Match List-I with List-II and select the correct answer using the code given below the Lists:
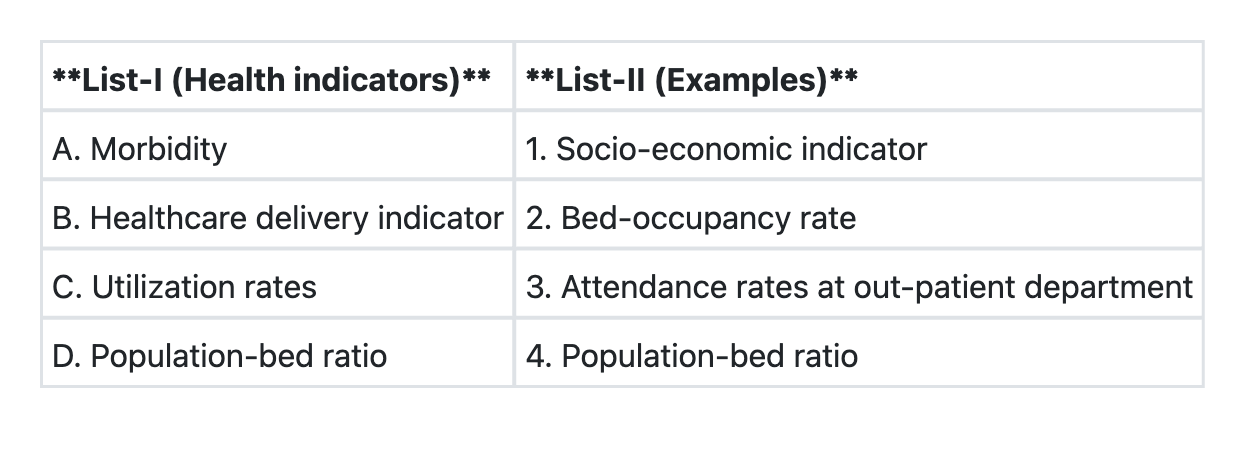
Winslow's definition of public health does not include which one of the following concepts?
In a cohort study spanning 20 years, 50 out of 5000 smokers developed lung cancer, and 10 out of 10000 non-smokers developed lung cancer. What is the 'relative risk' among smokers for developing lung cancer?
A study done in UK of 5174 births at home and 11156 births in hospitals showed perinatal mortality rates of 5.4/1000 in home births and 27.8/1000 in hospital births. What kind of Association is this?