A 20-year-old alcoholic malnourished patient presented to the hospital with respiratory distress. His pulse was 112/minute. The patient had edema, hypertension, a systolic murmur along the left sternal edge, and bilateral crepitations in the lungs. A diagnosis of congestive high-output cardiac failure was made. Which vitamin is deficient?
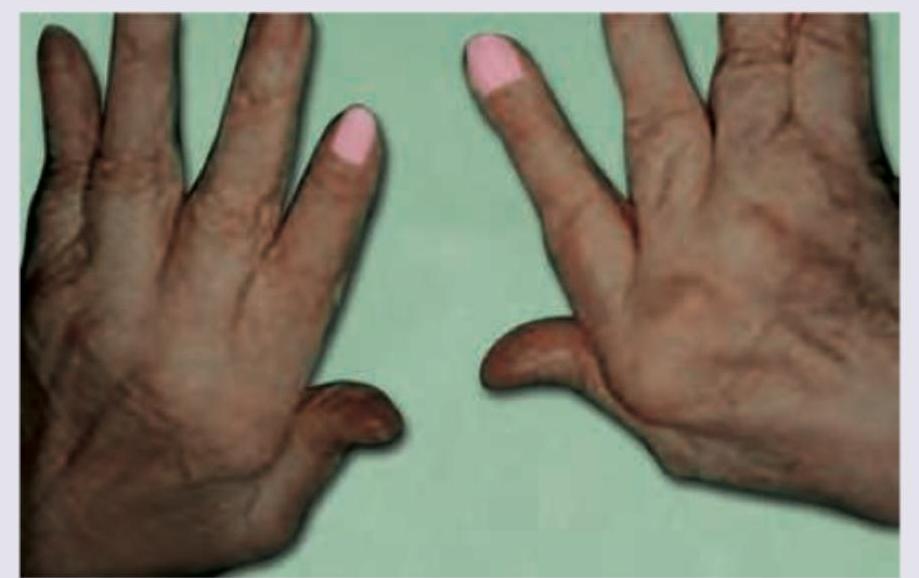
A 55-year-old female on methotrexate presents with continuous pain and swelling of bilateral hand joints. What is the best treatment plan for this patient?