Head — MCQs

On this page
A 47-year-old woman presents with signs of cavernous sinus thrombosis. Radiographic examination reveals a pituitary tumor involving the cavernous sinus. The tumor is suspected to have damaged the patient's right abducens nerve. In which direction will the physician most likely ask the patient to turn her right eye to confirm the abducens nerve damage, assuming she is unable to perform this task?
Which bone does not contribute to the medial wall of the orbit?
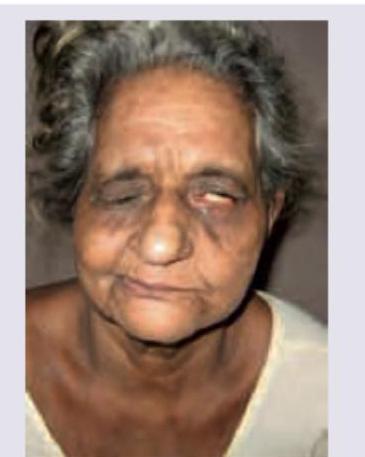
The structure damaged in the given condition is responsible for all except:
The lambda is the meeting point of which sutures?
Which nerve crosses the submandibular gland?
Damage to the middle meningeal artery typically results in which type of intracranial hemorrhage?
Which of the following extraocular muscles does not arise from the annulus of Zinn?
Ptosis is due to which of the following?
What overlies the lateral wall of the mastoid antrum?
Which of the following is NOT a terminal branch of the facial nerve?
Practice by Chapter
Skull and Facial Bones
Practice Questions
Scalp and Facial Muscles
Practice Questions
Dural Venous Sinuses
Practice Questions
Cranial Cavity
Practice Questions
Orbit and Contents
Practice Questions
Temporal and Infratemporal Regions
Practice Questions
Pterygopalatine Fossa
Practice Questions
Oral Cavity
Practice Questions
Paranasal Sinuses
Practice Questions
Applied Anatomy and Clinical Correlations
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
