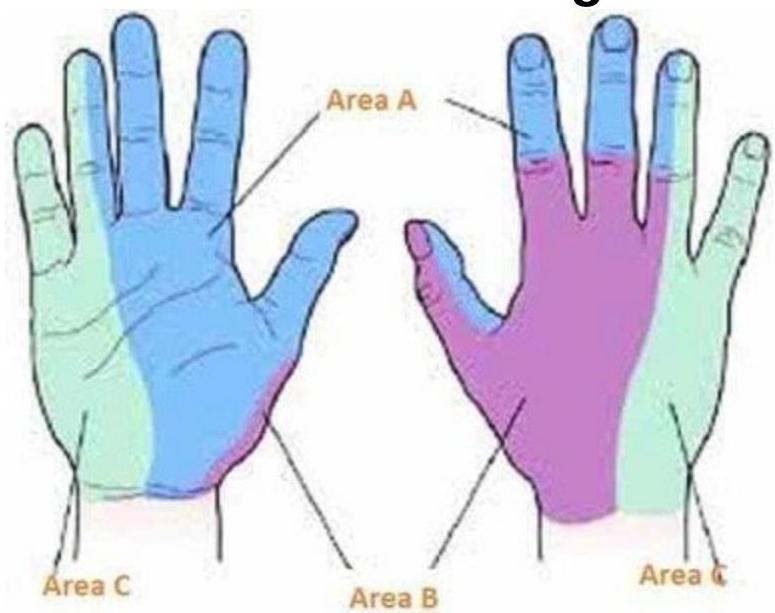
Which nerve supplies the area marked as ‘Area B’ in the image?
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
Which nerve supplies the area marked as ‘Area B’ in the image?

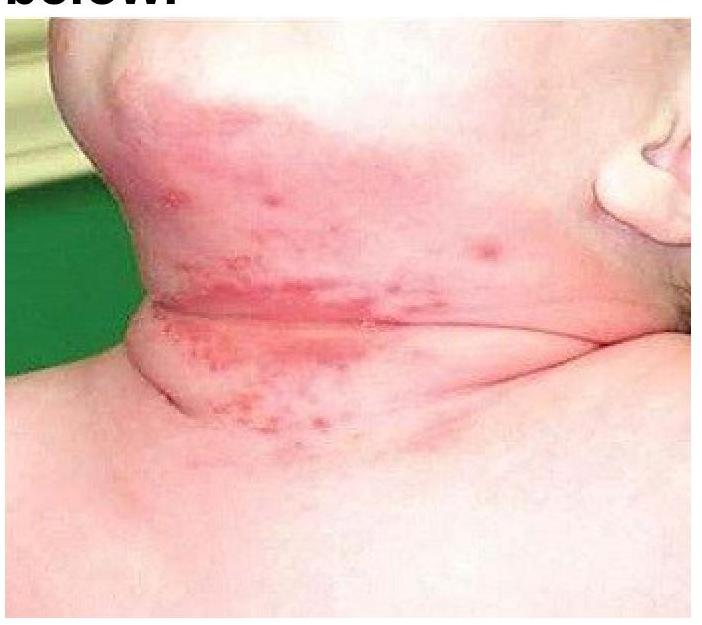
A child presents with a rash in the neck folds as shown in the image. The area appears erythematous with satellite lesions and maceration. What is the most likely diagnosis?
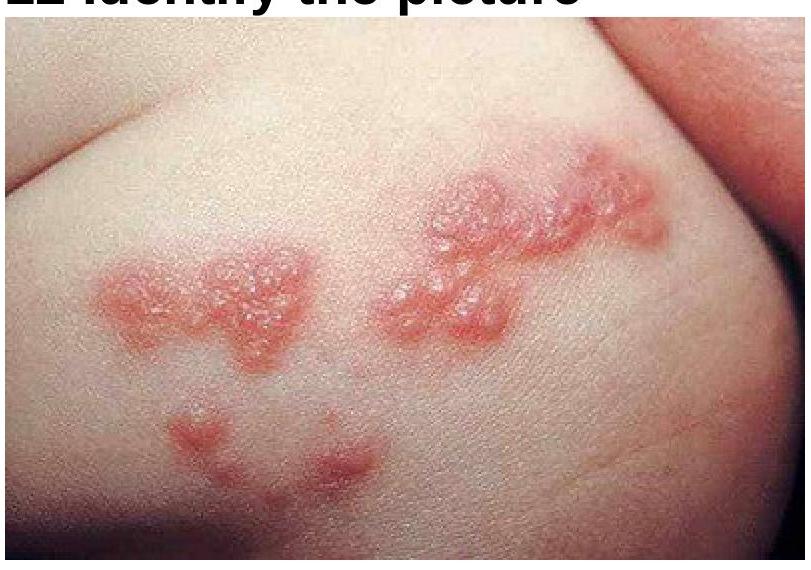
A patient presents with painful vesicular eruptions on one side of the body. What is the most likely diagnosis based on the clinical image?
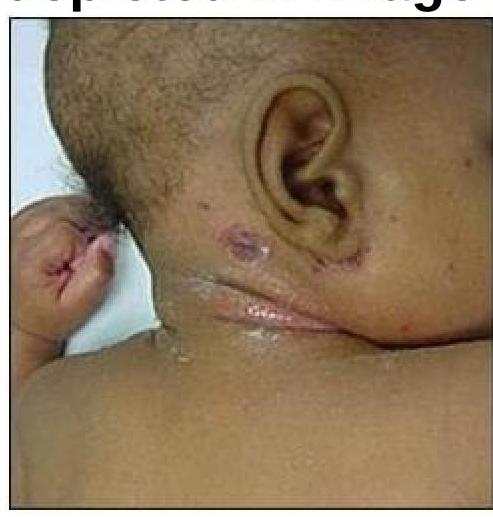
What is the causative organism for the condition depicted in the image?
Which of the following treatments is used for vulvar atrophy and itching?
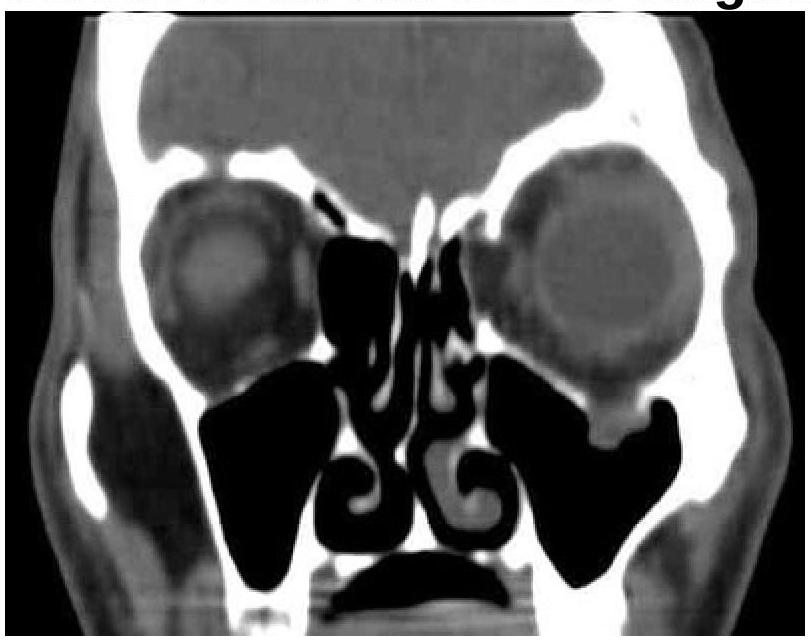
A patient presented with a history of diplopia and restricted eye movements. What is the most likely diagnosis based on the clinical and CT images?
A baby born at 34 weeks gestation weighs 3kg. Which of the following conditions is this child most likely to develop in the immediate postnatal period?
Type of sensation lost on same side of Brown Sequard syndrome?
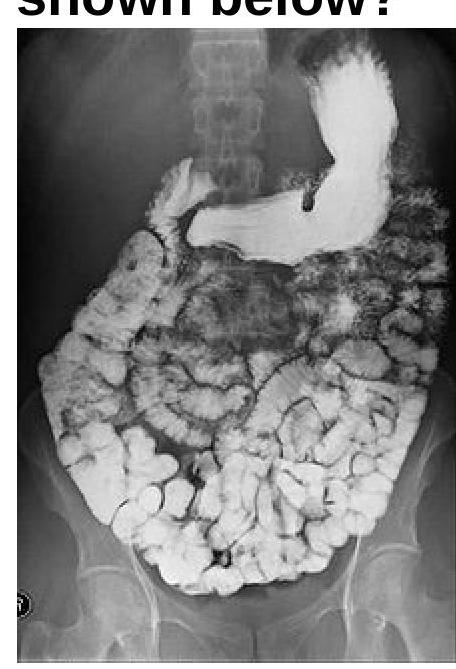
Identify the radiological procedure shown in the image?
The most common site of the branchial cyst is: