Head — MCQs

On this page
What bones form the lateral orbital wall?
Which of the following nerves is also known as the Vidian nerve?
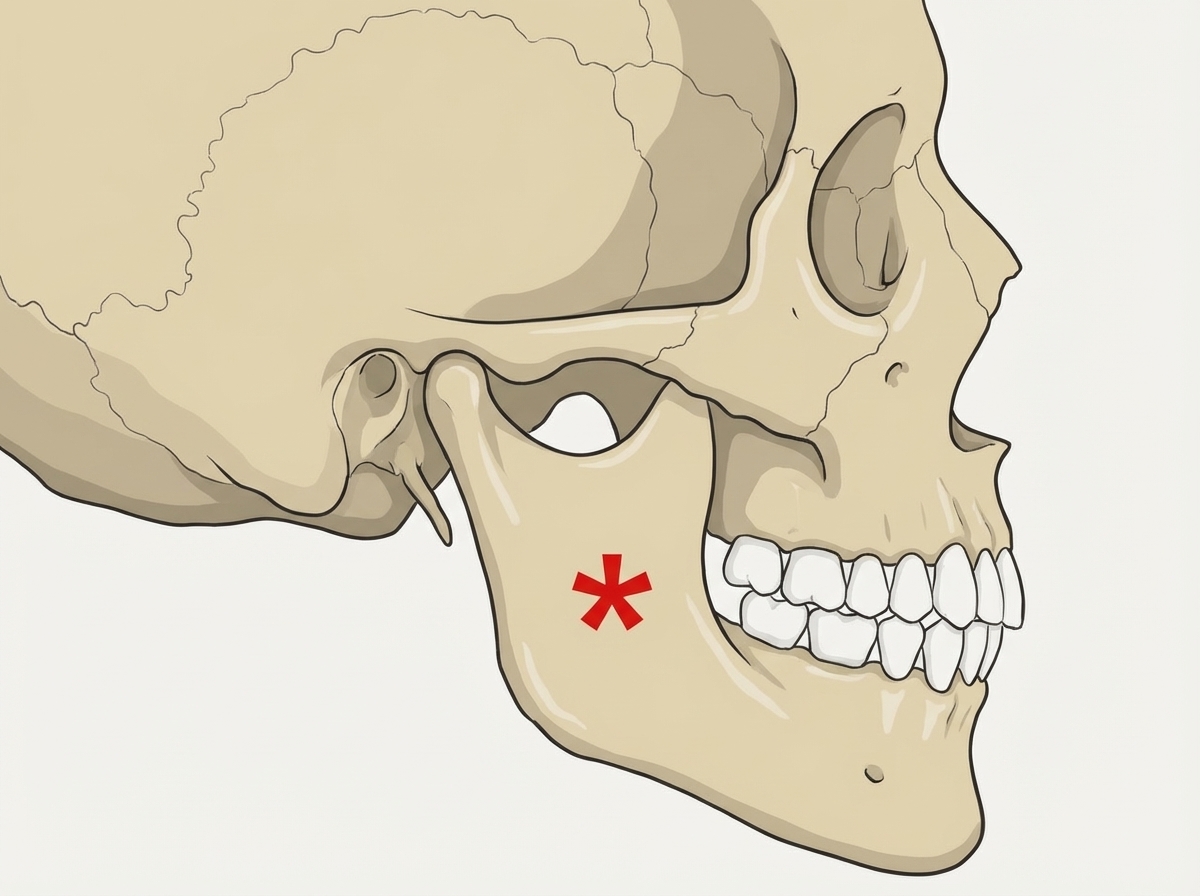
Identify the muscle attached to the marked area in the diagram.
Which extraocular muscle is NOT supplied by the oculomotor nerve?
The middle meningeal artery is related to which point on the skull?
The preganglionic parasympathetic fibres for the otic ganglion originate from which nucleus?
Which of the following does not drain into the submental lymph nodes?
Which cranial nerve carries pain sensations from the tip of the tongue?
Loss of corneal reflex is due to injury of which nerve or nerve division?
The facial artery terminates in an anastomosis with which of the following?
Practice by Chapter
Skull and Facial Bones
Practice Questions
Scalp and Facial Muscles
Practice Questions
Dural Venous Sinuses
Practice Questions
Cranial Cavity
Practice Questions
Orbit and Contents
Practice Questions
Temporal and Infratemporal Regions
Practice Questions
Pterygopalatine Fossa
Practice Questions
Oral Cavity
Practice Questions
Paranasal Sinuses
Practice Questions
Applied Anatomy and Clinical Correlations
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
