NEET-PG 2019 — Internal Medicine
39 Previous Year Questions with Answers & Explanations
Calcitonin levels increased in
Which syndrome is associated with posterior inferior cerebellar artery thrombosis?
Which of the following exocrine glandular ducts are not obstructed in cystic fibrosis?
A 25-year-old alcoholic presented with edema, hypertension, ocular disturbance, and changes in mental state. A diagnosis of high output cardiac failure was made with Wet Beri Beri. This condition is due to a deficiency of which vitamin?
What does a decreased FEV1/FVC ratio typically indicate in pulmonary function tests?
Identify the cardiac condition represented in the image.
Which type of cardiomyopathy is associated with alcohol abuse?
Type of sensation lost on same side of Brown Sequard syndrome?
Which of the following statements about deep venous thrombosis (DVT) is incorrect?
A female patient of 26 years, presents with oral ulcers, photosensitivity and skin malar rash in face sparing the nasolabial folds of both side.
NEET-PG 2019 - Internal Medicine NEET-PG Practice Questions and MCQs
Question 1: Calcitonin levels increased in
- A. Hypoparathyroidism
- B. Cushing Syndrome
- C. Medullary thyroid carcinoma (Correct Answer)
- D. Hyperparathyroidism
Explanation: Medullary thyroid carcinoma - Calcitonin is a hormone produced by the parafollicular C cells of the thyroid gland. - Medullary thyroid carcinoma is a neuroendocrine tumor arising from these C cells, leading to excessive and unregulated calcitonin production. Hyperparathyroidism - This condition involves increased production of parathyroid hormone (PTH), which acts to increase serum calcium levels [2]. - Calcitonin secretion is typically decreased or normal in hyperparathyroidism, as calcitonin works to lower serum calcium. Hypoparathyroidism - This condition is characterized by insufficient production of parathyroid hormone (PTH), leading to low serum calcium levels [1]. - Calcitonin levels are generally unaffected or may even be slightly decreased in response to the low calcium, as its primary role is to lower calcium. Cushing Syndrome - Cushing Syndrome is caused by prolonged exposure to high levels of cortisol, a glucocorticoid. - While cortisol can affect bone metabolism, it does not directly impact calcitonin production or secretion, which is primarily regulated by serum calcium levels and C-cell activity.
Question 2: Which syndrome is associated with posterior inferior cerebellar artery thrombosis?
- A. Wallenberg syndrome (Correct Answer)
- B. Medial medullary syndrome
- C. Inferior alternating syndrome
- D. Dejerine syndrome
Explanation: No specific references from the provided list reached the relevance threshold (score >= 7) to be cited in the explanation. The original text remains unchanged. ***Wallenberg syndrome*** - Also known as **lateral medullary syndrome**, it is caused by **thrombosis of the posterior inferior cerebellar artery (PICA)** or its branches. - Symptoms include ipsilateral **ataxia**, **vertigo**, **nystagmus**, dysphagia, and contralateral loss of pain and temperature sensation. *Medial medullary syndrome* - This syndrome results from occlusion of the **anterior spinal artery** and paramedian branches of the **vertebral artery**. - Clinical features include contralateral **hemiparesis**, ipsilateral **tongue deviation**, and loss of position and vibration sensation. *Inferior alternating syndrome* - This is another name for **medial medullary syndrome**, caused by a lesion in the **medulla oblongata**. - It is characterized by ipsilateral cranial nerve signs and contralateral long tract signs, differentiating it from Wallenberg syndrome. *Dejerine syndrome* - Also known as **medial medullary syndrome**, it is linked to occlusion of the **anterior spinal artery**. - Symptoms primarily involve the **pyramidal tract**, **medial lemniscus**, and **hypoglossal nerve**.
Question 3: Which of the following exocrine glandular ducts are not obstructed in cystic fibrosis?
- A. Pancreas
- B. Lung
- C. Sweat gland (Correct Answer)
- D. None of the options
Explanation: ***Sweat gland*** - In cystic fibrosis, the **CFTR protein** in sweat glands is defective, leading to **impaired chloride reabsorption** and excessively salty sweat [1]. - This defect causes dysfunctional sweat production but **does not result in obstruction** of the sweat gland ducts, which continue to secrete. *Pancreas* - The **exocrine pancreatic ducts** are frequently obstructed in cystic fibrosis due to the production of **thick, sticky mucus**. - This obstruction leads to maldigestion and **pancreatic insufficiency**, requiring enzyme replacement therapy. *Lung* - **Bronchial ducts** and airways in the lungs are severely affected by the accumulation of **viscous mucus**, leading to chronic obstruction [1]. - This obstruction impairs mucociliary clearance, making patients susceptible to recurrent **pulmonary infections** and progressive lung damage [1], [2]. *None of the options* - This option is incorrect because sweat glands are indeed not obstructed, making option C the appropriate answer.
Question 4: A 25-year-old alcoholic presented with edema, hypertension, ocular disturbance, and changes in mental state. A diagnosis of high output cardiac failure was made with Wet Beri Beri. This condition is due to a deficiency of which vitamin?
- A. Vitamin B3
- B. Vitamin B6
- C. Vitamin B9
- D. Vitamin B1 (Correct Answer)
Explanation: Vitamin B1 - The constellation of **edema**, **hypertension**, **ocular disturbances**, and **mental status changes** in an **alcoholic** patient with **high-output cardiac failure** (Wet Beri Beri) is a classic presentation of **thiamine (Vitamin B1) deficiency** [2], [3]. - **Thiamine** is crucial for **carbohydrate metabolism** and **neurological function**, and a deficiency can lead to severe cardiovascular and neurological dysfunction, especially in chronic alcoholics due to poor absorption and increased metabolic demand [1], [3]. Vitamin B3 - Deficiency of Vitamin B3 (niacin) causes **pellagra**, characterized by the "4 D's": **dermatitis**, **diarrhea**, **dementia**, and death. - While it can cause psychiatric symptoms (dementia), it does not directly lead to the specific cardiovascular manifestations of high-output cardiac failure as seen in Wet Beri Beri. Vitamin B6 - Deficiency of Vitamin B6 (pyridoxine) can result in **peripheral neuropathy**, **anemia**, and **seizures**. - It is not directly linked to the cardiac and edematous symptoms characteristic of Wet Beri Beri. Vitamin B9 - Deficiency of Vitamin B9 (folate) primarily causes **megaloblastic anemia** and can lead to **neural tube defects** in developing fetuses. - While it can manifest with fatigue and weakness due to anemia, it does not typically present with the acute cardiovascular and neurological syndrome described.
Question 5: What does a decreased FEV1/FVC ratio typically indicate in pulmonary function tests?
- A. Normal pulmonary function
- B. Obstructive lung disease (Correct Answer)
- C. Restrictive lung disease
- D. Both obstructive and restrictive lung disease
Explanation: ***Obstructive lung disease*** - A decreased **FEV1/FVC ratio** indicates that the amount of air forcefully exhaled in one second (FEV1) is disproportionately low compared to the total forced vital capacity (FVC) [1]. This is a hallmark of **airflow limitation**, distinguishing obstructive lung diseases. - This pattern suggests a problem with **airway narrowing** or obstruction, making it difficult to exhale air quickly, which is characteristic of conditions like **COPD** (emphysema, chronic bronchitis) or **asthma** [1]. *Normal pulmonary function* - In normal pulmonary function, the **FEV1/FVC ratio** would be within the expected reference range, typically **above 70%** (or 0.7) for adults [1]. - A low ratio explicitly indicates a deviation from normal airflow dynamics, not a state of healthy lung function. *Restrictive lung disease* - **Restrictive lung diseases** are characterized by a **reduced total lung volume** (decreased FVC), but the FEV1/FVC ratio is typically **normal or even increased**. - This is because the airways are generally not obstructed; instead, the problem lies with the lungs' inability to expand fully, leading to a proportional reduction in FEV1 and FVC. *Both obstructive and restrictive lung disease* - While it is possible to have both conditions, a **decreased FEV1/FVC ratio** primarily points to an **obstructive pattern**. - A definitive diagnosis of both would require further interpretation of other PFT parameters such as **total lung capacity (TLC)**, which would be normal or increased in obstruction and reduced in restriction.
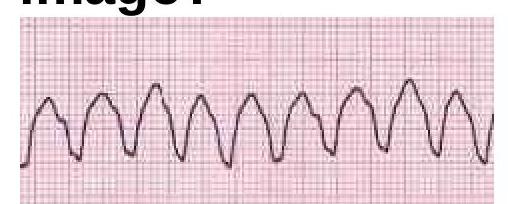
Question 6: Identify the cardiac condition represented in the image.
- A. Atrial fibrillation
- B. Atrial flutter
- C. Ventricular tachycardia (Correct Answer)
- D. Supraventricular tachycardia
Explanation: ***Ventricular tachycardia*** - The image displays a **wide, regular QRS complex tachycardia**, which is characteristic of **ventricular tachycardia (VT)**. - The QRS complexes are broad and bizarre, originating from an ectopic focus within the ventricles. *Atrial fibrillation* - **Atrial fibrillation** is characterized by an **irregularly irregular rhythm** with the absence of distinct P waves and varying R-R intervals. - The rhythm shown in the image is regular, which rules out atrial fibrillation. *Atrial flutter* - **Atrial flutter** typically presents with a "sawtooth" pattern of **flutter waves** in specific leads (e.g., II, III, aVF) and a regular or irregular ventricular response, often with a 2:1 or 3:1 block. - The image does not show these characteristic flutter waves. *Supraventricular tachycardia* - **Supraventricular tachycardia (SVT)** usually presents with a **narrow QRS complex** (unless there's an underlying bundle branch block) and a regular rhythm, originating from above the ventricles. - The QRS complexes in the image are wide, indicating a ventricular origin, not supraventricular.
Question 7: Which type of cardiomyopathy is associated with alcohol abuse?
- A. Hypertrophic cardiomyopathy
- B. Dilated cardiomyopathy (Correct Answer)
- C. Pericarditis
- D. Myocarditis
Explanation: ### Dilated cardiomyopathy - Chronic **alcohol abuse** is a well-established cause of **dilated cardiomyopathy**, leading to weakening and enlargement of the ventricles [1]. - This condition results in impaired systolic function and can cause **heart failure** [1]. *Hypertrophic cardiomyopathy* - This condition is primarily characterized by **pathological thickening of the heart muscle**, often genetic, and is not directly caused by alcohol abuse. - It leads to issues with relaxation and filling of the heart, rather than dilation and weakness. *Pericarditis* - **Pericarditis** is the inflammation of the sac surrounding the heart (pericardium), most commonly caused by viral infections, autoimmune diseases, or injury. - It is not directly linked to alcohol abuse as a primary cause. *Myocarditis* - **Myocarditis** is the inflammation of the heart muscle, often triggered by viral infections, autoimmune reactions, or certain medications. - While heavy alcohol use can weaken the heart, myocarditis is primarily an inflammatory process not directly caused by alcohol.
Question 8: Type of sensation lost on same side of Brown Sequard syndrome?
- A. Loss of pain sensation
- B. Loss of touch sensation
- C. Loss of proprioception (Correct Answer)
- D. Loss of temperature sensation
Explanation: ***Loss of proprioception*** - In **Brown-Séquard syndrome**, the lesion on one side of the spinal cord interrupts the **dorsal columns** on the same side, which carry **proprioception** and vibration sense [1]. - This results in the loss of **fine touch and proprioception** ipsilateral to the lesion [1]. *Loss of pain sensation* - **Pain and temperature sensations** are carried by the **spinothalamic tracts**, which cross in the spinal cord one or two levels above their entry [1]. - Therefore, a lesion in **Brown-Séquard syndrome** typically causes a loss of pain and temperature sensation **contralateral** to the lesion, starting a few segments below the injury [1]. *Loss of touch sensation* - **Crude touch** (non-discriminative touch) is carried by the spinothalamic tract, crossing to the contralateral side. - **Fine touch** (discriminative touch) is carried by the dorsal columns, which ascend ipsilaterally and cross in the medulla, leading to ipsilateral loss of fine touch in Brown-Séquard syndrome [1]. This option is too general, as fine touch is lost but crude touch involves a different pathway. *Loss of temperature sensation* - Similar to pain sensation, **temperature sensation** is carried by the **spinothalamic tracts** and crosses over in the spinal cord [1]. - This leads to a loss of temperature sensation **contralateral** to the lesion below the level of injury in **Brown-Séquard syndrome** [1].
Question 9: Which of the following statements about deep venous thrombosis (DVT) is incorrect?
- A. Mostly bilateral (Correct Answer)
- B. Most common clinically presents as pain and tenderness in calf
- C. Some cases may directly present as pulmonary thromboembolism
- D. Clinical assessment highly reliable
Explanation: ***Mostly bilateral*** - DVT is typically **unilateral**, affecting one limb [2]. Bilateral DVT is less common, making this statement incorrect [2]. - The symptoms of **pain, swelling, and tenderness** are usually localized to one leg [1]. *Most common clinically presents as pain and tenderness in calf* - **Calf pain and tenderness** are common clinical presentations of DVT, especially in the lower extremities [1]. - Other common signs include **swelling, warmth, and redness** in the affected leg [1]. *Some cases may directly present as pulmonary thromboembolism* - A significant concern with DVT is that a **clot can dislodge** and travel to the lungs, causing a **pulmonary embolism (PE)**, which can be the initial presentation [1]. - PE is a potentially life-threatening complication and may present with **dyspnea, chest pain, and hemoptysis**. *Clinical assessment highly reliable* - **Clinical assessment alone is not highly reliable** for diagnosing DVT due to its variable and often non-specific presentation [2]. - A definitive diagnosis usually requires objective diagnostic tests such as **compression ultrasonography** or **D-dimer assay** [3].
Question 10: A female patient of 26 years, presents with oral ulcers, photosensitivity and skin malar rash in face sparing the nasolabial folds of both side.
- A. Sturge weber syndrome
- B. Dermatitis
- C. Psoriasis
- D. SLE (Correct Answer)
Explanation: ***SLE*** - The combination of **oral ulcers**, **photosensitivity**, and a **malar rash** that spares the nasolabial folds is highly characteristic of **Systemic Lupus Erythematosus (SLE)** [1]. - SLE is an autoimmune disease with diverse clinical manifestations involving multiple organ systems. *Sturge weber syndrome* - This is a neurocutaneous disorder characterized by a **port-wine stain** (nevus flammeus) typically on the face, neurological abnormalities like seizures, and ocular involvement. - It does not present with oral ulcers or photosensitivity as primary features. *Dermatitis* - **Dermatitis** is a general term for skin inflammation, often presenting with redness, itching, and sometimes blisters. - It does not typically involve the specific constellation of oral ulcers, photosensitivity, and a malar rash that spares nasolabial folds. *Psoriasis* - **Psoriasis** is a chronic autoimmune disease primarily affecting the skin, characterized by red, scaly patches (plaques) [2]. - While it can cause nail changes and sometimes joint pain, it does not present with photosensitivity, oral ulcers, or the characteristic malar rash described.