Head — MCQs

On this page
Which of the following statements about the lateral pterygoid muscle is true?
Which of the following is most important in separating the esophagus from the larynx, and must consequently be carefully passed behind during endoscopy?
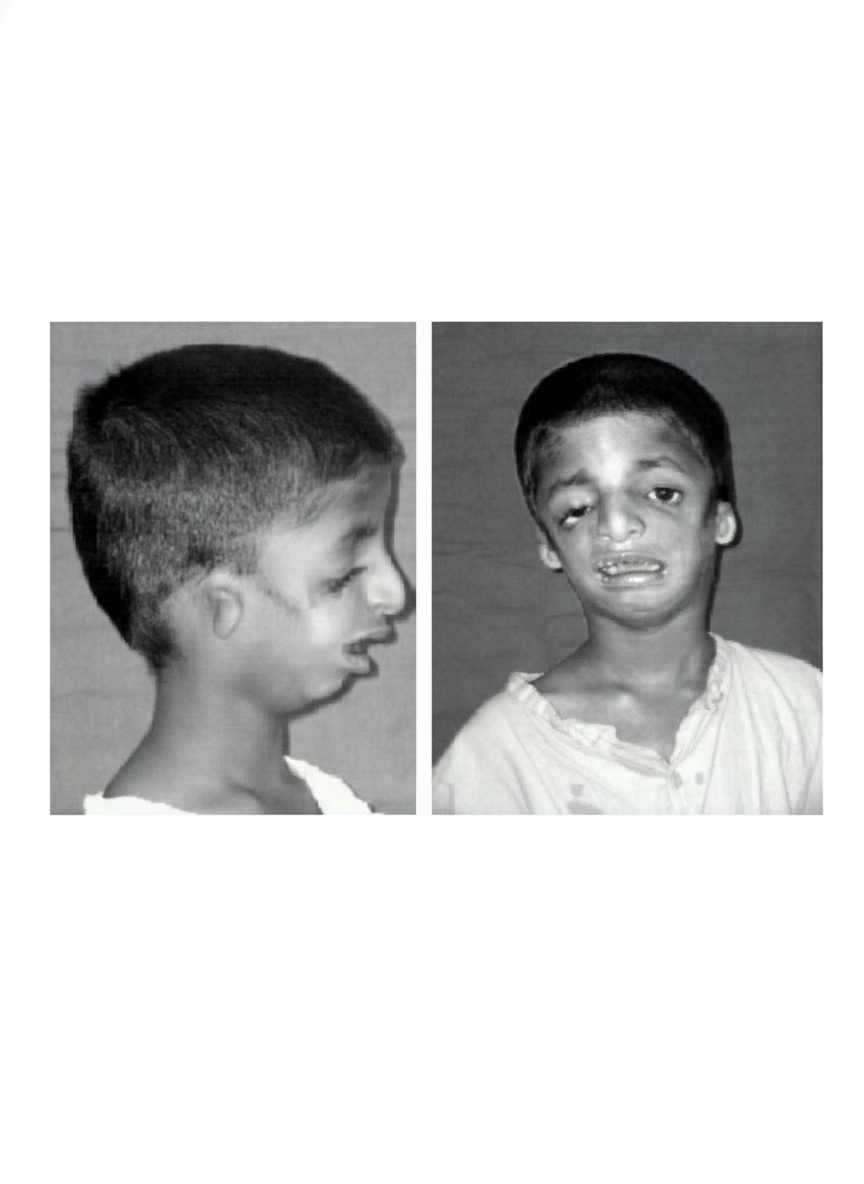
The image shows a patient with a congenital craniofacial condition. Which of the following is a striking feature of this condition?
Which of the following statements about the vertebral artery is/are true?
What is the length of the nasolacrimal duct?
According to Cawood and Howell, what is the classification for a depression with a cup-shaped surface of an edentulous atrophic maxilla?
What is true about the sphenoid sinus?
Which nerve supplies the muscles of the tongue?
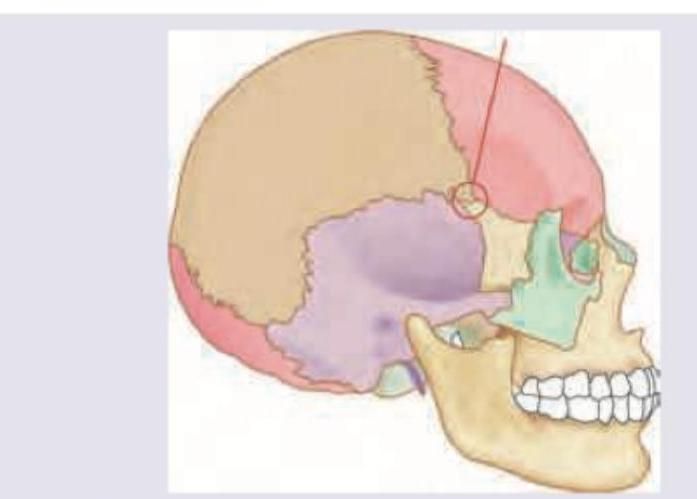
Injury to the marked area of the skull will cause intracranial hemorrhage due to damage to which artery?
Crocodile tears is due to abnormal regeneration of which nerve?
Practice by Chapter
Skull and Facial Bones
Practice Questions
Scalp and Facial Muscles
Practice Questions
Dural Venous Sinuses
Practice Questions
Cranial Cavity
Practice Questions
Orbit and Contents
Practice Questions
Temporal and Infratemporal Regions
Practice Questions
Pterygopalatine Fossa
Practice Questions
Oral Cavity
Practice Questions
Paranasal Sinuses
Practice Questions
Applied Anatomy and Clinical Correlations
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
