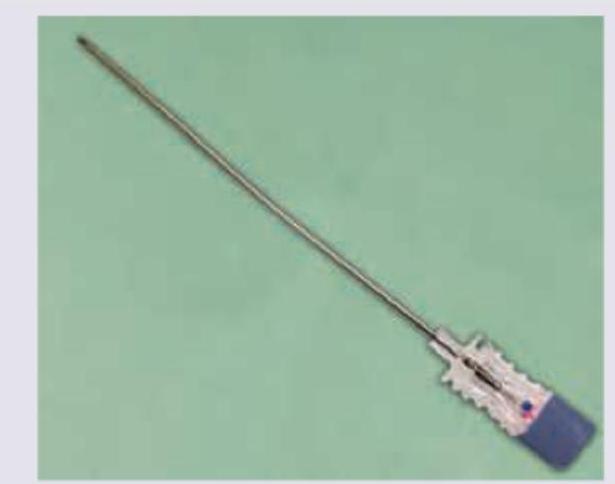
All of the following layers are pierced by the needle shown below except:
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
All of the following layers are pierced by the needle shown below except:

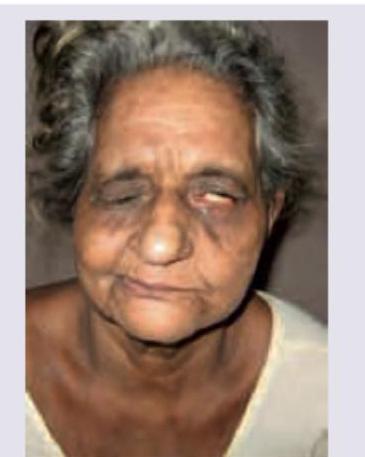
A 79-year-old male presented to the emergency department after a facial trauma. The patient had Parkinson's disease and atrial fibrillation and was on treatment with acetylsalicylic acid for AF. The image shows? (Recent NEET Pattern 2016-17)
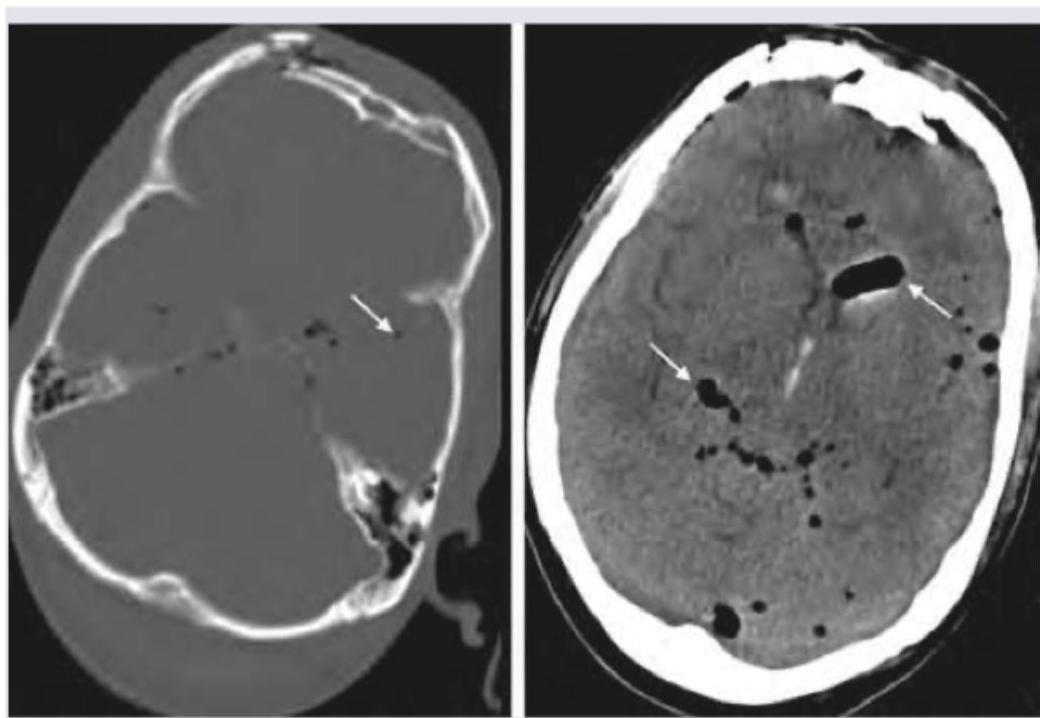
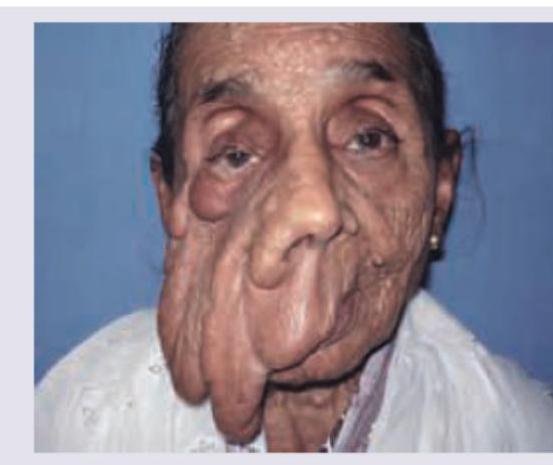
Identify the lesion. (Recent NEET Pattern 2016-17)
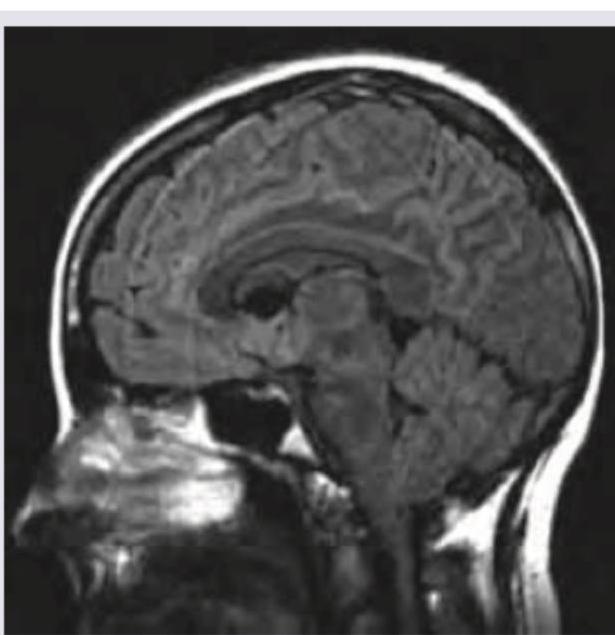
MRI was performed on a 35-year-old man with progressive myoclonus and apathy. What is the diagnosis? (Recent NEET Pattern 2016-17)
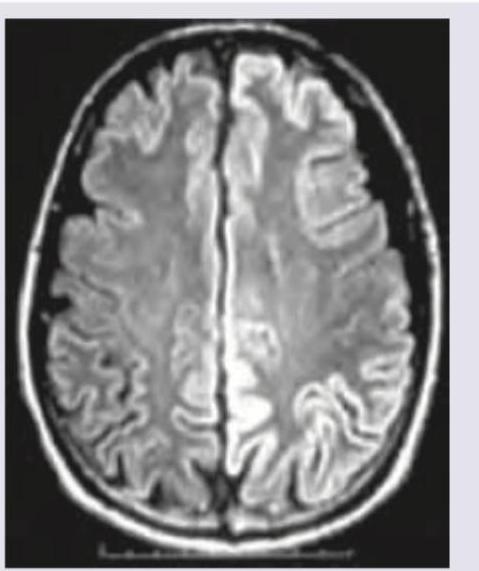
A 35-year-old woman presents with thunderclap headache. NCCT was done. All are true about the condition except:
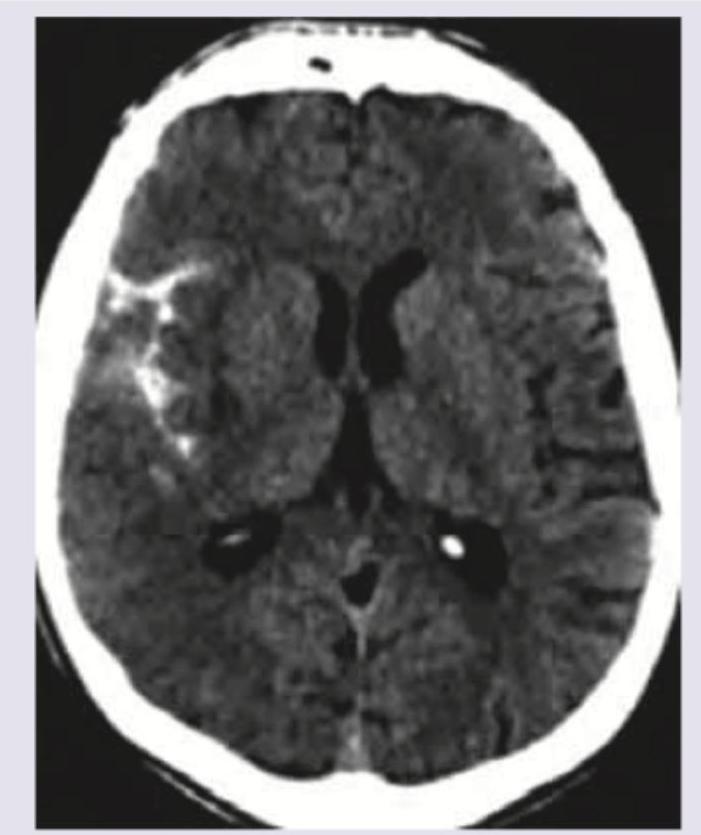
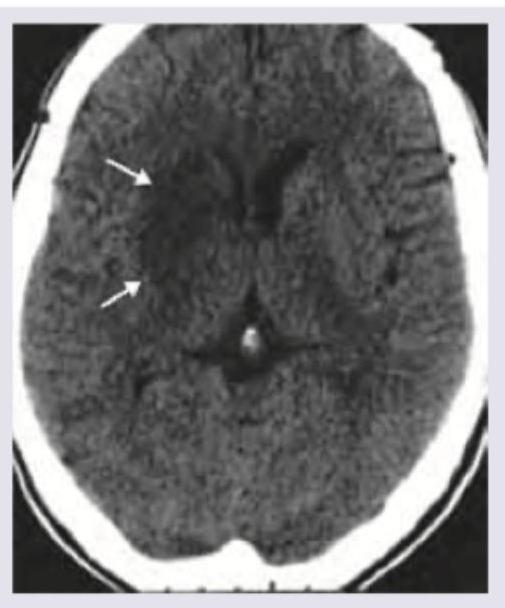
A 50-year-old hypertensive patient develops sudden onset drooping of right face and hemiplegia. What is the diagnosis?
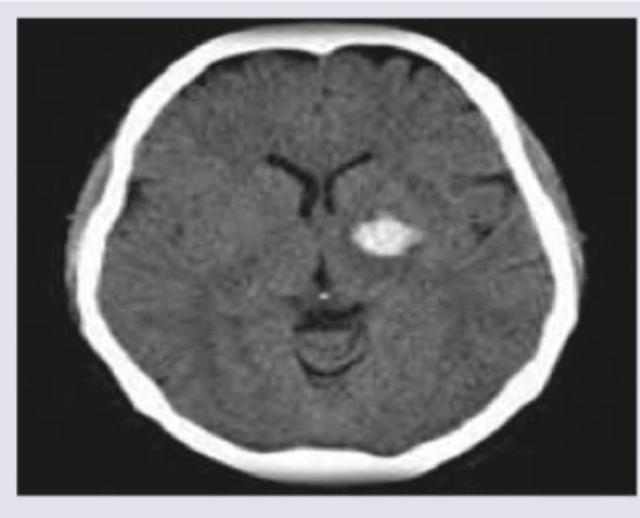
A 2-year-old epileptic child with developmental delay presents to emergency with fever for the last two days. NCCT shows:
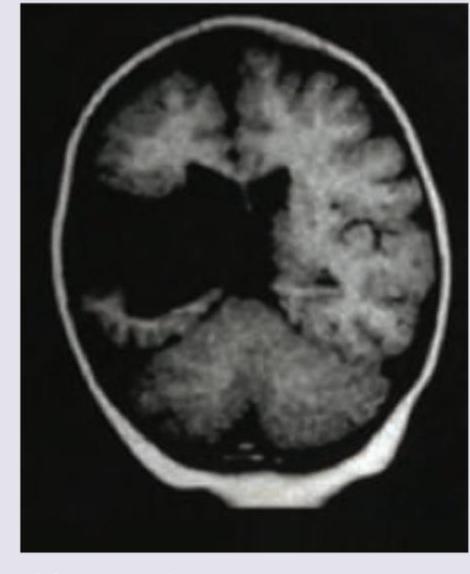
Comment on the diagnosis based on the image shown below. (Recent NEET Pattern 2016-17)
Which of the following is correct about the NCCT shown below? (Recent NEET Pattern 2016-17)
All are true about CNS malformation shown below except: