A 25-year-old female presented to ER unconscious. Her mother tells you about her having recurrent syncopal episodes. Her BP is 80/60 mm Hg and you order an ECG. Treatment is

Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
Depth of Anesthesia is best measured by:
Retinitis pigmentosa is associated with deficiency of:
A 25-year-old female presented to ER unconscious. Her mother tells you about her having recurrent syncopal episodes. Her BP is 80/60 mm Hg and you order an ECG. Treatment is

McCallum patches/plaques are usually seen in which chamber of the heart?
False statement about Barrett esophagus is:
Drug of choice for Digoxin induced Ventricular Tachycardia:
Drug inhibiting granulocyte migration is:-
Cilastatin is given in combination with Imipenem because:-
All are true about Decerebrate posture except:-
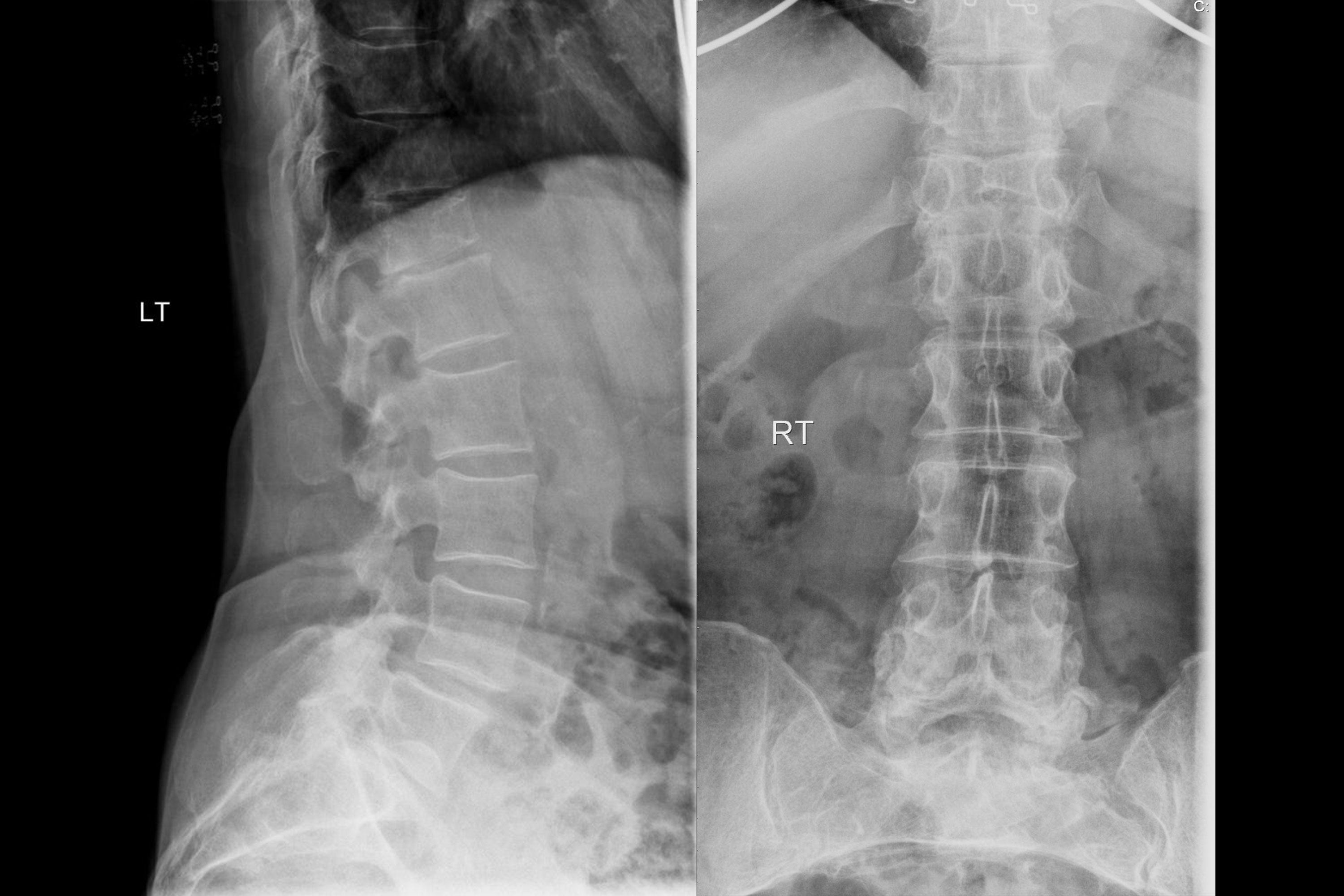
A 75-year-old female has chronic backache. X-ray of the spine is shown. What is the most likely diagnosis?