In which condition is a Cushing ulcer most likely to occur?
In which condition are solitary lytic lesions typically seen?
What are the essential major blood culture criteria for diagnosing infective endocarditis?
Most common type of gallstone is?
MRP2 associated with which of the following?
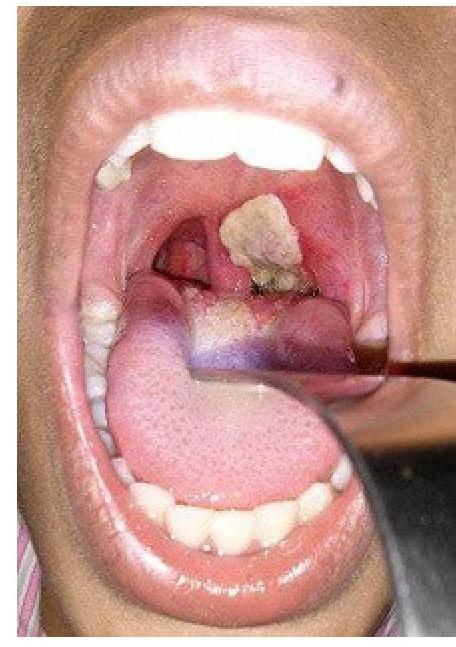
A patient presents with hoarseness of voice and a clinical condition as shown in the image. Identify the lesion:
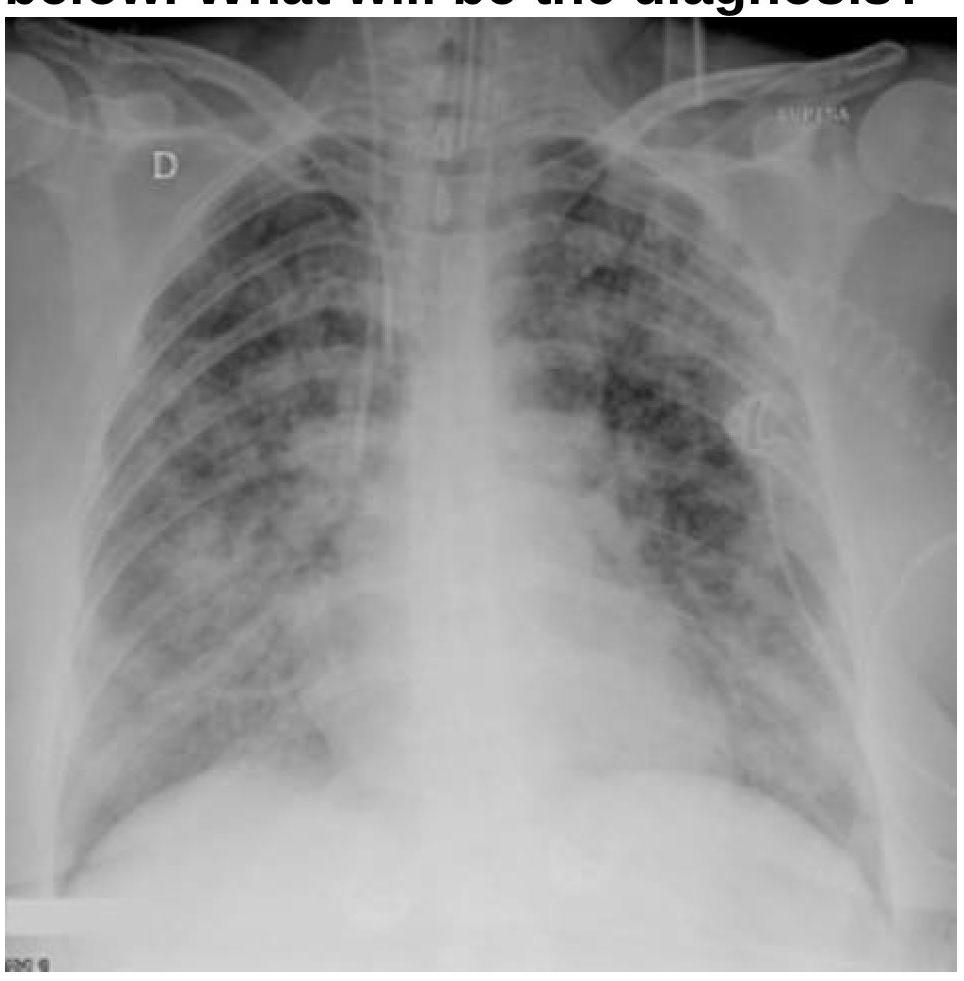
A patient with a known case of acute pancreatitis develops breathlessness and bilateral basal crepitations on day 4. What is the most likely diagnosis based on the chest radiography image?
True about decorticate rigidity:
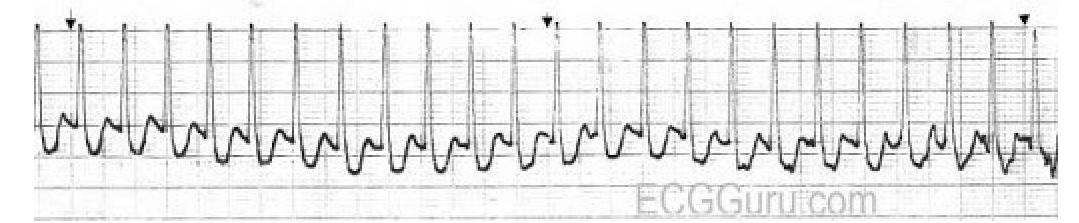
Identify the diagnosis based on the provided ECG image.
Most characteristic cardiovascular defect seen in Rubella-