Head — MCQs

On this page
What is the primary lymphatic drainage site for the maxillary sinus?
All of the following are true about the middle ear cavity except?
What is the connecting vein between the facial vein and the cavernous sinus?
Fracture of the base of the skull may cause injury to the various cranial nerves, except:
Which of the following muscles of mastication has an opposite and independent function?
Which of the following cranial nerves does not contain parasympathetic motor (GVE) fibers?
Which nerve supplies the Muller muscle?
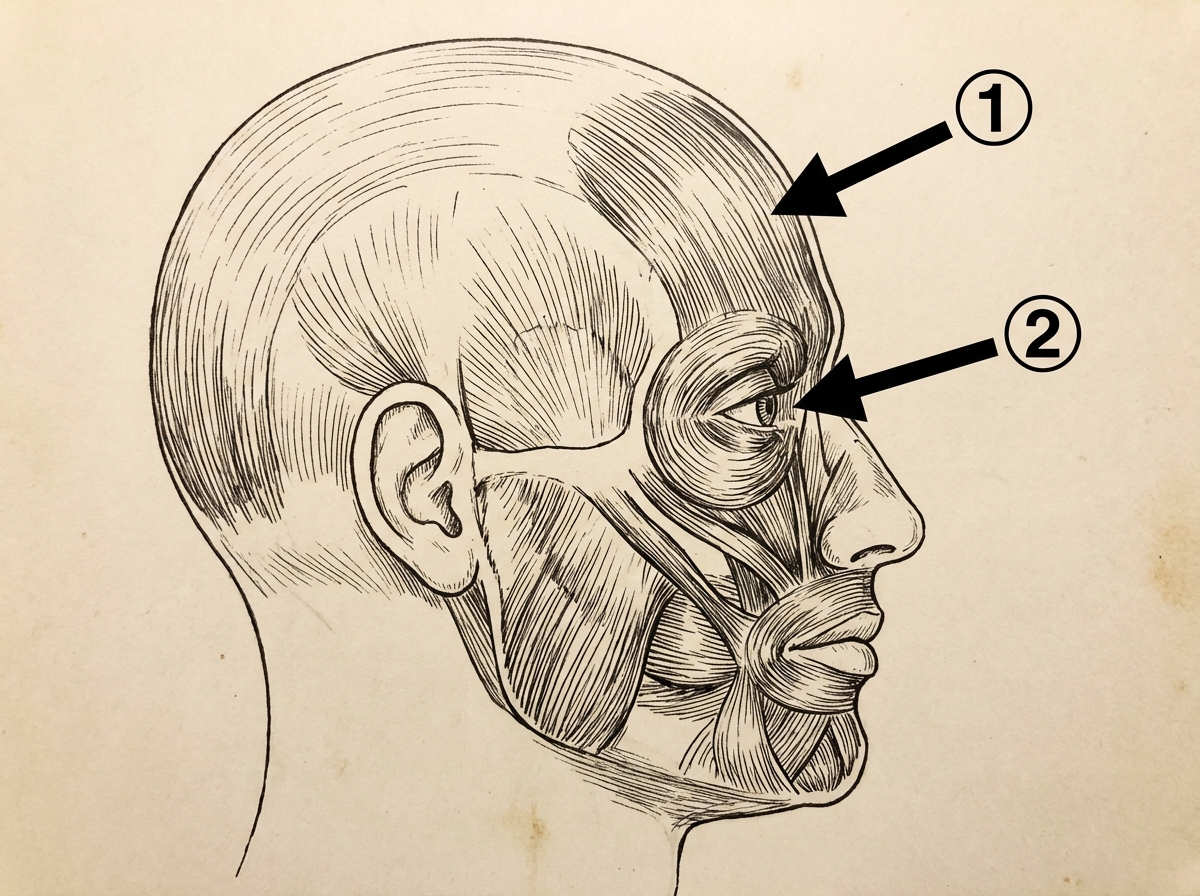
Which nerve supplies the muscle indicated by the second arrow?
What does the Greek letter lambda represent?
All of the following structures pierce the buccinator muscle, except:
Practice by Chapter
Skull and Facial Bones
Practice Questions
Scalp and Facial Muscles
Practice Questions
Dural Venous Sinuses
Practice Questions
Cranial Cavity
Practice Questions
Orbit and Contents
Practice Questions
Temporal and Infratemporal Regions
Practice Questions
Pterygopalatine Fossa
Practice Questions
Oral Cavity
Practice Questions
Paranasal Sinuses
Practice Questions
Applied Anatomy and Clinical Correlations
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
