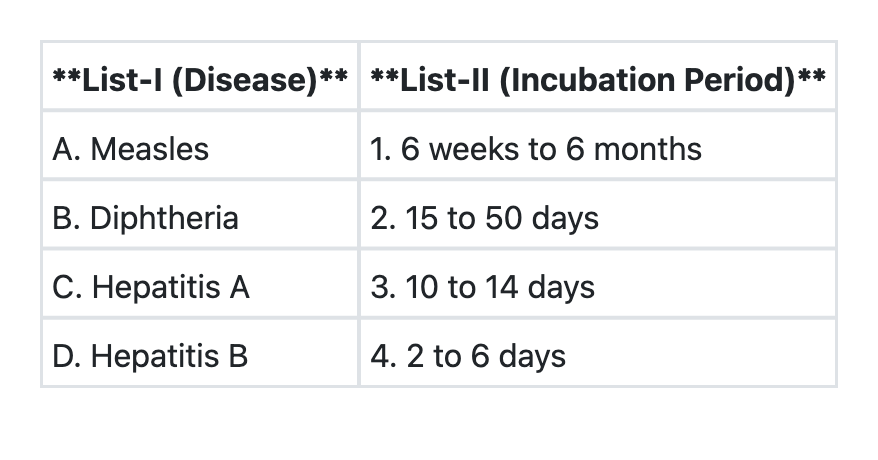
Match the diseases in List-I with their respective incubation periods in List-II and select the correct answer using the code given below:
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
Match the diseases in List-I with their respective incubation periods in List-II and select the correct answer using the code given below:

The "fern pattern" of cervical mucus seen in the first half of menstrual cycle is because of
Polycystic ovarian syndrome is associated with the following except
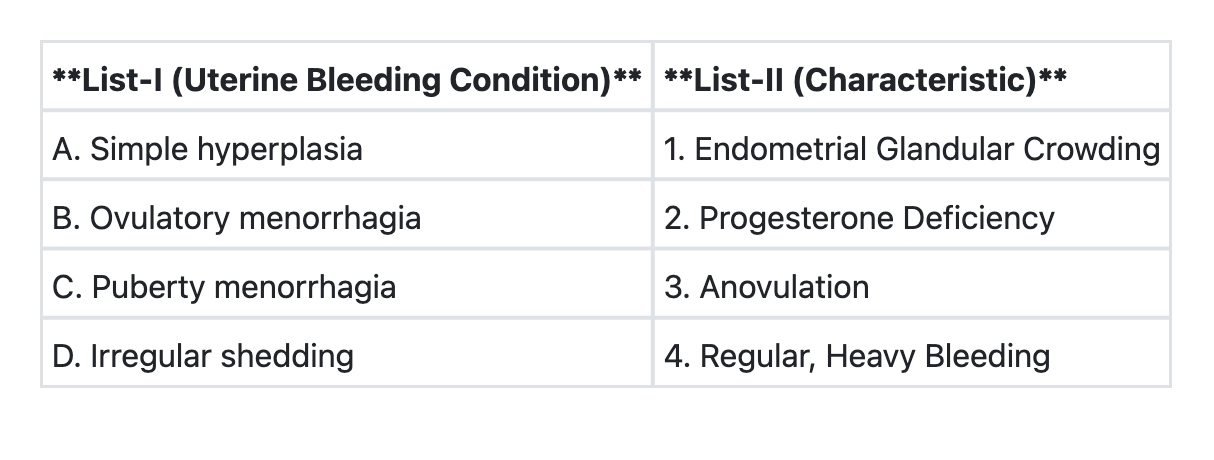
Match List-I with List-II and select the correct answer using the code given below the Lists:

Match List-I with List-II and select the correct answer using the code given below the Lists:

The most appropriate management of a 32 weeks pregnant lady with carcinoma cervix stage IIb is.
Safe period is calculated by
Which of the following is not related to the use of Levonorgestrel releasing intra-uterine contraceptive device ?
Combined oral pills protect the woman against all except
Which of these can be used for uterine artery embolization for fibroid uterus?