Which murmur increases on standing?
Most characteristic cardiovascular defect seen in Rubella-
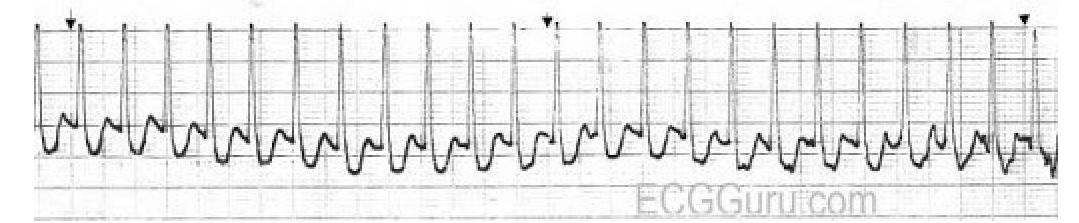
Identify the diagnosis based on the provided ECG image.
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
In patients with Retinitis pigmentosa, which of the following substances is known to have decreased levels?
In the context of gunshot injuries, which of the following describes the characteristics of a close shot entry wound, including signs such as burning, blackening, tattooing around the wound, and the presence of a dirt collar?
Which murmur increases on standing?
Most characteristic cardiovascular defect seen in Rubella-
Identify the diagnosis based on the provided ECG image.

Female with 41 wk gestation confirmed by radiological investigation, very sure of her LMP, no uterine contractions, no effacement and no dilatation. What should be done to induce labor?
Which of the following statements about conjunctival lesions is NOT true?
What is the recommended dose of diphtheria antitoxin for adults?
Achondroplasia shows which type of inheritance?
Identify the surgical instrument based on its characteristics: a small, triangular blade used for precise incisions.