Practice Questions
Thiamine (B1) and Pyruvate Dehydrogenase
Practice Questions
Riboflavin (B2) and Flavin Coenzymes
Practice Questions
Niacin and NAD/NADP
Practice Questions
Vitamin B6 and Transamination
Practice Questions
Folate and Vitamin B12 in One-Carbon Metabolism
Practice Questions
Vitamin C and Collagen Synthesis
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
