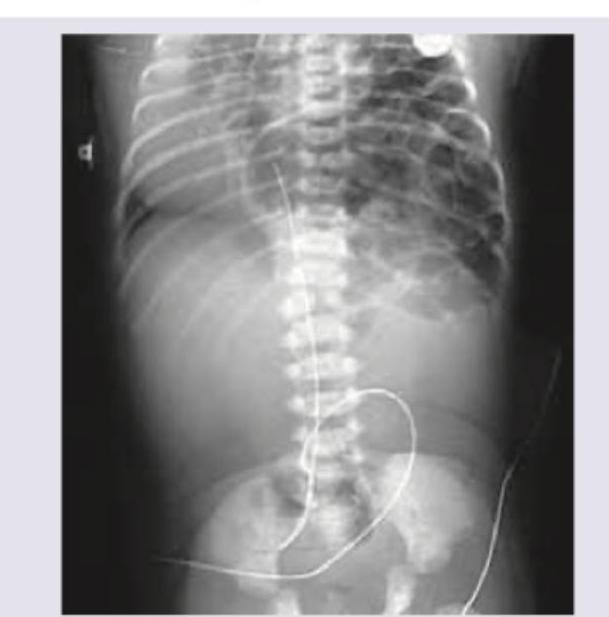
All investigations are useful in work up of this condition except:
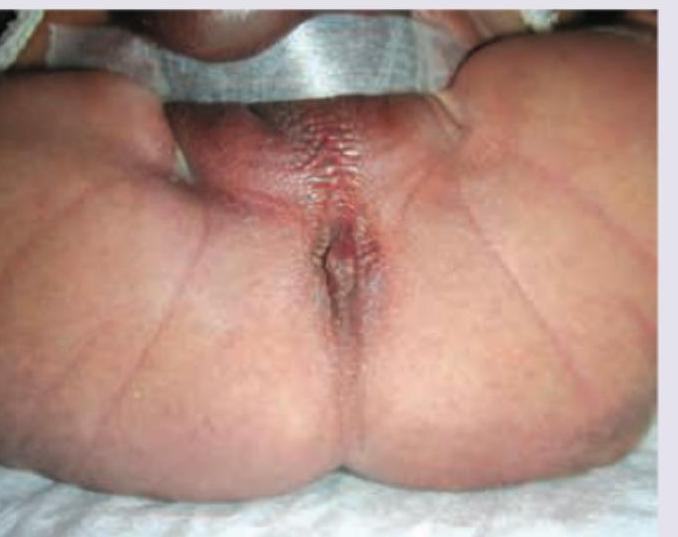
A 2-day-old neonate under phototherapy unit. For exchange transfusion serum bilirubin-albumin ratio should be: (Recent NEET Pattern 2016-17)
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
All investigations are useful in work up of this condition except:

A 2-day-old neonate under phototherapy unit. For exchange transfusion serum bilirubin-albumin ratio should be: (Recent NEET Pattern 2016-17)
Which of the following infections in most commonly seen in this transfusion dependant child shown below?
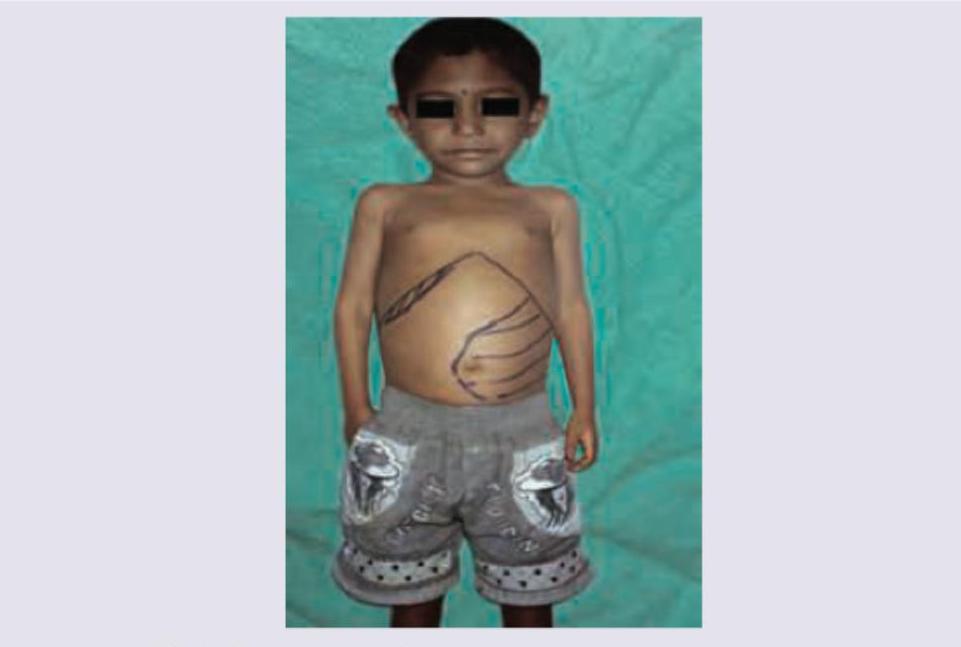
A 3-year-old child has presented with abdominal lump and peculiar appearance of eyes. All genes are responsible for development of this condition except:
Child has not passed stool by 2nd day of life. X-Ray study done shows:
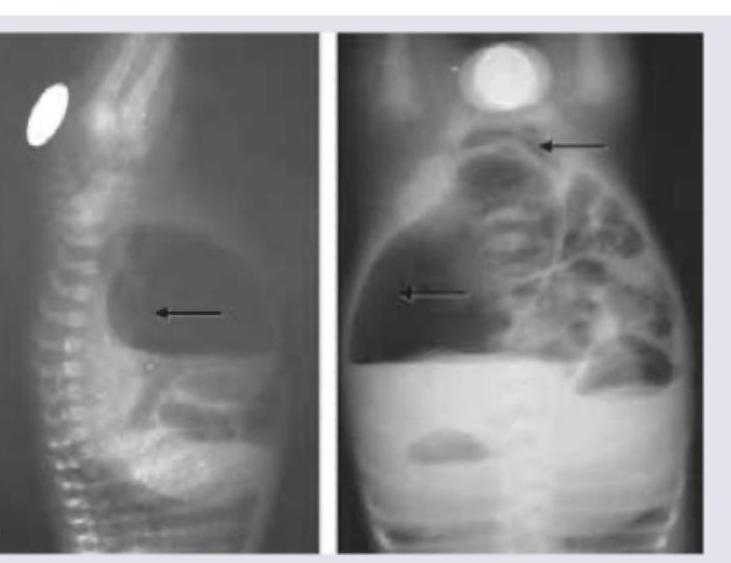
A neonate presents with the clinical features shown in the image below. What is the most likely diagnosis?
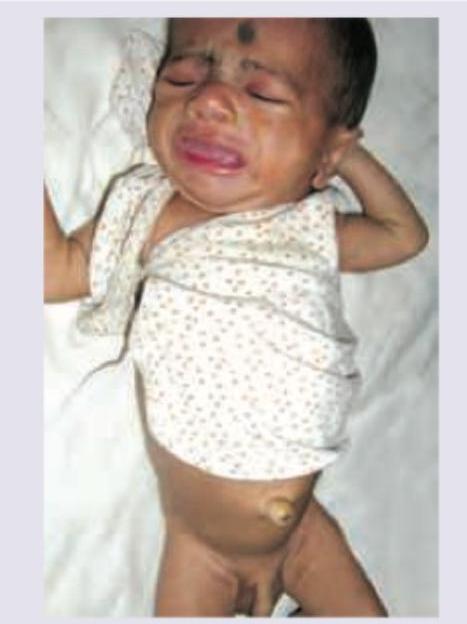
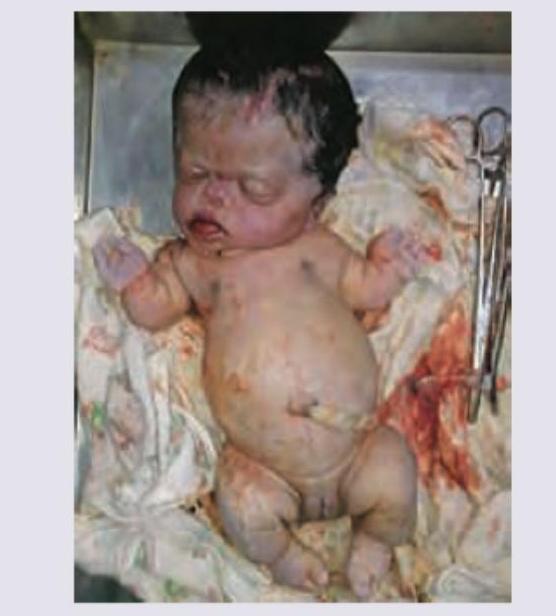
A newborn presents with macrosomia, plethoric appearance, and generalized edema. The image shows:
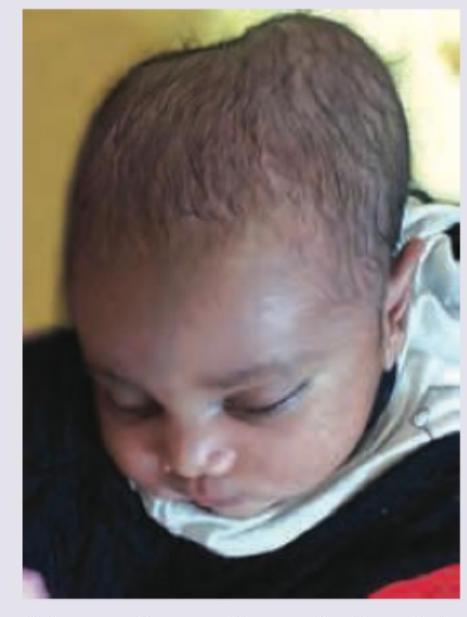
All are true about the swelling on scalp of a 2-day old neonate except: (Recent NEET Pattern 2016-17)
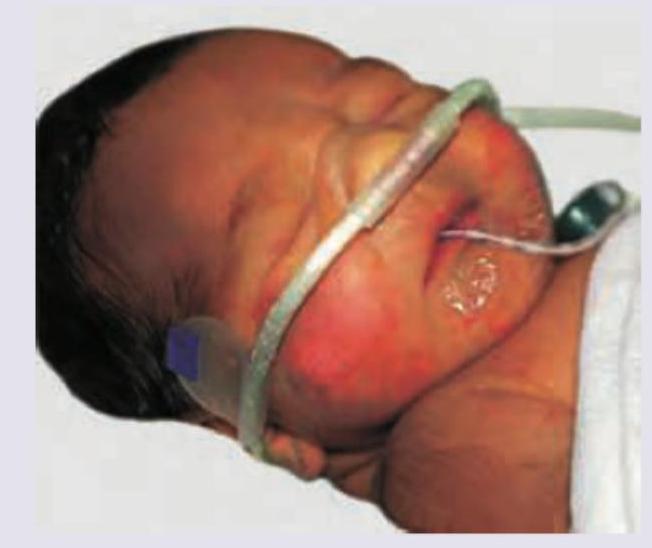
Which of the following interventions is being done in this neonate?
Identify the condition on the basis of infantogram shown in the image: