Head — MCQs

On this page
The concha and eminent concha are supplied by which nerve?
Which nerve to an extraocular muscle gives rise to a branch of the ciliary ganglion?
What is the main arterial supply to the tongue?
Which veins are NOT involved in spreading infection to the cavernous sinus from the danger area of the face?
All of the following statements about Sternberg Canal are true, except:
Which of the following is NOT a branch of the external carotid artery?
The nasal septum is supplied by all the following nerves except:
Which cranial nerve is shown in this diagram?
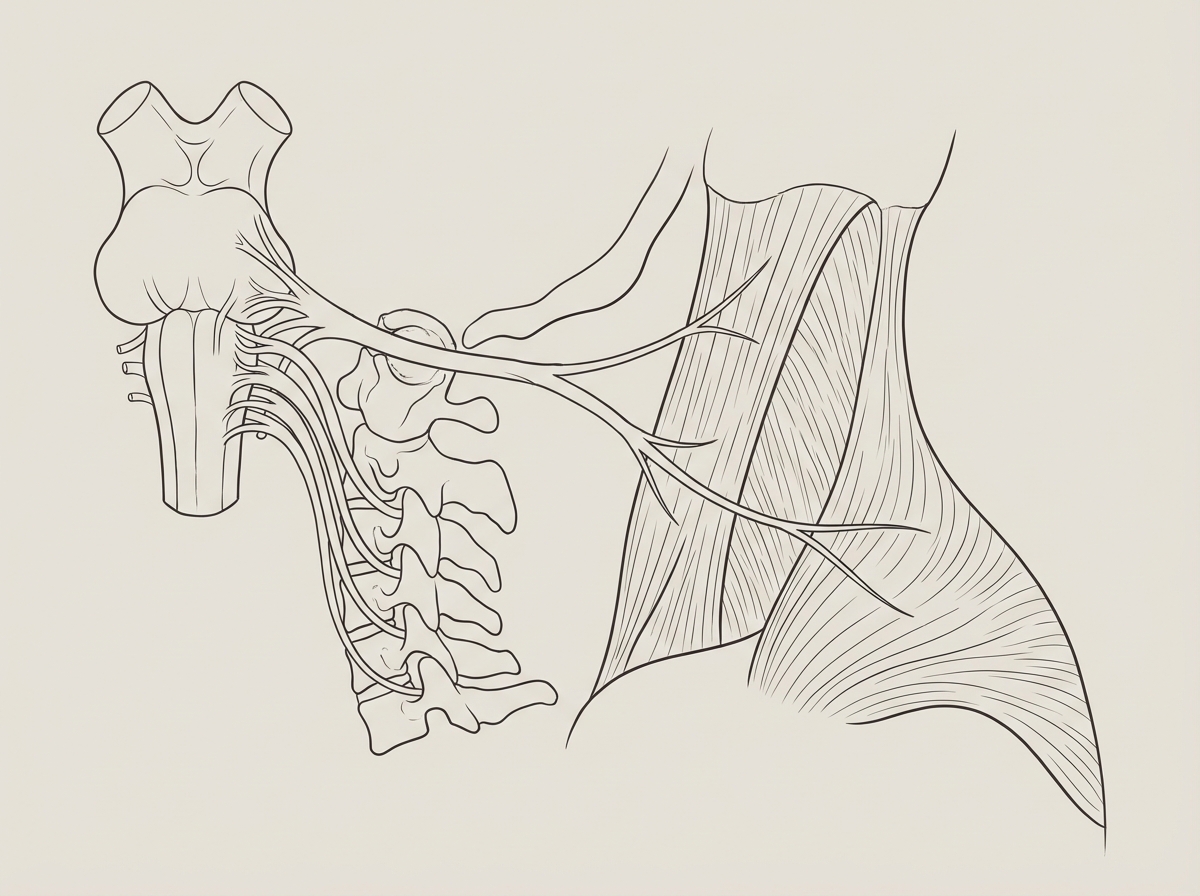
Which structure does not pass through the jugular foramen?
Which of the following bones are pneumatic?
Practice by Chapter
Skull and Facial Bones
Practice Questions
Scalp and Facial Muscles
Practice Questions
Dural Venous Sinuses
Practice Questions
Cranial Cavity
Practice Questions
Orbit and Contents
Practice Questions
Temporal and Infratemporal Regions
Practice Questions
Pterygopalatine Fossa
Practice Questions
Oral Cavity
Practice Questions
Paranasal Sinuses
Practice Questions
Applied Anatomy and Clinical Correlations
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
