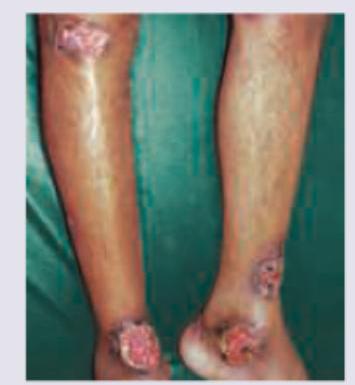
A 45-year-old Ulcerative colitis patient presents with multiple painful lesions on both legs. What is the diagnosis?
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
A 45-year-old Ulcerative colitis patient presents with multiple painful lesions on both legs. What is the diagnosis?

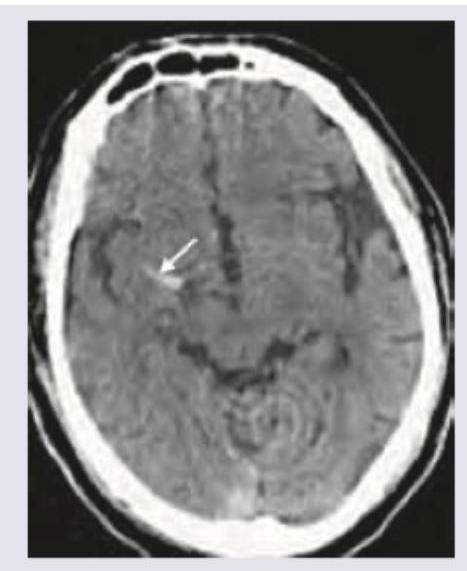
A 55-year-old diabetic patient develops sudden onset hemiparesis and facial asymmetry. NCCT scan shows:
A 35-year-old woman presents with breathlessness at rest. She also complains of a skin lesion on nose which has increased in size for last 6 months. What is the diagnosis?
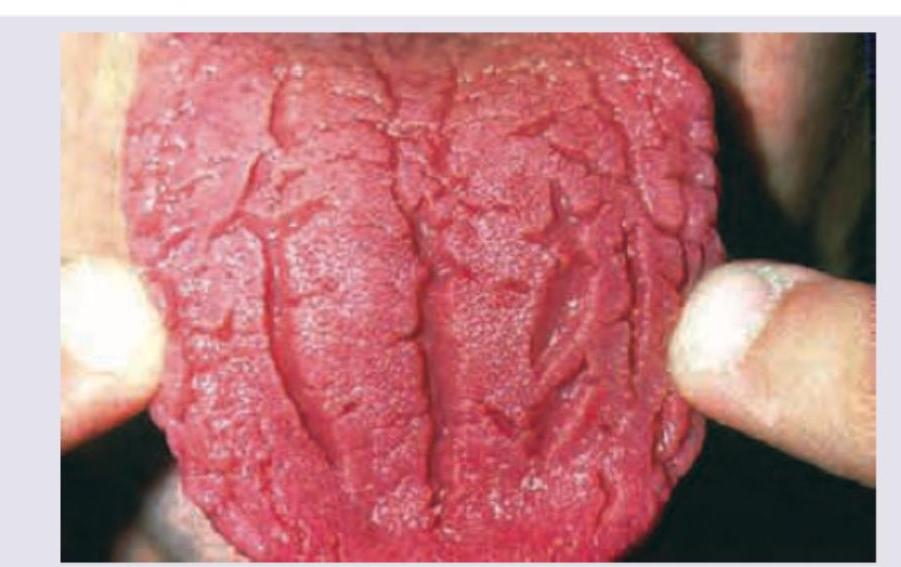
All are causes of following tongue appearance except: (Recent NEET Pattem 2016-17)
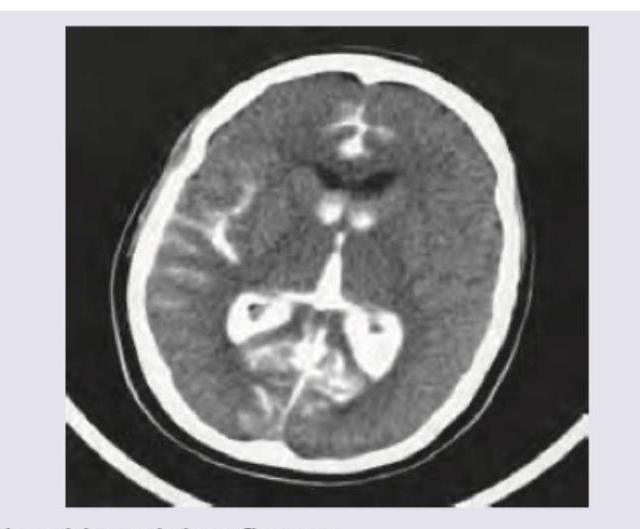
A patient presents with GCS of 7 with nuchal rigidity and bloody CSF. Which is incorrect regarding this condition? (Recent NEET Pattern 2016-17)
A patient of swine flu has developed severe respiratory distress. Which of the following findings confirm the diagnosis of ARDS in this patient?
What is the correct diagnosis based on the image shown below?
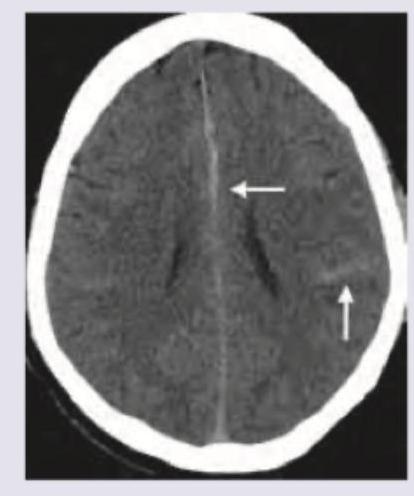
Which is correct about the intracranial bleeding shown below?
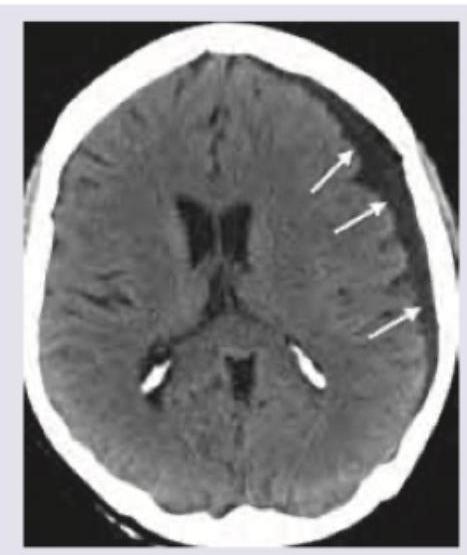
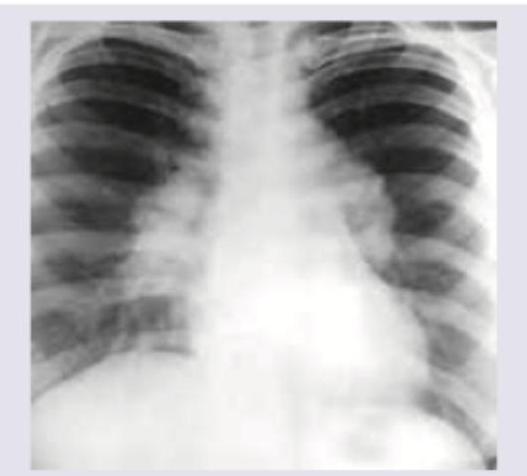
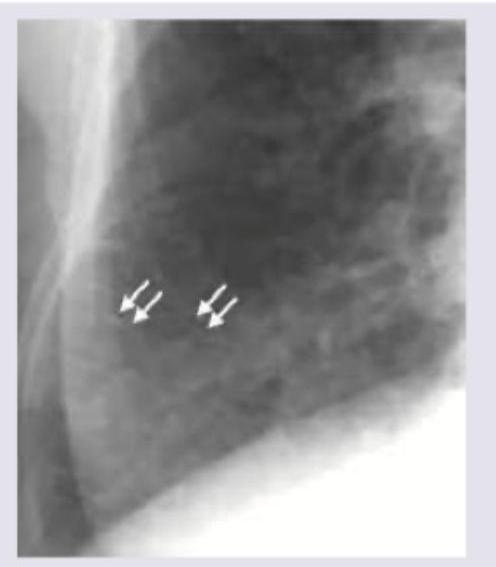
The CXR shows markings near the costophrenic angle. Which of the following is the cause of these markings? (Recent NEET Pattern 2016-17)
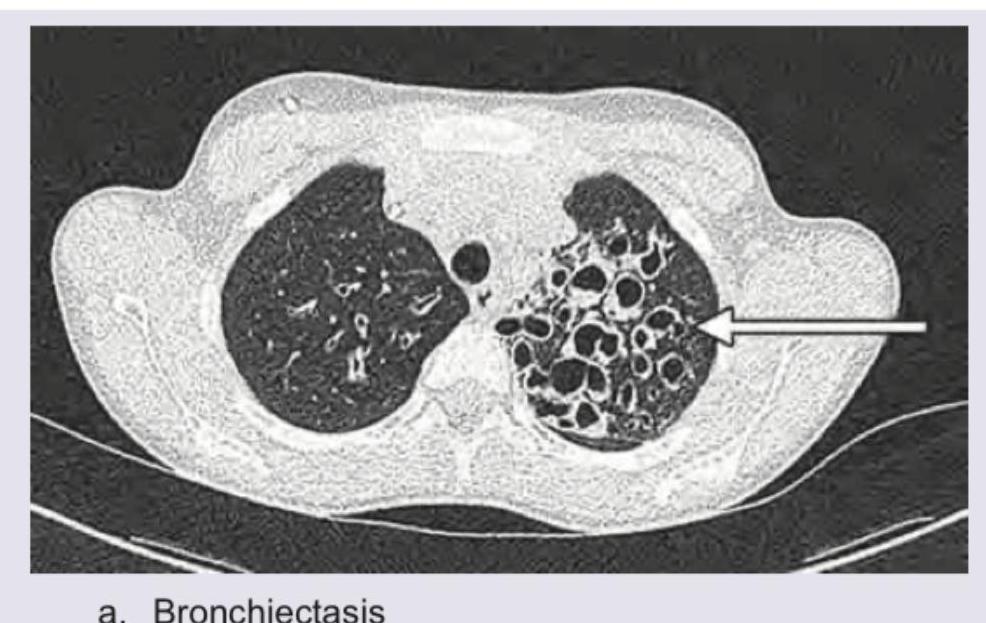
The CT chest of a patient given below shows presence of: (Recent NEET Pattern 2016-17)