NEET-PG 2019 — Microbiology
19 Previous Year Questions with Answers & Explanations
What is the gold standard microbiological test for diagnosing Leptospira infection?
Rubella virus belongs to which family?
Which culture media is specifically used for the growth of Legionella?
A 36-year-old male patient complaining of cough, cold, fever, and rusty sputum, with a history of travel to China and consumption of crab. Name the infection.
What is the causative organism for the condition depicted in the image?
A 6-year-old boy presents with fever and chills, cough, rapid breathing, difficulty breathing, and chest pain. A culture from a respiratory sample shows Gram-positive bacteria. What is the most likely organism causing this infection?
What is the primary method for diagnosing Pneumocystis jirovecii pneumonia?
MHC II is associated with:-
Caspase involved in activation of IL-1 is which of the following?
A 9 years old child presented to OPD with complaints of high grade fever, vomiting, one episode of seizure. CSF examination was done and Gram staining of the culture showed the following finding. What is the probable causative agent?
NEET-PG 2019 - Microbiology NEET-PG Practice Questions and MCQs
Question 1: What is the gold standard microbiological test for diagnosing Leptospira infection?
- A. Cold agglutination
- B. Standard agglutination
- C. Microscopic agglutination test (MAT) (Correct Answer)
- D. ELISA test
Explanation: ***Microscopic agglutination test (MAT)*** - The **Microscopic Agglutination Test (MAT)** is considered the **gold standard** for diagnosing leptospirosis due to its high sensitivity and specificity. - It detects **agglutinating antibodies** against live leptospiral serovars, allowing for both diagnosis and serovar identification. *Cold agglutination* - **Cold agglutinins** are antibodies that react with red blood cells at cold temperatures and are typically associated with **Mycoplasma pneumoniae** infections or certain autoimmune conditions. - This test is **not used** for the diagnosis of leptospirosis. *Standard agglutination* - **Standard agglutination tests** involve macroscopic observation of agglutination and are generally less sensitive and specific than microscopic methods. - While agglutination is the principle, the **MAT** specifically refers to the microscopic, highly sensitive method used for Leptospira. *ELISA test* - **ELISA (Enzyme-Linked Immunosorbent Assay)** is used for leptospirosis, primarily for screening and detecting **IgM antibodies** in acute infections. - However, it has **lower specificity** and sensitivity compared to MAT, particularly in early stages or for serovar differentiation.
Question 2: Rubella virus belongs to which family?
- A. Orthomyxovirus
- B. Rheovirus
- C. Togavirus (Correct Answer)
- D. Picornavirus
Explanation: ***Togavirus*** - The **Rubella virus** is categorized under the family **Togaviridae**, specifically within the genus *Rubivirus*. - This classification is based on its genetic structure, being an **enveloped, positive-sense, single-stranded RNA virus**. *Rheovirus* - **Reoviruses** are characterized by a **double-stranded segmented RNA genome** and are typically non-enveloped. - This contrasts with Rubella's single-stranded, non-segmented RNA and enveloped structure. *Picornavirus* - **Picornaviruses** are a family of **non-enveloped, positive-sense, single-stranded RNA viruses** that are structurally different from Rubella. - Examples include species like **poliovirus** and **rhinovirus**, which do not share the distinct biological properties of Rubella. *Orthomyxovirus* - **Orthomyxoviruses** are a family of **enveloped, negative-sense, segmented RNA viruses**, which includes influenza viruses. - Their genomic organization and replication strategy are fundamentally different from those of the Rubella virus.
Question 3: Which culture media is specifically used for the growth of Legionella?
- A. Buffered Charcoal Yeast Extract (BCYE) agar (Correct Answer)
- B. MacConkey agar
- C. Baird–Parker agar
- D. Sabouraud’s agar
Explanation: ***(BCYE) agar media*** - **Buffered charcoal yeast extract (BCYE) agar** is the specific and most widely used culture medium for the isolation and growth of *Legionella* species. - It contains **L-cysteine** and **iron salts**, which are essential growth factors for *Legionella*, along with activated charcoal to neutralize toxic metabolites. *MacConkey agar* - **MacConkey agar** is a selective and differential medium primarily used for the isolation of **Gram-negative enteric bacilli**. - It inhibits the growth of Gram-positive bacteria and differentiates lactose fermenters from non-fermenters. *Baird–Parker agar* - **Baird–Parker agar** is a selective medium specifically designed for the isolation and enumeration of **coagulase-positive staphylococci**, particularly *Staphylococcus aureus*, from food and clinical samples. - It contains tellurite, which is reduced by staphylococci to form black colonies. *Sabouraud’s agar* - **Sabouraud's dextrose agar (SDA)** is a selective medium primarily used for the cultivation of **fungi** (yeasts and molds). - Its low pH and high dextrose concentration inhibit the growth of most bacteria.
Question 4: A 36-year-old male patient complaining of cough, cold, fever, and rusty sputum, with a history of travel to China and consumption of crab. Name the infection.
- A. Paragonimus westermani (Correct Answer)
- B. Fasciola hepatica
- C. Fasciolopsis buski
- D. Entamoeba histolytica
Explanation: ***Paragonimus westermani*** - This patient's symptoms of **cough**, **fever**, and **rusty sputum**, combined with a history of **travel to China** and consumption of **crab**, are highly suggestive of **paragonimiasis**. - *Paragonimus westermani* is a **lung fluke** endemic to East Asia, and its larvae are acquired by ingesting undercooked **crabs** or **crayfish**. *Fasciola hepatica* - *Fasciola hepatica* causes **fascioliasis**, primarily affecting the **liver** and **biliary ducts**, leading to symptoms like **fever**, **abdominal pain**, and **hepatomegaly**. - It is acquired by consuming **contaminated watercress** or other aquatic plants, not crabs. *Fasciolopsis buski* - *Fasciolopsis buski* causes **fasciolopsiasis**, an **intestinal fluke infection** presenting with **abdominal pain**, **diarrhea**, and **malabsorption**. - It is transmitted through ingestion of **contaminated aquatic plants**, and does not typically cause respiratory symptoms or "rusty sputum." *Entamoeba histolytica* - *Entamoeba histolytica* is a **protozoan** that causes **amoebiasis**, primarily presenting as **dysentery** or **amoebic liver abscess**. - While it can manifest as fever and liver involvement, it does not cause respiratory symptoms like "rusty sputum" and is not acquired from crabs.
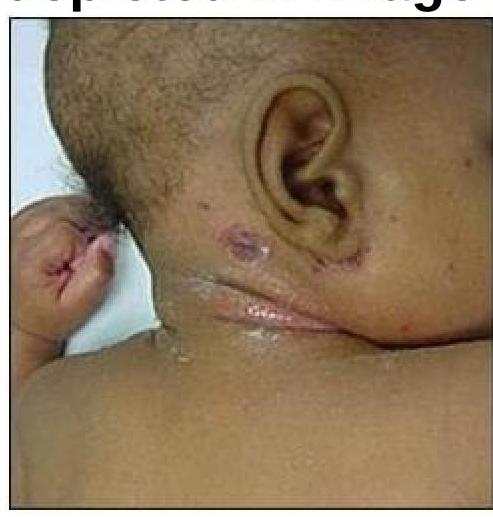
Question 5: What is the causative organism for the condition depicted in the image?
- A. Staphylococci (Correct Answer)
- B. Candidal infection
- C. Streptococcus
- D. Actinomycetes
Explanation: ***Staphylococci*** - The image shows **impetigo** with **crusted lesions**, consistent with **_Staphylococcus aureus_** infection. - **Staphylococcus aureus** is a major causative organism of impetigo, particularly **bullous impetigo**, and commonly produces the characteristic **honey-colored crusts** seen in non-bullous forms as well. - This superficial bacterial skin infection is highly contagious and responds well to topical or systemic antibiotics. *Candidal infection* - **Candidal infections** (e.g., candidiasis) typically present as **erythematous patches** with satellite lesions, or white plaques in mucosal areas, which is not consistent with the image. - This fungal infection is often seen in immunocompromised individuals or in warm, moist skin folds, not as crusted superficial lesions. *Streptococcus* - While **_Streptococcus pyogenes_** can also cause impetigo (especially non-bullous impetigo), the clinical presentation in the image is most consistent with **staphylococcal infection**. - Streptococcal infections may present similarly but can also cause other conditions like cellulitis or erysipelas with distinct features. *Actinomycetes* - **Actinomycosis** is a rare, chronic bacterial infection that forms **abscesses and sinus tracts**, often with "sulfur granules," which is distinct from the superficial skin lesions shown. - This infection usually involves deeper tissues and presents as a chronic, indolent infection, unlike the acute superficial presentation of impetigo.
Question 6: A 6-year-old boy presents with fever and chills, cough, rapid breathing, difficulty breathing, and chest pain. A culture from a respiratory sample shows Gram-positive bacteria. What is the most likely organism causing this infection?
- A. Streptococcus pyogenes
- B. Streptococcus pneumoniae (Correct Answer)
- C. Staphylococcus aureus
- D. Propionibacterium acnes
Explanation: ***Streptococcus pneumoniae*** - This clinical picture describes typical symptoms of **pneumonia** in a child, including fever, cough, rapid and difficult breathing, and chest pain. - **_Streptococcus pneumoniae_** is the most common bacterial cause of community-acquired pneumonia in children. The respiratory sample showing gram-positive bacteria further supports this. *Staphylococcus aureus* - While **_Staphylococcus aureus_** can cause pneumonia, it is less common than _Streptococcus pneumoniae_ in community-acquired cases in healthy children and often associated with more severe, necrotizing forms or post-viral infections. - While it is a **Gram-positive bacterium**, its clinical presentation would not be the most likely first choice for typical pneumonia symptoms in this age group. *Propionibacterium acnes* - **_Propionibacterium acnes_** (now *Cutibacterium acnes*) is primarily associated with **acne vulgaris** and, less commonly, opportunistic infections related to implanted devices or some rare soft tissue infections. - It is not a typical cause of primary respiratory infections like pneumonia. *Streptococcus pyogenes* - **_Streptococcus pyogenes_** (Group A Streptococcus) is known for causing **pharyngitis** (strep throat), skin infections (impetigo, cellulitis), and scarlet fever. - While it can rarely cause pneumonia, it is not a common cause, and the constellation of symptoms points more strongly to _Streptococcus pneumoniae_.
Question 7: What is the primary method for diagnosing Pneumocystis jirovecii pneumonia?
- A. Sputum microscopy
- B. Chest X-ray findings
- C. Bronchoalveolar lavage (BAL) (Correct Answer)
- D. Serum beta-D-glucan assay
Explanation: ***Bronchoalveolar lavage (BAL)*** - **BAL** is the **gold standard** and **primary definitive method** for diagnosing *Pneumocystis jirovecii* pneumonia (PJP), with **sensitivity of 90-99%** and high specificity. - It involves bronchoscopy with lavage of the affected lung segments, allowing direct visualization and sampling of organisms using stains like **Gomori methenamine silver (GMS)**, **Giemsa**, or **immunofluorescence**. - BAL is particularly important in **immunocompromised patients** (HIV/AIDS, transplant recipients, chemotherapy patients) where definitive diagnosis is crucial for treatment decisions. - Though invasive, it remains the **most reliable diagnostic method** when PJP is suspected, especially when non-invasive methods are negative or inconclusive. *Sputum microscopy* - **Induced sputum microscopy** is a useful **initial non-invasive screening method**, but has **limited sensitivity (50-60%)** compared to BAL. - Many PJP patients cannot produce adequate sputum samples, and negative results do not exclude the diagnosis. - When positive, it can guide early treatment, but **negative sputum requires proceeding to BAL** for definitive diagnosis in high-suspicion cases. *Serum beta-D-glucan assay* - The **serum beta-D-glucan assay** is a **highly sensitive supportive marker** for PJP (sensitivity 90-95%), detecting fungal cell wall components. - However, it is an **indirect test** that cannot differentiate PJP from other fungal infections (*Candida*, *Aspergillus*). - Used as an **adjunctive diagnostic tool** rather than a primary definitive method, particularly helpful in risk stratification. *Chest X-ray findings* - **Chest X-ray** typically shows **bilateral interstitial infiltrates** in a "ground-glass" pattern, but findings are **non-specific** and can be normal in early disease. - Radiographic findings support clinical suspicion but **cannot provide definitive diagnosis** without microbiological confirmation. - Useful for initial assessment and monitoring treatment response, not for primary diagnosis.
Question 8: MHC II is associated with:-
- A. Red blood cells
- B. Antigen presenting cells (Correct Answer)
- C. Platelets
- D. Epithelial cells
Explanation: ***Antigen presenting cells*** - **MHC II (Major Histocompatibility Complex class II)** molecules are primarily expressed on the surface of professional **antigen-presenting cells (APCs)**. - APCs, such as **macrophages**, **dendritic cells**, and **B lymphocytes**, use MHC II to present **extracellularly derived antigens** to **CD4+ T helper cells**. *Red blood cells* - **Red blood cells (RBCs)** are anucleated and lack MHC molecules entirely. - Their primary function is **oxygen transport**, not immune cell communication. *Platelets* - **Platelets** are cell fragments involved in **hemostasis** (blood clotting). - They do not express MHC class II molecules as they are not involved in antigen presentation. *Epithelial cells* - Most **epithelial cells** primarily express **MHC class I** molecules to present **intracellular antigens** to **CD8+ cytotoxic T cells**. - They do not typically express MHC class II unless under specific inflammatory conditions, and even then, not as their primary function.
Question 9: Caspase involved in activation of IL-1 is which of the following?
- A. Caspase 5
- B. Caspase 1 (Correct Answer)
- C. Caspase 8
- D. Caspase 3
Explanation: ***Caspase 1*** - **Caspase 1** (also known as interleukin-1 beta converting enzyme or ICE) is the primary caspase responsible for the proteolytic cleavage and activation of pro-IL-1β and pro-IL-18 into their mature, active forms. - This activation occurs within the **inflammasome complex**, a multiprotein oligomer that assembles in response to various pathogens and danger signals. *Caspase 5* - While **Caspase 5** is an inflammatory caspase, similar to Caspase 1, it primarily functions in the direct activation of pro-IL-1β in certain contexts, particularly in response to *Gram-negative bacteria* through the non-canonical inflammasome. - However, **Caspase 1** is the canonical and most well-known activator of IL-1 in the classical inflammasome pathway. *Caspase 8* - **Caspase 8** is a key **initiator caspase** in the extrinsic pathway of apoptosis, activated by death receptors like Fas and TNF receptors. - Its primary role is in **apoptotic signaling** and it is not directly involved in the proteolytic activation of IL-1. *Caspase 3* - **Caspase 3** is a major **effector caspase** in both the intrinsic and extrinsic pathways of apoptosis. - It executes apoptosis by cleaving numerous cellular substrates and is not directly involved in the **processing of cytokines** like IL-1.
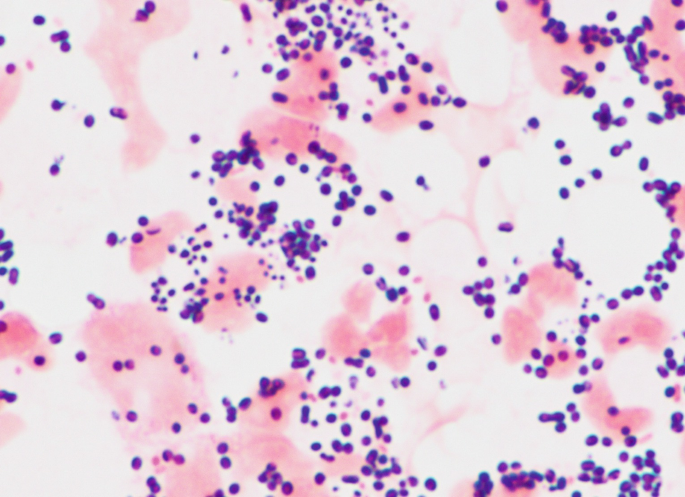
Question 10: A 9 years old child presented to OPD with complaints of high grade fever, vomiting, one episode of seizure. CSF examination was done and Gram staining of the culture showed the following finding. What is the probable causative agent?
- A. Gram-negative coccobacilli (e.g., Haemophilus influenzae)
- B. Gram-negative diplococci (e.g., Neisseria meningitidis)
- C. Gram-positive diplococci (e.g., Streptococcus pneumoniae) (Correct Answer)
- D. Gram-positive cocci in chains (e.g., Streptococcus pyogenes)
Explanation: ***Gram-positive diplococci (e.g., Streptococcus pneumoniae)*** - The image displays small, purple (Gram-positive) cocci arranged in pairs (**diplococci**). - *Streptococcus pneumoniae* is a common cause of **bacterial meningitis** in children, and its characteristic morphology on Gram stain is Gram-positive diplococci. *Gram-negative coccobacilli (e.g., Haemophilus influenzae)* - While *Haemophilus influenzae* can cause meningitis in children, its Gram stain morphology would show **pink-stained coccobacillary forms**, not purple cocci. - The bacteria in the image are clearly cocci, not coccobacilli, and stain Gram-positive (purple). *Gram-negative diplococci (e.g., Neisseria meningitidis)* - *Neisseria meningitidis* is a significant cause of meningitis and appears as **Gram-negative (pink) diplococci**. - The organisms in the image are stained purple, indicating they are Gram-positive. *Gram-positive cocci in chains (e.g., Streptococcus pyogenes)* - *Streptococcus pyogenes* typically forms **chains of Gram-positive cocci**, which is not the predominant arrangement seen in the image. - Although it is Gram-positive, the characteristic arrangement in the image is diplococci, not chains.