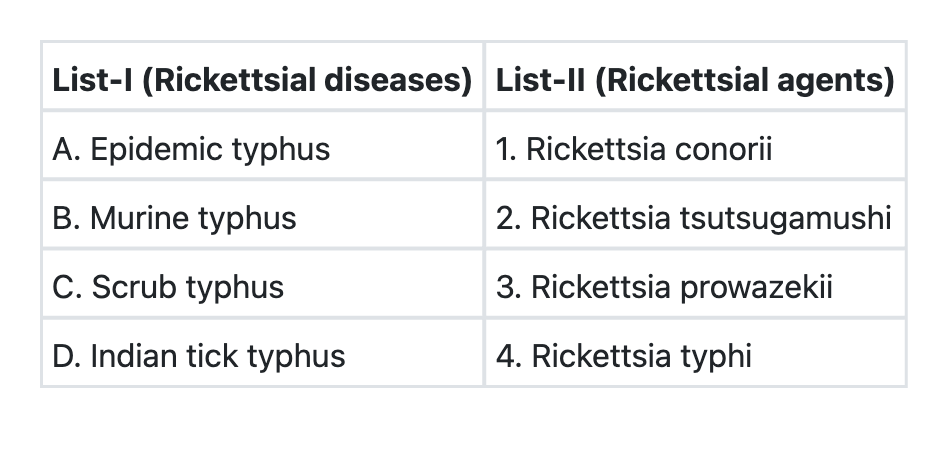
Match List-I with List-II and select the correct answer using the code given below the Lists:
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
Biochemical screening of newborn infants by heel-prick blood samples is performed by using the
What is the most cost-effective screening for identifying carcinoma cervix in a population?
Consider the following : 1. Hepatitis A outbreak 2. Polio outbreak 3. Gonorrhoea outbreak through prostitution Which of the above-listed outbreaks is/are classified under propagated epidemics?
What is the Body Mass Index of a person 150 cm tall and weighing 67.5 kg?
Consider the following indices : 1. Chandelier index 2. Sullivan's index 3. Waist-hip index 4. Ponderal index Which of the above is/are used for measuring obesity?
Which is the most common cause of mortality in infants between one and twelve months of age in India?
The cut-off standard for defining low birth-weight babies in India is considered to be
Match List-I with List-II and select the correct answer using the code given below the Lists:

Consider the following : 1. Night blindness 2. Corneal xerosis 3. Conjunctival xerosis 4. Keratomalacia What is the correct sequence of the above in the progress of clinical presentation of vitamin A deficiency blindness?
With reference to the role of fibre in diet, consider the following statements: 1. It inhibits faecal mutagen synthesis. 2. It reduces post-prandial glucose. 3. It decreases the transit time of food in the bowel. Which of the above represent(s) the role of fibre in our diet?