All (353)Anatomy (30)Anesthesiology (8)Biochemistry (8)Community Medicine (15)Dermatology (23)ENT (17)Forensic Medicine (18)General Medicine (2)Internal Medicine (22)Internal Medicine (5)Microbiology (39)Obstetrics and Gynecology (15)Ophthalmology (16)Orthopaedics (10)Pathology (14)Pathology (10)Pediatrics (24)Pharmacology (5)Physiology (15)Radiology (31)Surgery (4)Surgery (22)
Q321
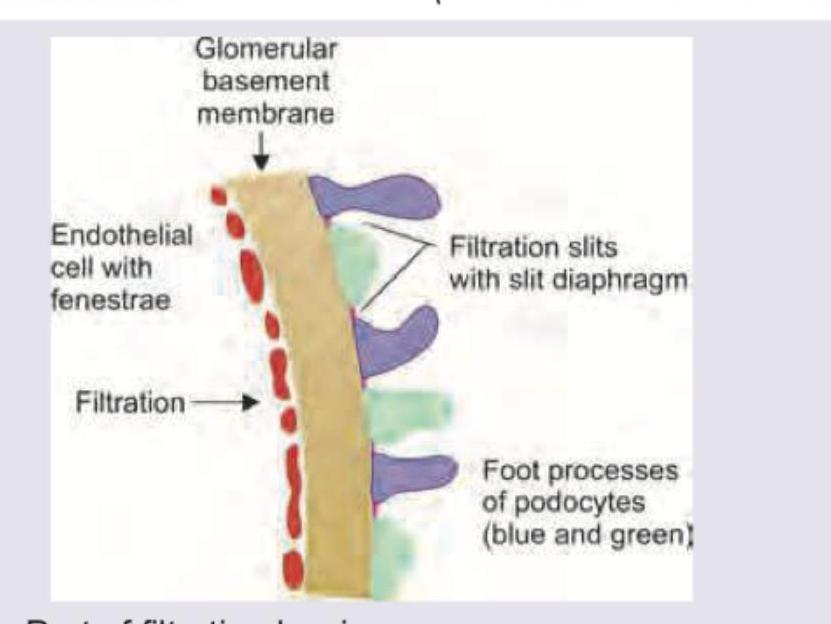
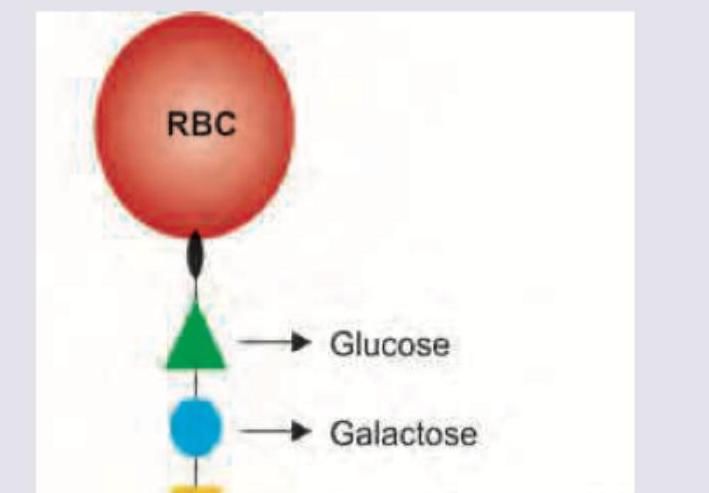
What is incorrect about the shown basement membrane?