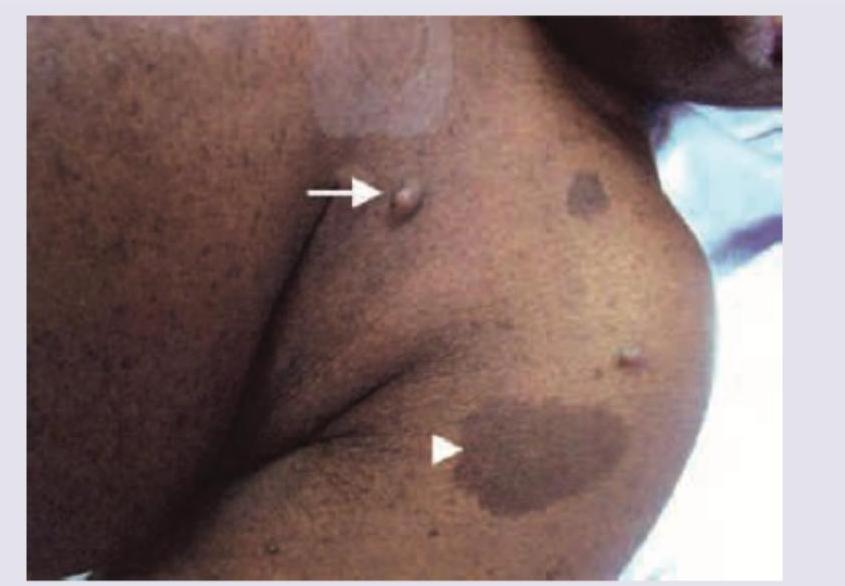
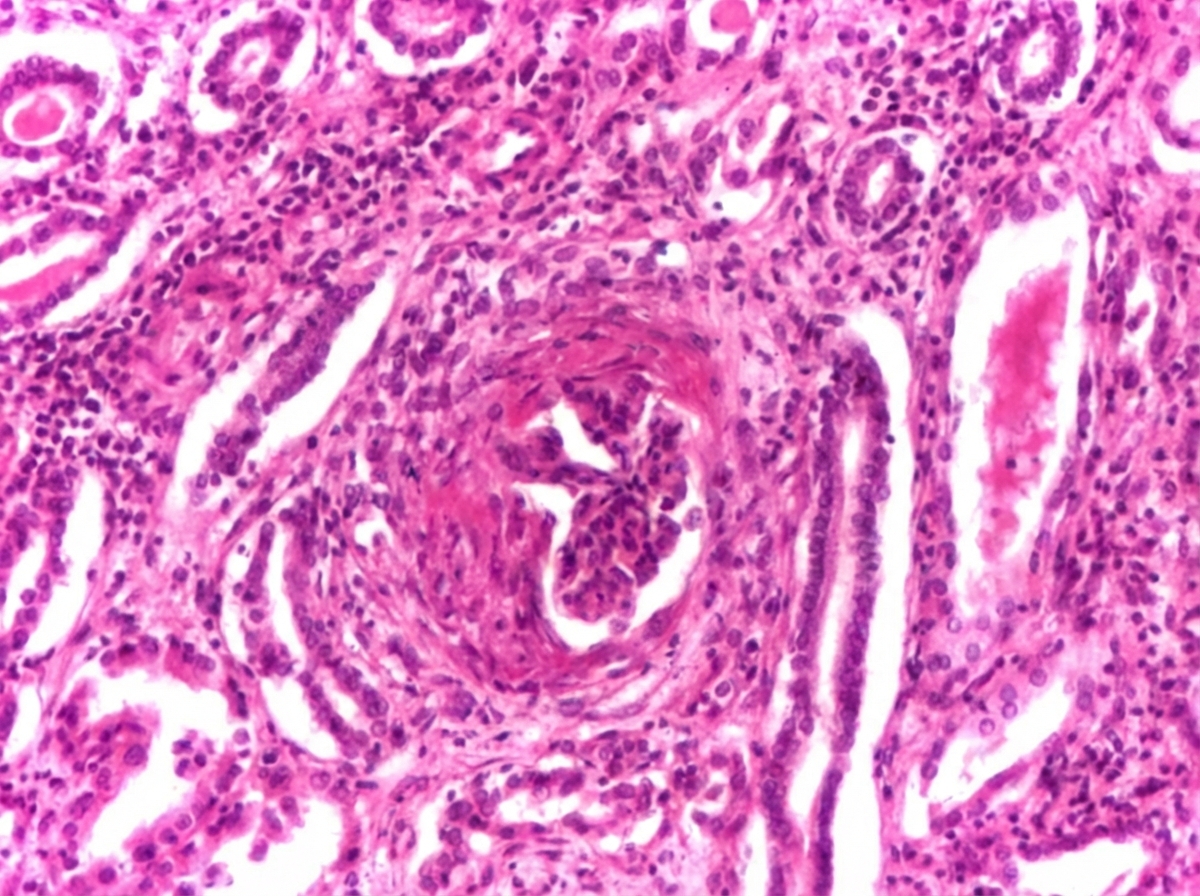
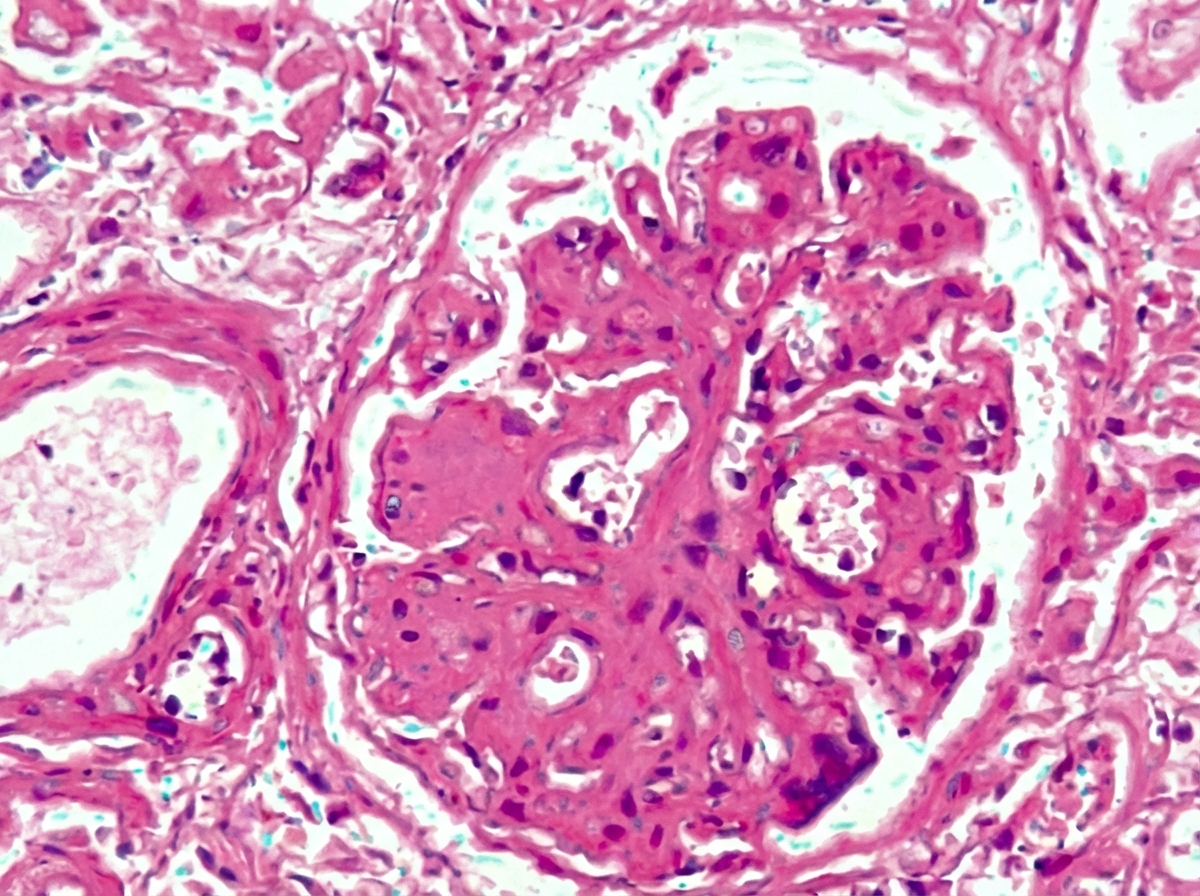
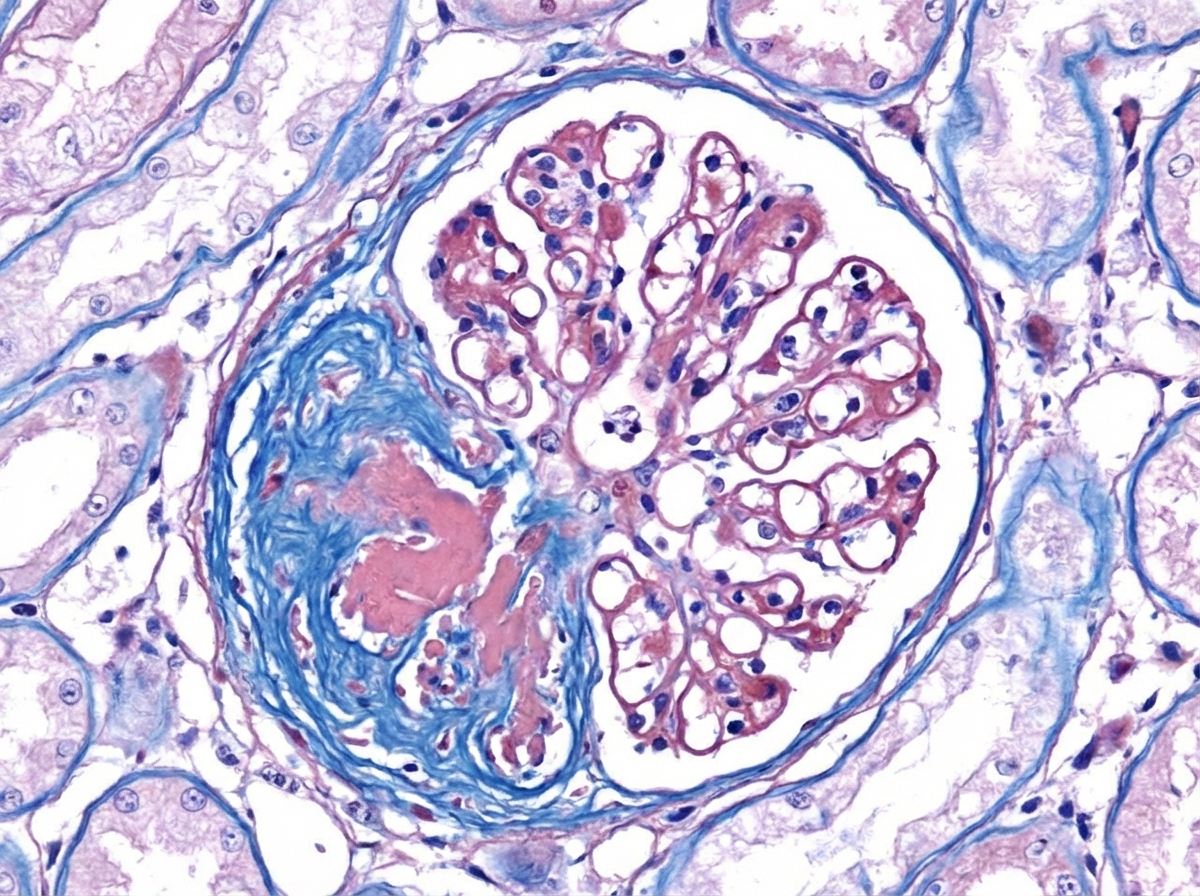
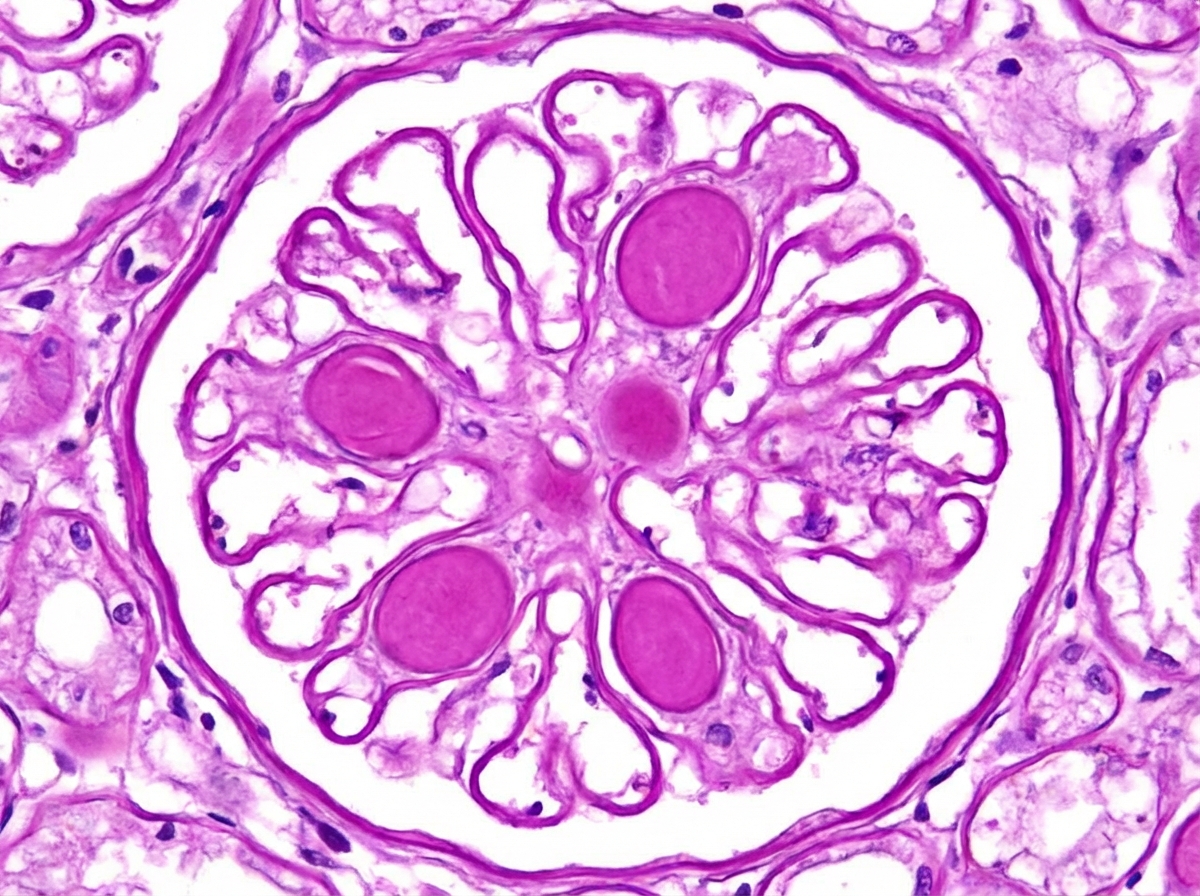
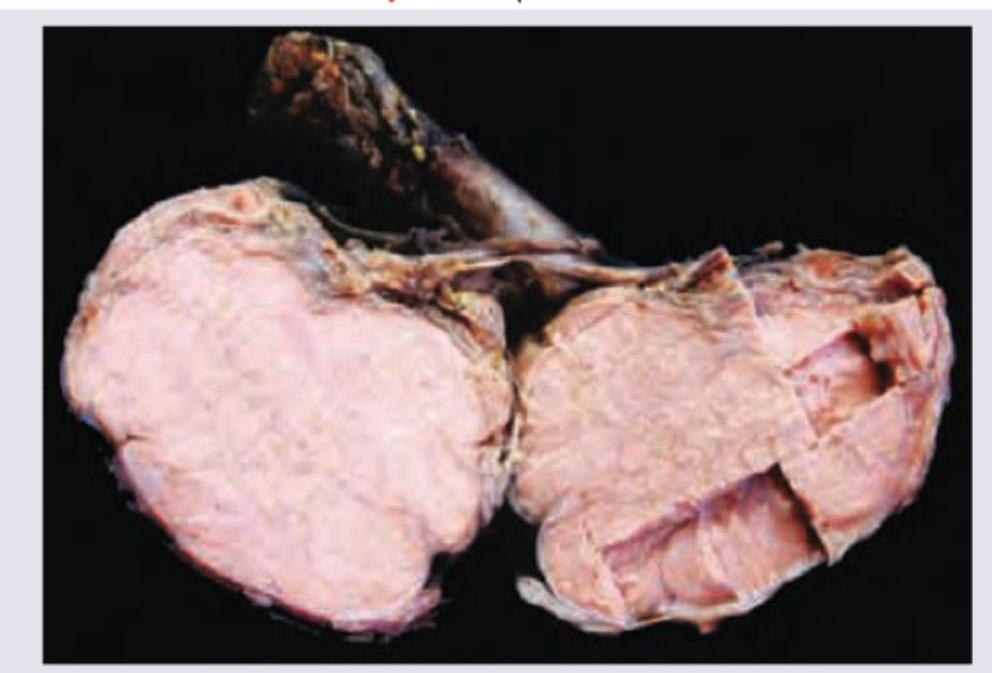
A 38-year-old man presents with the manifestation shown in the image. He has a number of family members suffering from the same condition, though the severity is different in different members. Which of the following statements is false regarding this condition?