All SubjectsAnatomy (1)Anatomy (23)Anesthesiology (9)Biochemistry (23)Community Medicine (11)Dermatology (15)ENT (5)Forensic Medicine (4)General Medicine (2)Internal Medicine (39)Microbiology (19)Obstetrics and Gynecology (16)Ophthalmology (7)Orthopaedics (6)Pathology (19)Pathology (1)Pediatrics (11)Pharmacology (40)Physiology (13)Psychiatry (2)Psychiatry (5)Radiology (8)Surgery (15)
Q11
A patient presents with a gradually progressive, painless mass persisting for 10 years. The mass is firm to nodular and shows variable consistency within different areas of the swelling. What is the most probable diagnosis?
Q12
Dohlman surgery in Zenker's diverticulum is:-
Q13
Cushing ulcers are:-
Q14
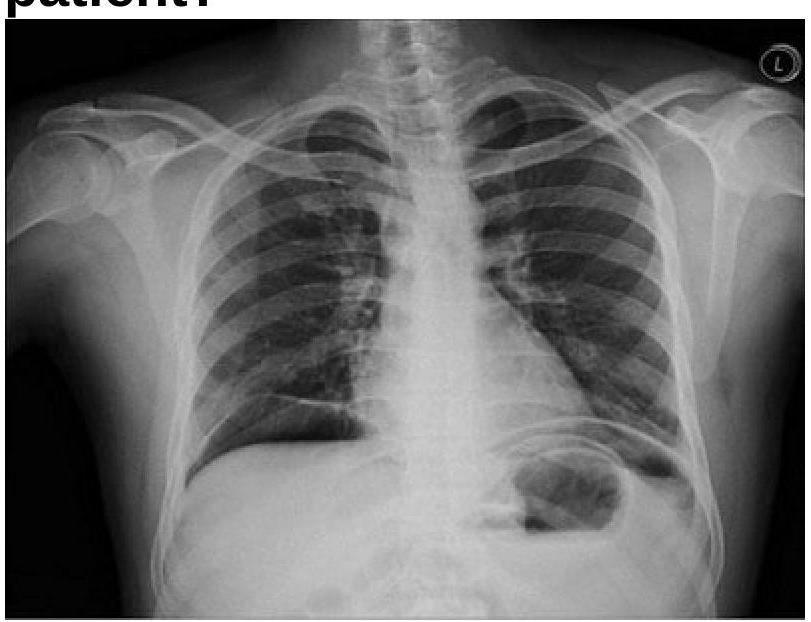
A 40 years old male was brought emergency with severe abdominal pain. On examination, pulse rate was 112/minute and systolic BP was 80 mmHg. Chest x-ray is given below. What is the most appropriate management?
Q15
Which of the following is true about tenosynovitis of the finger?