Vitamins and Coenzymes — MCQs

On this page
In pellagra, all are seen except?
Which pathway describes the synthesis of metabolically active vitamin D?
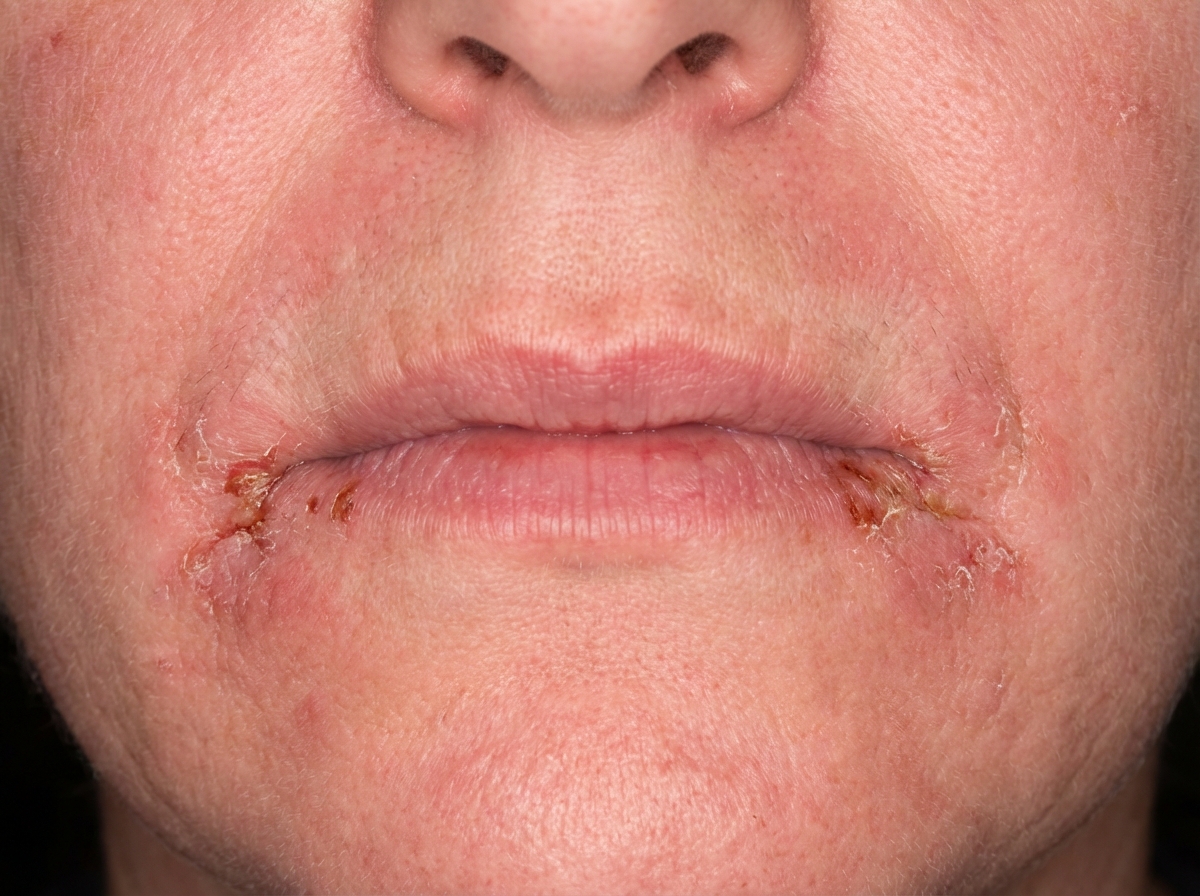
Which vitamin deficiency is most commonly responsible for this condition?
Absorption of vitamin K requires normal absorption of:
Transketolase requires which of the following as a cofactor?
Which element is required for the function of the enzyme group kinases?
Which of the following is NOT a form of Vitamin K?
Which nutritional deficiency is associated with hereditary ataxia?
Tocopherols are derivatives of which of the following?
Which vitamin deficiency disorder is associated with a diet primarily consisting of cereals?
Practice by Chapter
Fat-Soluble Vitamins: A, D, E, K
Practice Questions
Vitamin A and Vision
Practice Questions
Vitamin D and Calcium Metabolism
Practice Questions
Vitamin E and Antioxidant Functions
Practice Questions
Vitamin K and Blood Coagulation
Practice Questions
Water-Soluble Vitamins: B Complex and C
Practice Questions
Thiamine (B1) and Pyruvate Dehydrogenase
Practice Questions
Riboflavin (B2) and Flavin Coenzymes
Practice Questions
Niacin and NAD/NADP
Practice Questions
Vitamin B6 and Transamination
Practice Questions
Folate and Vitamin B12 in One-Carbon Metabolism
Practice Questions
Vitamin C and Collagen Synthesis
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
