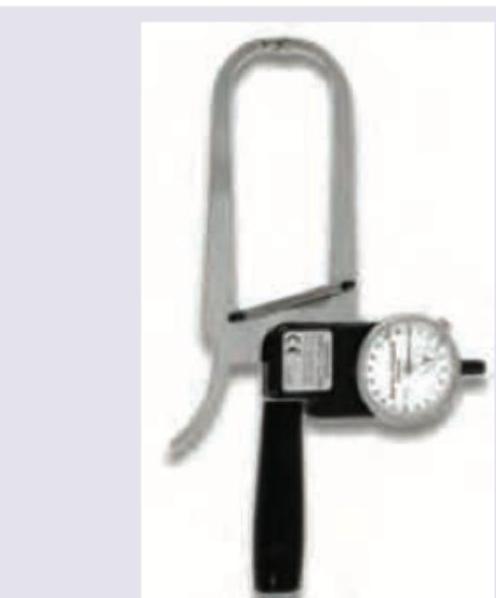
The following instrument is used for the measurement of: (Recent NEET Pattern 2016-17)
The image shows a special ward in a district hospital. What is it called and what should be the minimum number of beds?

Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
The following instrument is used for the measurement of: (Recent NEET Pattern 2016-17)

The image shows a special ward in a district hospital. What is it called and what should be the minimum number of beds?

The image shows:
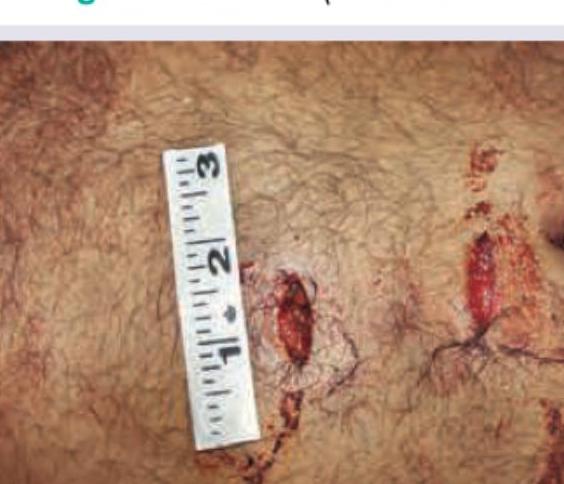
A 12-year-old boy presents with difficulty in reading from the blackboard in school. Initially refraction error was considered but visual acuity was normal. He has started complaining of diplopia on watching TV or after studying for long. He takes very long time to finish his meals and his speech becomes very difficult to understand after speaking continuously for few minutes. Anti-Acetylcholine receptor blocking antibody is detected in high titers. All are done in management except? (Recent NEET Pattern 2016-17)
A 65-year-old patient of dilated cardiomyopathy was prescribed 1 mg warfarin tablet for sustained atrial fibrillation. The chemist however gave him 2 mg tablets by mistake which resulted in him developing hemorrhagic complications (bleeding). CT scan is performed. This is which kind of ADR? (Recent NEET Pattern 2016-17) Warfarin Sodium Tablets, USP Crystalline 2 mg Protect from light
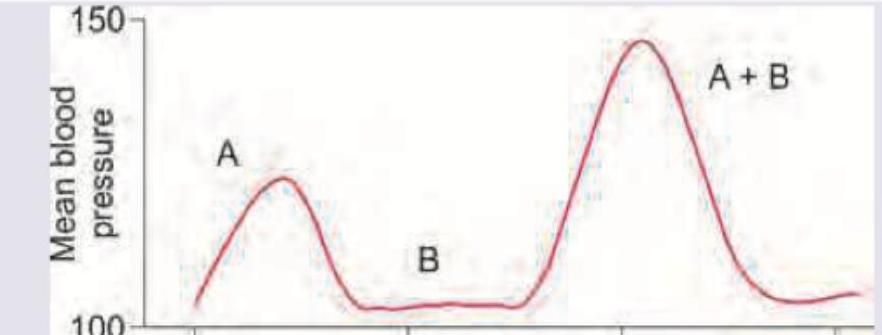
The effect of both drugs given together on the blood pressure of a patient was evaluated in comparison with the effect of individual drugs on BP. The following curve represents: (Recent NEET Pattern 2016-17)
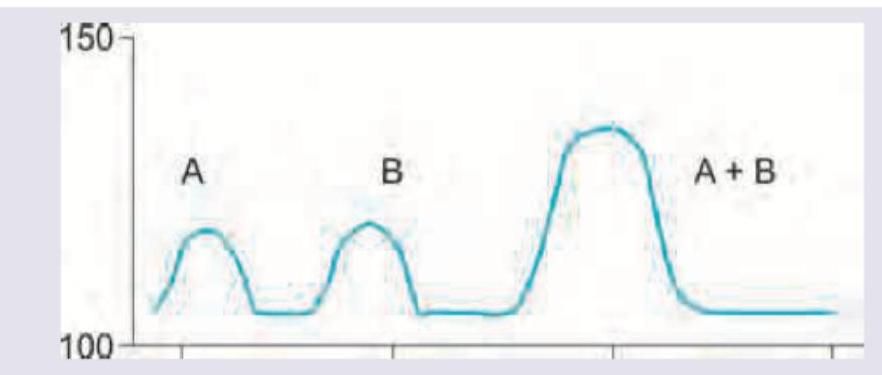
Drug A is epinephrine and drug B is cocaine. The effect of both drugs given together on the blood pressure of a patient was evaluated in comparison with effect of individual drugs on BP. The following curve represents:
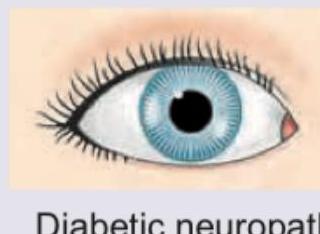
A 20-year-old woman is admitted with the following presentation. 1% pilocarpine is not showing any response on the side of mydriasis. What is the diagnosis? (Recent NEET Pattern 2016-17)
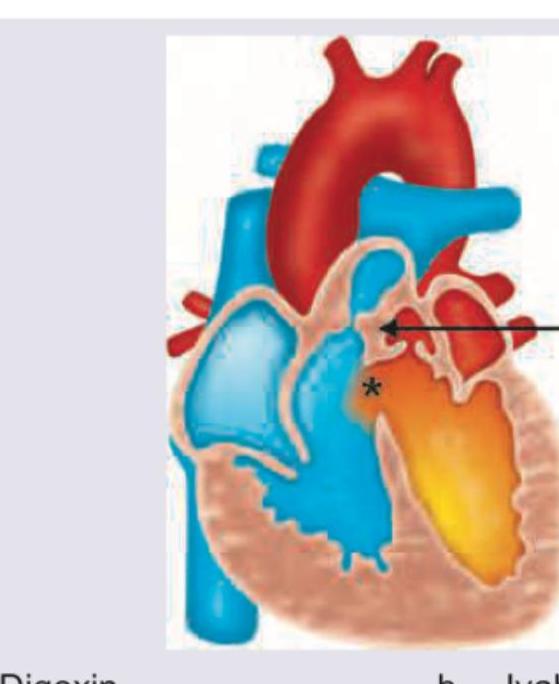
A neonate presents with a congenital heart disease as shown below. Which drug should be started immediately? (Recent NEET Pattern 2016-17)
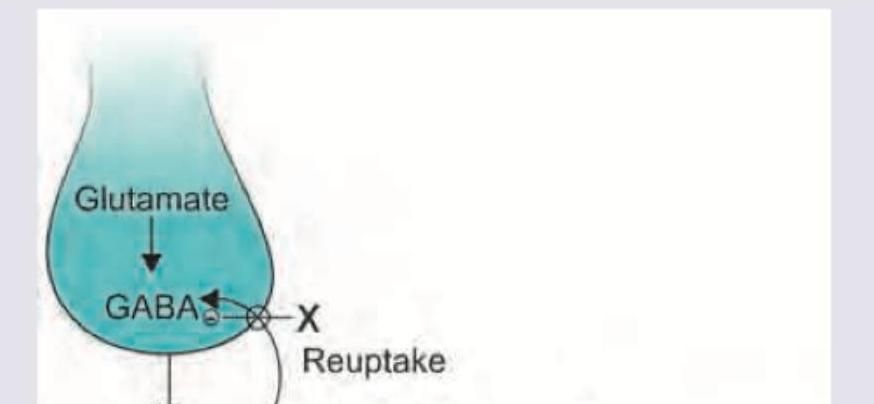
Which anti-epileptic drug marked X will act at the site shown?