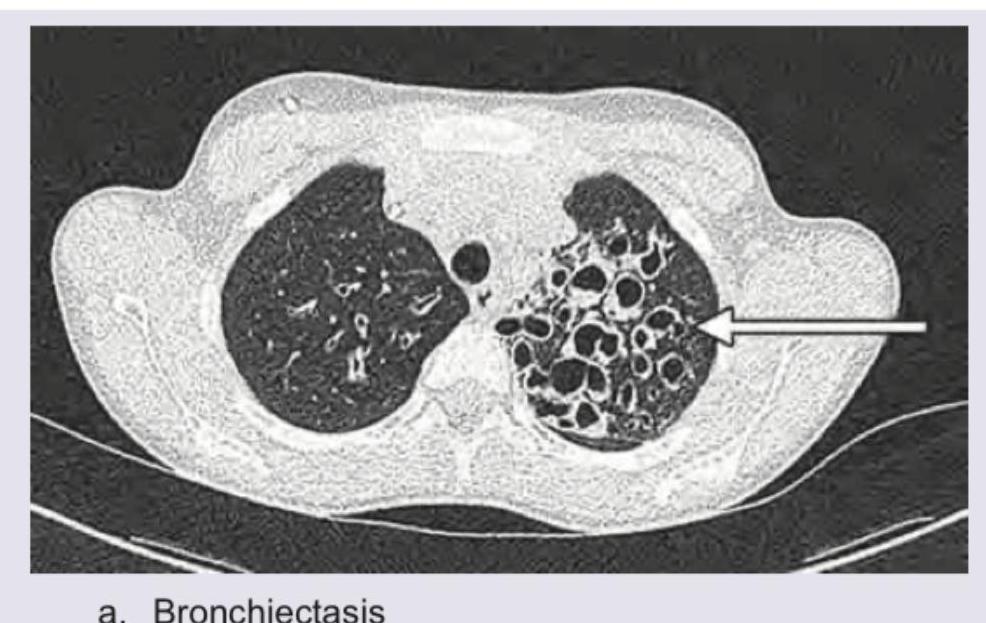
A cement slab fell on the chest of a 20-year-old construction worker. The arrow in the given CT chest points to:
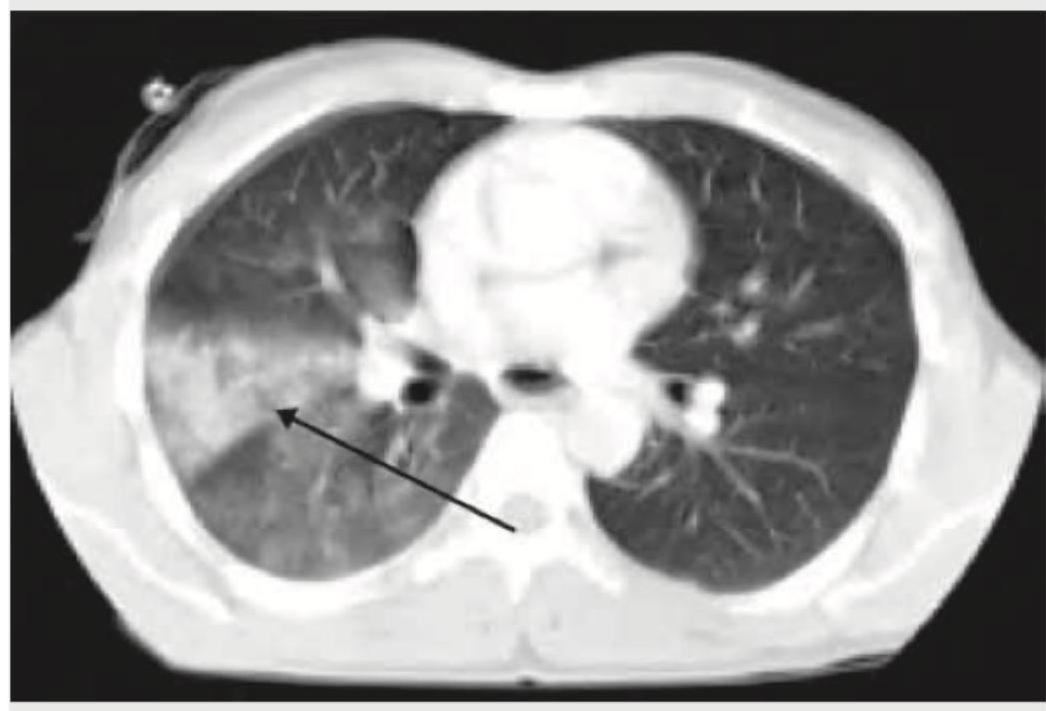
A 25-year-old patient underwent surgery for scoliosis correction. 5 days post-operatively he develops voluminous bilious vomiting. The given CT abdomen shows:
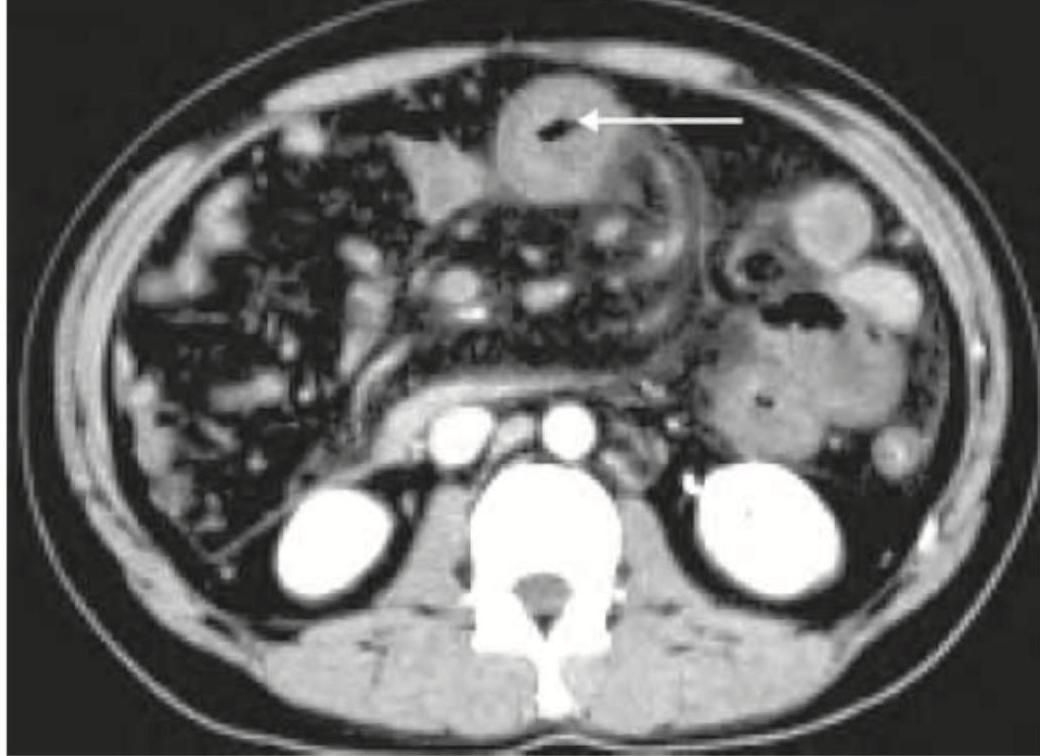
Excretory urogram in a two-year-old child with recurrent UTI shows:
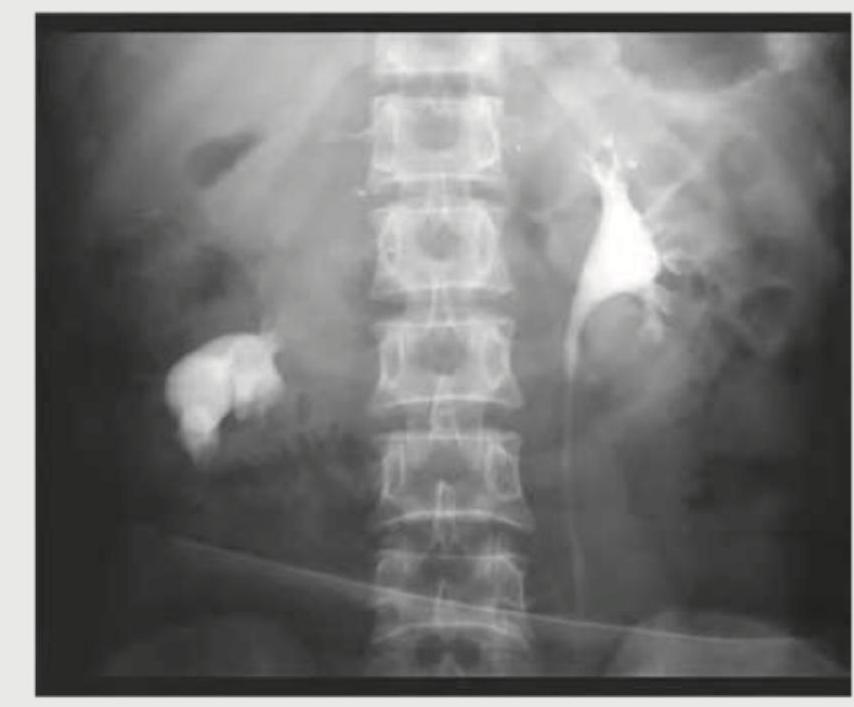
What is the radiological sign that could best describe this image?
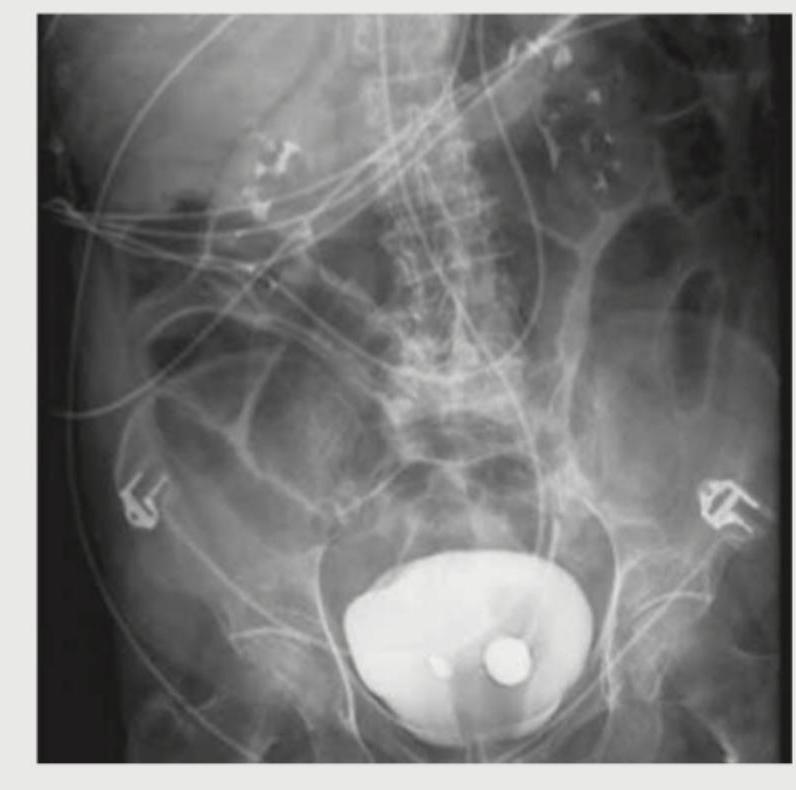
A 26-year-old construction worker with a previous history of recurrent kidney stones presents with flank pain. What is the radiological sign demonstrated in the IVP image shown below?
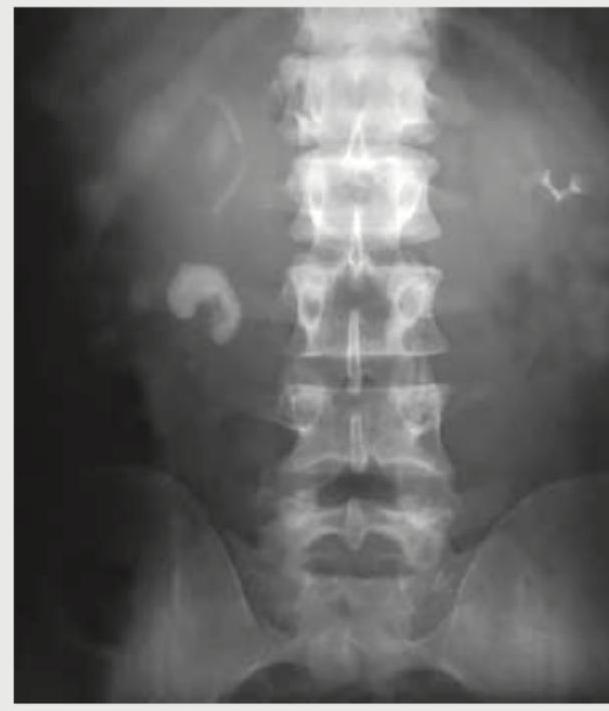
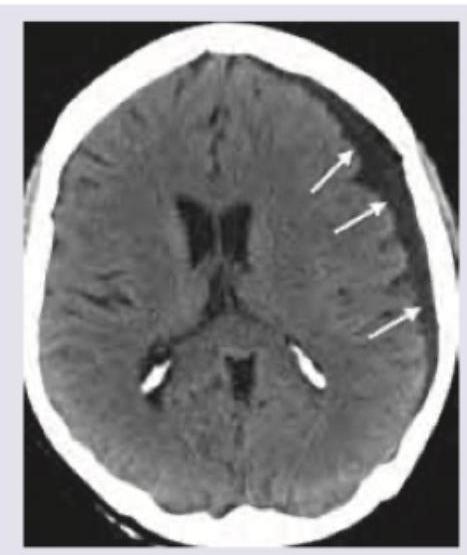
Which of the following is correct about the NCCT shown below? (Recent NEET Pattern 2016-17)
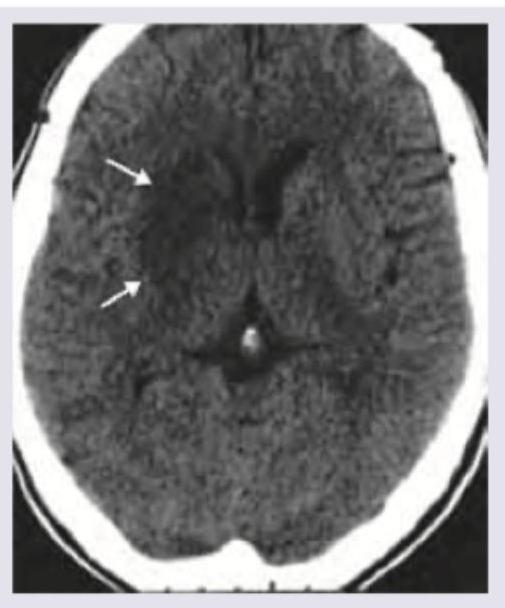
All are true about CNS malformation shown below except:
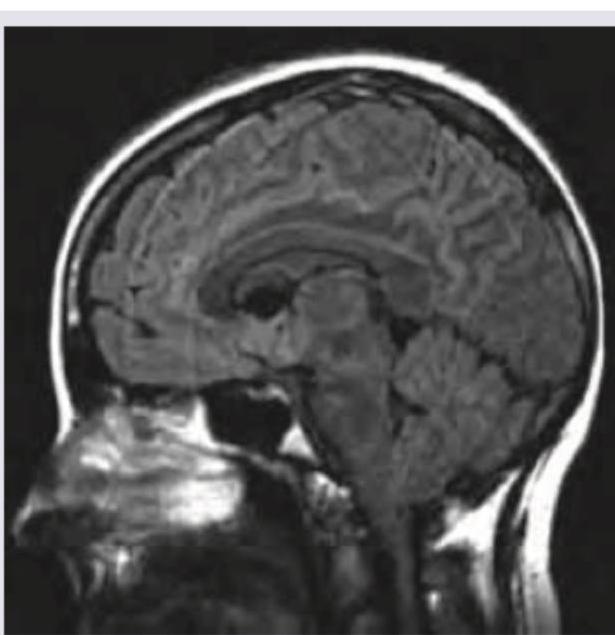
Which is correct about the intracranial bleeding shown below?
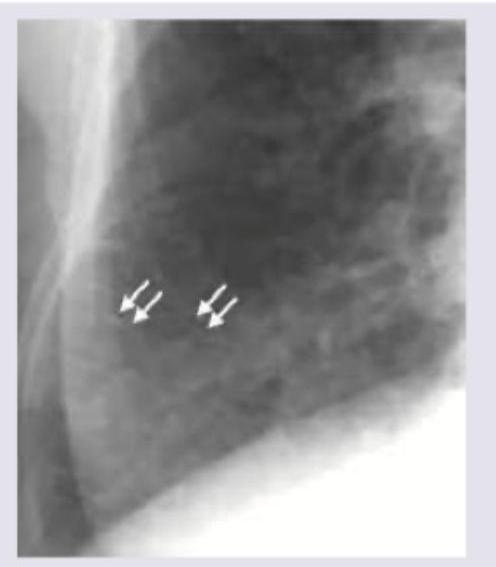
The CXR shows markings near the costophrenic angle. Which of the following is the cause of these markings? (Recent NEET Pattern 2016-17)
The CT chest of a patient given below shows presence of: (Recent NEET Pattern 2016-17)