UPSC-CMS 2012 — Community Medicine
16 Previous Year Questions with Answers & Explanations
Consider the following statements : HIV can be transmitted to a healthcare worker from a patient through : 1. A needle stick injury 2. Contact with the patient's blood 3. External examination of the patient 4. Inhalation Which of the statements given above is/are correct ?
A Health Assistant (Male) covers a population of
Case Fatality Rate of a disease is a measure of its
The incubation period of mumps is
Which of the following specialists is mandatory at a Community Health Centre as per IPHS guidelines?
In a normal curve, how much per cent of the values will be included in the area between two standard deviations on either side of the mean (X ± 2σ) ?
The ability of a test to identify correctly those who do not have the disease is called its
The Relative Risk of a disease measures the
Match List-I with List-II and select the correct answer using the code given below the Lists:

Match List-I with List-II and select the correct answer using the code given below the Lists:
UPSC-CMS 2012 - Community Medicine UPSC-CMS Practice Questions and MCQs
Question 1: Consider the following statements : HIV can be transmitted to a healthcare worker from a patient through : 1. A needle stick injury 2. Contact with the patient's blood 3. External examination of the patient 4. Inhalation Which of the statements given above is/are correct ?
- A. 1 and 2 only (Correct Answer)
- B. 2 and 3 only
- C. 1 and 4
- D. 1, 2 and 3
Explanation: ***1 and 2 only*** - **Needle stick injuries** pose a significant risk as they involve direct inoculation of infected blood into the healthcare worker's bloodstream. - **Contact with a patient's blood** can lead to transmission if there are cuts, abrasions, or mucous membrane exposures on the healthcare worker. *2 and 3 only* - **Contact with a patient's blood** is a known transmission route, but **external examination** alone, without blood contact or needle stick, typically carries no risk of HIV transmission. - HIV is not transmitted through casual contact or touch during an examination. *1 and 4* - **Needle stick injuries** are a recognized transmission route, but **inhalation** is not a mechanism for HIV transmission. - HIV is not an airborne virus and does not spread like respiratory illnesses. *1, 2 and 3* - While **needle stick injuries** and **contact with blood** are clear transmission pathways, **external examination** of a patient, in the absence of blood contact or needle stick injuries, does not transmit HIV. - HIV transmission requires specific fluid exchange (blood, semen, vaginal fluids, breast milk) entering the bloodstream or mucous membranes.
Question 2: A Health Assistant (Male) covers a population of
- A. 1,000
- B. 30,000 (Correct Answer)
- C. 5,000
- D. 1,00,000
Explanation: ***Correct Answer: 30,000*** - A Health Assistant (Male), also known as a **Multi-Purpose Worker (Male) [MPW(M)]**, is responsible for a population of **30,000** in a rural plain area. - Their duties include assisting with family planning, maternal and child health, immunization, and communicable disease control programs. - This is the standard population norm as per **Indian Public Health Standards (IPHS)**. *Incorrect Option: 1,000* - A population of **1,000** is typically covered by an **Accredited Social Health Activist (ASHA)**, who operates at the village level. - ASHAs are community health workers primarily focused on mobilizing the community for health services and providing basic health education. - This represents a much smaller coverage area than Health Assistant (Male). *Incorrect Option: 5,000* - A **Sub-Centre**, the most peripheral and first contact point between the primary health care system and the community, covers a population of **5,000 in plain areas** and **3,000 in hilly/tribal areas**. - Sub-Centre is staffed by one ANM (Auxiliary Nurse Midwife) and one Male Health Worker. - This is the coverage for a health facility, not specifically for Health Assistant (Male). *Incorrect Option: 1,00,000* - A **Community Health Centre (CHC)** serves as a referral unit for **4-5 Primary Health Centres** and covers a population of **80,000 to 1.2 lakh** in plain areas. - CHCs provide specialist services like obstetrics and gynecology, surgery, pediatrics, and emergency services. - This represents the coverage of a referral-level health facility, much larger than Health Assistant (Male) coverage.
Question 3: Case Fatality Rate of a disease is a measure of its
- A. Chronicity
- B. Endemicity
- C. Infectivity
- D. Virulence (Correct Answer)
Explanation: ***Virulence*** - **Case fatality rate (CFR)** is defined as the proportion of persons with a disease who **die from that disease**. - It directly reflects the **severity** or **lethality** of a disease among those infected. - A higher CFR indicates that the disease is more **virulent**, causing a greater proportion of infected individuals to die. - CFR is the standard epidemiological measure of **virulence**. *Chronicity* - **Chronicity** refers to the **duration** of a disease, indicating whether it is long-lasting or recurrent. - It does not directly measure the disease's ability to cause death among those infected. *Endemicity* - **Endemicity** describes the **constant presence** and/or usual prevalence of a disease in a geographic area or population. - This term relates to the typical occurrence pattern, not the deadliness of the disease. *Infectivity* - **Infectivity** is the ability of an organism to **cause infection** in a susceptible host. - It measures how easily an agent can spread and establish itself, not its capacity to cause severe disease or death.
Question 4: The incubation period of mumps is
- A. 2-3 weeks (Correct Answer)
- B. 4-5 weeks
- C. 1-2 weeks
- D. 3-4 weeks
Explanation: ***2-3 weeks*** - The incubation period for **mumps** is typically 16 to 18 days, with a range of 12 to 25 days, which falls within the 2-3 week timeframe. - This period is the time from exposure to the mumps virus until the onset of symptoms, such as **parotitis**. *4-5 weeks* - An incubation period of 4-5 weeks is longer than the typical range for mumps, suggesting a different viral infection. - This duration is more characteristic of diseases like **hepatitis B** rather than mumps. *1-2 weeks* - An incubation period of 1-2 weeks is shorter than the typical range for mumps. - This timeframe is more commonly associated with various **respiratory viruses** or **influenza**. *3-4 weeks* - While 3-4 weeks (21-28 days) can include the upper end of the mumps incubation period, it is not the most common or typical duration. - The average incubation is closer to **2.5 weeks**, making 2-3 weeks the more accurate general range.
Question 5: Which of the following specialists is mandatory at a Community Health Centre as per IPHS guidelines?
- A. Surgery
- B. Paediatrics (Correct Answer)
- C. Obstetrics and Gynaecology
- D. Dermatology and Venereology
Explanation: ***Paediatrics*** - As per **Indian Public Health Standards (IPHS)** guidelines for Community Health Centres (CHCs), a **Paediatrician** is one of the **four mandatory specialists** required at CHCs. - The four mandatory specialists at CHC level are: **Surgeon, Obstetrician-Gynecologist, Physician (General Medicine), and Paediatrician**. - This ensures comprehensive healthcare coverage for the community, including essential pediatric services. *Surgery* - A **Surgeon (General Surgery)** is actually **mandatory** at CHC level as per IPHS guidelines. - This is one of the four required specialist positions at CHCs. - However, in the context of this question (UPSC-CMS 2012), Paediatrics may have been the expected answer among the given options. *Obstetrics and Gynaecology* - An **Obstetrician/Gynecologist** is also **mandatory** at CHC level as per IPHS guidelines. - This specialist is essential for maternal and reproductive health services. - Like Surgery, this is one of the four required specialists at CHCs. *Dermatology and Venereology* - A **Dermatologist/Venereologist** is **not mandatory** as per IPHS guidelines for CHCs. - Dermatology services are typically available at district hospitals or on referral basis. - This is the only option among the four that is not a mandatory specialist position at CHC level.
Question 6: In a normal curve, how much per cent of the values will be included in the area between two standard deviations on either side of the mean (X ± 2σ) ?
- A. 68.3
- B. 90.4
- C. 95.4 (Correct Answer)
- D. 99.7
Explanation: ***Correct: 95.4*** - According to the **empirical rule** (also known as the 68-95-99.7 rule), approximately 95% of data falls within two standard deviations of the mean in a normal distribution. - More precisely, the area between **X ± 2σ** encompasses **95.4%** of the values. - This is a fundamental concept in biostatistics used for calculating confidence intervals and reference ranges. *Incorrect: 68.3* - This percentage represents the proportion of data within **one standard deviation** (X ± 1σ) of the mean in a normal distribution. - It is not the correct value for the range of two standard deviations. *Incorrect: 90.4* - This value does not correspond to any standard interval of standard deviations around the mean in a normal distribution. - It is not part of the empirical rule for common standard deviation ranges. *Incorrect: 99.7* - This percentage represents the proportion of data within **three standard deviations** (X ± 3σ) of the mean in a normal distribution. - It is a larger interval than what is asked in the question (two standard deviations).
Question 7: The ability of a test to identify correctly those who do not have the disease is called its
- A. Sensitivity
- B. Positive predictive value
- C. Specificity (Correct Answer)
- D. Negative predictive value
Explanation: ***Specificity*** - **Specificity** is the proportion of **true negatives** correctly identified by the test. - It measures the ability of a test to correctly identify individuals who **do not have the disease**. *Sensitivity* - **Sensitivity** is the proportion of **true positives** correctly identified by the test. - It measures the ability of a test to correctly identify individuals who **do have the disease**. *Positive predictive value* - **Positive predictive value (PPV)** is the probability that a patient with a **positive test result** actually has the disease. - It depends on the **prevalence** of the disease in the population being tested. *Negative predictive value* - **Negative predictive value (NPV)** is the probability that a patient with a **negative test result** actually does not have the disease. - It also depends on the **prevalence** of the disease in the population.
Question 8: The Relative Risk of a disease measures the
- A. Strength of association between suspected cause and effect (Correct Answer)
- B. Biological plausibility between suspected cause and effect
- C. Temporal relationship between suspected cause and effect
- D. Specificity of association between suspected cause and effect
Explanation: ***Strength of association between suspected cause and effect*** - **Relative Risk (RR)** quantifies how much more likely an exposed group is to develop an outcome compared to an unexposed group, directly indicating the **strength of association**. - An RR of 1 means no association, an RR > 1 suggests increased risk, and an RR < 1 suggests protection, demonstrating the **magnitude of the relationship**. *Biological plausibility between suspected cause and effect* - **Biological plausibility** refers to the coherence of a hypothesis with existing biological and medical knowledge. - While it's a criterion for causal inference, **Relative Risk** itself measures statistical association, not the underlying biological mechanism. *Temporal relationship between suspected cause and effect* - The **temporal relationship** (cause precedes effect) is a crucial criterion for causality but is not directly measured by **Relative Risk**. - **Relative Risk** evaluates risk at a given point or over a period, assuming exposure has already occurred. *Specificity of association between suspected cause and effect* - **Specificity of association** suggests that a single exposure is linked to a single disease, which is rarely true in complex biological systems. - **Relative Risk** quantifies association without implying one-to-one causation or absence of other contributing factors.
Question 9: Match List-I with List-II and select the correct answer using the code given below the Lists:
- A. A→4 B→3 C→2 D→1
- B. A→4 B→2 C→3 D→1
- C. A→1 B→2 C→3 D→4
- D. A→4 B→2 C→1 D→3 (Correct Answer)
Explanation: ***A→4 B→2 C→1 D→3*** - This option correctly matches each committee with its primary recommendation contributing to the evolution of healthcare in India. - The **Bhore Committee** recommended **three months' training in PSM for doctors** to address basic healthcare needs, the **Mudaliar Committee** focused on **strengthening district hospitals**, the **Kartar Singh Committee** proposed the development of a **referral services complex**, and the **Srivastava Committee** suggested replacing ANMs with **female health workers**. *A→4 B→3 C→2 D→1* - This option incorrectly associates the **Mudaliar Committee** with replacing ANMs and the **Kartar Singh Committee** with strengthening district hospitals. - While both committees made significant recommendations, their specific focus areas were different from what is listed here. *A→4 B→2 C→3 D→1* - This option incorrectly links the **Kartar Singh Committee** with replacing ANMs and the **Srivastava Committee** with developing a referral services complex. - The **Kartar Singh Committee** focused on providing a comprehensive referral system, while the **Srivastava Committee** emphasized the creation of multi-purpose health workers. *A→1 B→2 C→3 D→4* - This option incorrectly matches the **Bhore Committee** with developing a referral services complex and the **Srivastava Committee** with training in PSM for doctors. - The **Bhore Committee**, formed in the 1940s, had a broader vision for healthcare infrastructure and medical education, while the **Srivastava Committee** focused on health personnel rationalization.
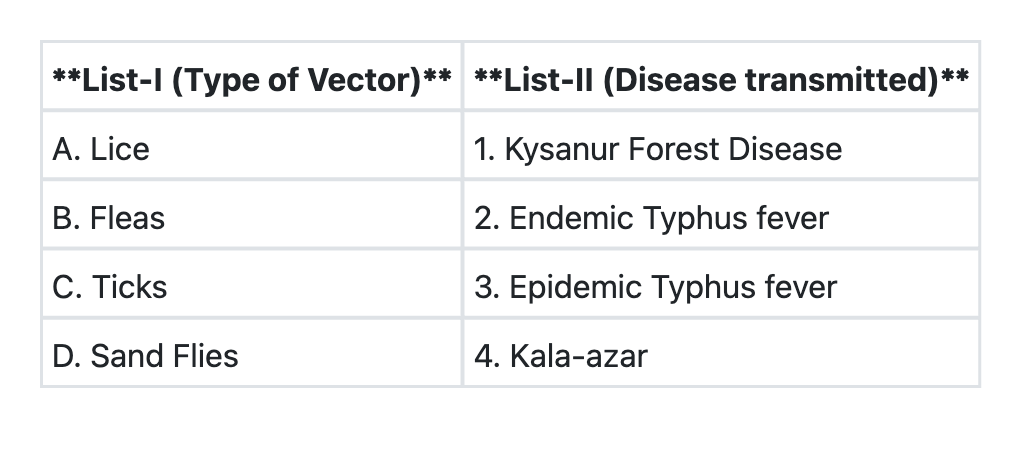
Question 10: Match List-I with List-II and select the correct answer using the code given below the Lists:
- A. A→1 B→2 C→4 D→3
- B. A→3 B→2 C→4 D→1
- C. A→3 B→2 C→1 D→4 (Correct Answer)
- D. A→2 B→1 C→3 D→4
Explanation: ***Correct Answer: A→3 B→2 C→1 D→4*** This option correctly matches each vector with its transmitted disease: - **A (Lice) → 3 (Epidemic Typhus fever)** - *Pediculus humanus corporis* transmits *Rickettsia prowazekii* - **B (Fleas) → 2 (Endemic Typhus fever)** - *Xenopsylla cheopis* transmits *Rickettsia typhi* - **C (Ticks) → 1 (Kyasanur Forest Disease)** - *Haemaphysalis* ticks transmit KFD virus - **D (Sand Flies) → 4 (Kala-azar)** - *Phlebotomus* species transmit *Leishmania donovani* Understanding these specific vector-disease pairings is crucial for epidemiology, disease surveillance, and vector control programs in public health. *Incorrect: A→1 B→2 C→4 D→3* - Incorrectly pairs **Lice with Kyasanur Forest Disease** (should be Epidemic Typhus) and **Ticks with Kala-azar** (should be KFD) - KFD is tick-borne, not transmitted by sand flies; Kala-azar is sand fly-borne, not tick-borne *Incorrect: A→3 B→2 C→4 D→1* - Incorrectly pairs **Ticks with Kala-azar** (should be KFD) and **Sand Flies with Kyasanur Forest Disease** (should be Kala-azar) - Reverses the correct tick and sand fly disease associations *Incorrect: A→2 B→1 C→3 D→4* - Multiple errors: **Lice with Endemic Typhus** (should be Epidemic), **Fleas with KFD** (should be Endemic Typhus), and **Ticks with Epidemic Typhus** (should be KFD) - Confuses both typhus types and mismatches the tick-borne disease entirely