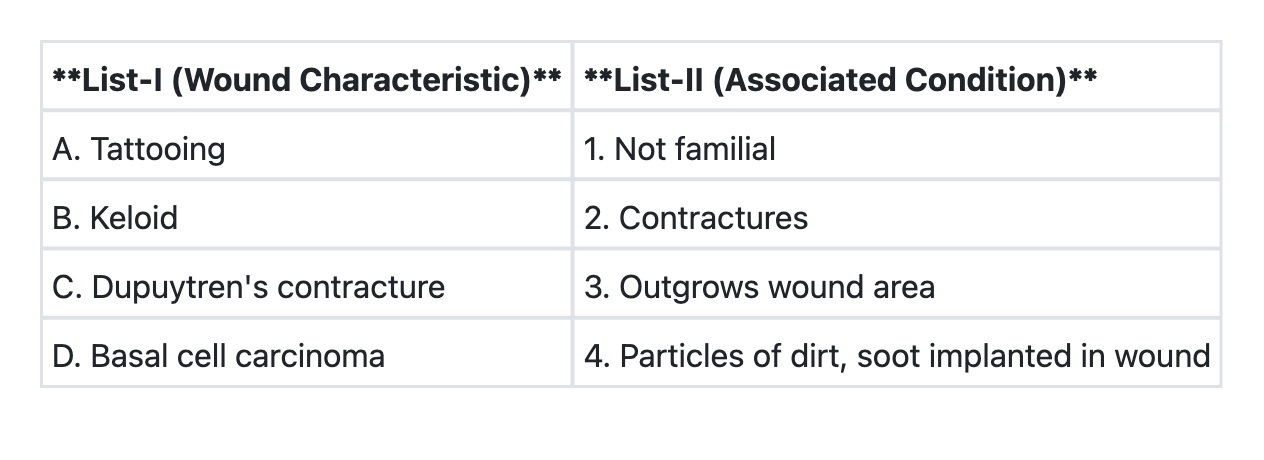
Match List-I with List-II and select the correct answer using the code given below the Lists: (Refer to the image for List-I and List-II)
Which of the following is the best indicator of prognosis of soft tissue sarcoma?
Lympho-venous anastomosis is done for
Which one of the following statements is not correct regarding thoracic outlet syndrome?