A man who is chronic alcoholic will develop which type of cardiomyopathy?
In type I diabetes, which of the following is the MOST characteristic metabolic change that distinguishes it from type II diabetes:-
Which of the following is autosomal dominant in inheritance?
HIV patient presented with diarrhea. On stool examination, acid-fast organisms (Isospora belli) were seen. What is the drug of choice in this patient?
Which apolipoprotein is most strongly associated with increased risk of Alzheimer's disease?
Which chamber of the heart is enlarged first in a patient with mitral stenosis?
A 26 year old female patient presented with fever, oral ulcers, sensitivity to light and rash over the malar area of the face sparing the nasolabial folds of both side. Which of the following indicates the condition associated with these manifestations?
A 20-year-old alcoholic malnourished patient presented to the hospital with respiratory distress. His pulse was 112/minute. The patient had edema, hypertension, a systolic murmur along the left sternal edge, and bilateral crepitations in the lungs. A diagnosis of congestive high-output cardiac failure was made. Which vitamin is deficient?
A 55-year-old female on methotrexate presents with continuous pain and swelling of bilateral hand joints. What is the best treatment plan for this patient?
NEET-PG 2019 - Internal Medicine NEET-PG Practice Questions and MCQs
Question 31: A man who is chronic alcoholic will develop which type of cardiomyopathy?
- A. Dilated cardiomyopathy (Correct Answer)
- B. Hypertrophic cardiomyopathy
- C. Myocarditis
- D. Pericarditis
Explanation: ***Dilated cardiomyopathy*** - Chronic alcohol abuse is a major cause of **dilated cardiomyopathy**, where the heart's pumping chambers (ventricles) become enlarged and weakened, leading to reduced cardiac output [1]. - This condition often called **alcoholic cardiomyopathy**, is characterized by **ventricular dilation** and **systolic dysfunction**. *Hypertrophic cardiomyopathy* - This condition involves thickening of the heart muscle, often genetic, and is not directly caused by **chronic alcoholism**. - While alcohol can worsen pre-existing heart conditions, it does not typically lead to primary **hypertrophic cardiomyopathy**. *Myocarditis* - **Myocarditis** is an inflammation of the heart muscle, usually caused by viral infections or autoimmune processes. - Although heavy alcohol use can weaken the immune system, it is not a direct cause of viral or primary inflammatory myocarditis. *Pericarditis* - **Pericarditis** is the inflammation of the pericardium, the sac surrounding the heart, most commonly due to viral infections or autoimmune conditions. - While alcohol abuse can have various systemic effects, it is not a recognized direct cause of **pericarditis**.
Question 32: In type I diabetes, which of the following is the MOST characteristic metabolic change that distinguishes it from type II diabetes:-
- A. Increased protein catabolism
- B. Decreased glucose uptake
- C. Increased hepatic glucose output
- D. Increased lipolysis (Correct Answer)
Explanation: ***Increased lipolysis*** - In **type 1 diabetes** (T1D), there is an **absolute deficiency of insulin**, which is a potent **anti-lipolytic hormone**. [1] - This lack of insulin leads to unopposed **lipolysis**, resulting in increased free fatty acid (FFA) release, which can be metabolized into **ketone bodies** and contribute to **diabetic ketoacidosis (DKA)**. [2] *Increased protein catabolism* - While protein catabolism is increased in uncontrolled T1D due to the lack of insulin and increased counter-regulatory hormones, it is not the *most characteristic* metabolic change that clearly distinguishes it from type 2 diabetes (T2D), especially in early stages of T2D where some insulin may still be present. [1] - **Protein breakdown** produces amino acids for gluconeogenesis, contributing to hyperglycemia, but **lipolysis leading to ketosis** is more specific to severe insulin deficiency. [3] *Decreased glucose uptake* - **Decreased glucose uptake** by peripheral tissues (especially muscle and adipose tissue) is a characteristic feature of both T1D and T2D. [1] - In T1D, it's due to insulin deficiency, while in T2D, it's primarily caused by **insulin resistance**, making it less specific to distinguish T1D. *Increased hepatic glucose output* - **Increased hepatic glucose output** is a significant contributor to hyperglycemia in both T1D and T2D. [1] - In T1D, it's due to the lack of insulin's suppressive effect on the liver, whereas in T2D, it's due to **hepatic insulin resistance** and increased gluconeogenesis.
Question 33: Which of the following is autosomal dominant in inheritance?
- A. Achondroplasia (Correct Answer)
- B. Hemochromatosis
- C. Sickle cell disease
- D. Wiskott Aldrich syndrome
Explanation: ***Achondroplasia*** - This condition is inherited in an **autosomal dominant** pattern, meaning only one copy of the mutated gene is needed to cause the disorder. - It is caused by a mutation in the **FGFR3 gene**, leading to abnormal bone growth and short-limbed dwarfism [1]. *Hemochromatosis* - This condition is primarily inherited in an **autosomal recessive** pattern, meaning two copies of the mutated gene (HFE gene) are required for the disease to manifest. - It leads to excessive iron absorption and organ damage. *Sickle cell disease* - This is an **autosomal recessive** disordertoo. - It results from a mutation in the **HBB gene**, affecting hemoglobin and causing red blood cells to become sickle-shaped. *Wiskott Aldrich syndrome* - This is an **X-linked recessive** disorder, meaning it primarily affects males. - It involves mutations in the **WAS gene**, leading to immunodeficiency, eczema, and thrombocytopenia.
Question 34: HIV patient presented with diarrhea. On stool examination, acid-fast organisms (Isospora belli) were seen. What is the drug of choice in this patient?
- A. Niclosamide
- B. Nitazoxanide
- C. Primaquine
- D. TMP-SMX (Correct Answer)
Explanation: ***TMP-SMX*** - **Trimethoprim-sulfamethoxazole (TMP-SMX)** is the primary treatment for **Isospora belli** infections, especially in HIV-positive patients [1]. - It is highly effective in eradicating the parasite and preventing relapses in immunocompromised individuals [1]. *Niclosamide* - **Niclosamide** is an antihelminthic drug primarily used for treating **tapeworm infections** [2]. - It is not effective against protozoal parasites like *Isospora belli*. *Nitazoxanide* - **Nitazoxanide** is an antiparasitic drug that can be used for various protozoal and helminthic infections, including *Cryptosporidium* and *Giardia*. - While it has some efficacy against *Isospora belli*, it is generally considered a second-line agent, with **TMP-SMX** being the drug of choice [1]. *Primaquine* - **Primaquine** is an antimalarial drug specifically used to prevent relapse of **Plasmodium vivax** and **Plasmodium ovale** malaria by targeting hypnozoites. - It has no role in the treatment of **Isospora belli** infection.
Question 35: Which apolipoprotein is most strongly associated with increased risk of Alzheimer's disease?
- A. APOE3
- B. APOE4 (Correct Answer)
- C. APOC3
- D. APOE2
Explanation: APOE4 - The APOE4 allele is the strongest genetic risk factor for late-onset Alzheimer's disease, increasing risk and lowering the age of onset in a gene-dose dependent manner. - Individuals with one copy of APOE4 have a 2-3 times increased risk, and those with two copies have an 8-12 times increased risk compared to those with APOE3. APOE3 - APOE3 is the most common allele and is considered a neutral risk factor for Alzheimer's disease. - It plays a normal role in lipid metabolism and brain function without significantly increasing or decreasing AD risk. APOC3 - APOC3 is involved in triglyceride metabolism and is primarily linked to cardiovascular disease risk, not Alzheimer's disease. - While it modulates lipid levels, it does not have a direct, strong genetic association with AD pathogenesis. APOE2 - APOE2 is associated with a reduced risk of Alzheimer's disease, offering a protective effect against its development. - It is thought to improve the clearance of amyloid-beta (A̠) plaques, a hallmark of AD pathology.
Question 36: Which chamber of the heart is enlarged first in a patient with mitral stenosis?
- A. Left ventricle
- B. Right ventricle
- C. Right atrium
- D. Left atrium (Correct Answer)
Explanation: ***Left atrium*** - **Mitral stenosis** obstructs blood flow from the left atrium to the left ventricle, leading to a build-up of pressure in the left atrium [1]. - This chronic pressure overload causes the **left atrium to dilate and hypertrophy** in an attempt to pump blood through the narrowed valve [1]. *Left ventricle* - In **mitral stenosis**, the left ventricle typically receives a reduced volume of blood, leading to a **smaller, underfilled left ventricle**, rather than enlargement. - Its workload is decreased due to reduced preload, so it does not hypertrophy or dilate primarily. *Right ventricle* - **Right ventricular enlargement** can eventually occur in severe and chronic mitral stenosis due to **pulmonary hypertension** caused by back pressure from the left atrium, but it is not the *first* chamber to be affected [1], [2]. - Increased pressure in the pulmonary circulation increases the workload on the right ventricle, leading to hypertrophy and dilation over time [1], [2]. *Right atrium* - **Right atrial enlargement** is a consequence of chronic and severe pulmonary hypertension affecting the right ventricle, which then causes back pressure into the right atrium [1]. - This is a very late manifestation of mitral stenosis, occurring after significant involvement of the left atrium and pulmonary vasculature.
Question 37: A 26 year old female patient presented with fever, oral ulcers, sensitivity to light and rash over the malar area of the face sparing the nasolabial folds of both side. Which of the following indicates the condition associated with these manifestations?
- A. Rosacea
- B. Dermatomyositis
- C. Psoriasis
- D. SLE (Correct Answer)
Explanation: ***SLE*** - The combination of **fever**, **oral ulcers**, **photosensitivity**, and a **malar rash** (which typically spares the nasolabial folds), particularly in a young female, is classic for **Systemic Lupus Erythematosus (SLE)** [1]. - SLE is a **chronic autoimmune inflammatory disease** that can affect multiple organ systems [2]. *Rosacea* - Rosacea often presents with **facial erythema**, **telangiectasias**, and papulopustules, primarily on the central face, but it does not typically involve oral ulcers, fever, or photosensitivity in the same way as SLE [4]. - The rash of rosacea is usually not a classic malar rash sparing the nasolabial folds, and it is not an autoimmune systemic disease. *Dermatomyositis* - Dermatomyositis is characterized by **proximal muscle weakness** and specific skin manifestations like **Gottron's papules** (over joints), **heliotrope rash** (periorbital edema), and a **shawl sign**, which differ from the presented symptoms [3]. - While it can cause light sensitivity and a rash, the distribution and associated symptoms (like no mention of muscle weakness) are not typical for a primary presentation of dermatomyositis. *Psoriasis* - Psoriasis typically presents with **well-demarcated erythematous plaques** covered with **silvery scales**, commonly on extensor surfaces like elbows and knees, and can also affect nails and joints. - It does not typically cause fever, oral ulcers, or a malar rash with nasolabial fold sparing, which are hallmarks of SLE.
Question 38: A 20-year-old alcoholic malnourished patient presented to the hospital with respiratory distress. His pulse was 112/minute. The patient had edema, hypertension, a systolic murmur along the left sternal edge, and bilateral crepitations in the lungs. A diagnosis of congestive high-output cardiac failure was made. Which vitamin is deficient?
- A. Vitamin B 6
- B. Vitamin B1 (Correct Answer)
- C. Vitamin B2
- D. Vitamin C
Explanation: ***Vitamin B1*** - The constellation of **high-output cardiac failure** (tachycardia, edema, hypertension, systolic murmur, pulmonary crepitations) in an alcoholic and malnourished patient strongly indicates **wet beriberi**, which is caused by **thiamine (Vitamin B1) deficiency** [1]. - **Alcoholism** is a major risk factor for thiamine deficiency due to poor nutritional intake and impaired absorption/meta [2]. *Vitamin B 6* - Deficiency of **pyridoxine (Vitamin B6)** can cause **sideroblastic anemia**, neurological symptoms like neuropathy and seizures, and **dermatitis**, but typically not high-output cardiac failure. - While alcoholics can be deficient in B6, it doesn't directly cause a primary cardiac syndrome like beriberi. *Vitamin B2* - **Riboflavin (Vitamin B2)** deficiency leads to symptoms such as **cheilosis**, **angular stomatitis**, **glossitis**, and **seborrheic dermatitis**, and sometimes corneal vascularization. - It is not directly associated with the described **congestive high-output cardiac failure** symptoms in this patient. *Vitamin C* - **Scurvy**, caused by **Vitamin C deficiency**, presents with **gingival bleeding**, **perifollicular hemorrhages**, **poor wound healing**, and **joint pain** [3]. - It does not cause high-output cardiac failure, although severe scurvy can lead to anemia and non-specific weakness.
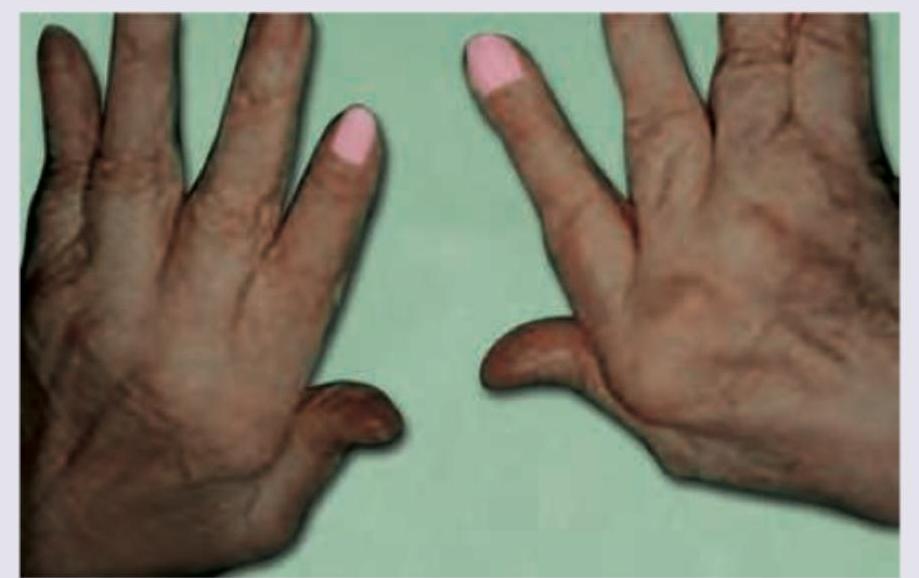
Question 39: A 55-year-old female on methotrexate presents with continuous pain and swelling of bilateral hand joints. What is the best treatment plan for this patient?
- A. Double the dose of methotrexate
- B. Methotrexate + high potency Oral steroids
- C. Methotrexate + Sulphasalazine + Hydroxychloroquine (Correct Answer)
- D. Stop methotrexate and start Monotherapy with anti-TNF- drugs
Explanation: ***Methotrexate + Sulphasalazine + Hydroxychloroquine*** - This combination, known as **triple therapy**, is a well-established and effective strategy for **rheumatoid arthritis** patients who have an inadequate response to methotrexate monotherapy. - The combination of **conventional synthetic DMARDs (csDMARDs)** targets different inflammatory pathways, leading to a synergistic effect and improved disease control. *Double the dose of methotrexate* - While methotrexate doses can be optimized, simply doubling the dose may not be the most effective next step for uncontrolled disease and could increase the risk of **toxicity** without significantly improving efficacy. - Current guidelines often advocate for adding another DMARD or switching to a biologic agent if maximum tolerated methotrexate is insufficient. *Methotrexate + high potency Oral steroids* - Oral steroids are primarily used for **short-term symptom control** during flares or as a bridge therapy, not as a long-term strategy for sustained disease modification due to their significant side effect profile. - Adding high-potency oral steroids long-term with methotrexate would increase the risk of adverse effects like osteoporosis, infections, and adrenal insufficiency. *Stop methotrexate and start Monotherapy with anti-TNF- drugs* - While **anti-TNF drugs** are a powerful next-line treatment, **monotherapy** is generally less effective than combination therapy, especially for patients with active disease. - **Methotrexate is often continued** in combination with anti-TNF drugs even when initiating biological therapies, as it can enhance their efficacy and reduce immunogenicity.