All (294)Anatomy (1)Anatomy (22)Anesthesiology (9)Biochemistry (26)Community Medicine (9)Dermatology (13)ENT (6)Forensic Medicine (5)General Medicine (1)Internal Medicine (33)Microbiology (23)Obstetrics and Gynecology (13)Ophthalmology (9)Orthopaedics (6)Pathology (23)Pathology (1)Pediatrics (13)Pharmacology (37)Physiology (15)Psychiatry (2)Psychiatry (4)Radiology (7)Surgery (16)
Q151
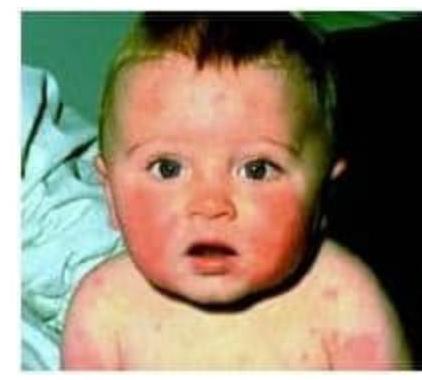
Identify the condition in the image