The patient with the following hematological abnormality presents with severe chest pain and difficulty in breathing. All are useful for managing this emergency except:
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
The patient with the following hematological abnormality presents with severe chest pain and difficulty in breathing. All are useful for managing this emergency except:

A 60-year-old hypertension patient presents with breathlessness. ECG was performed. What is the diagnosis? (Recent NEET Pattern 2016-17)
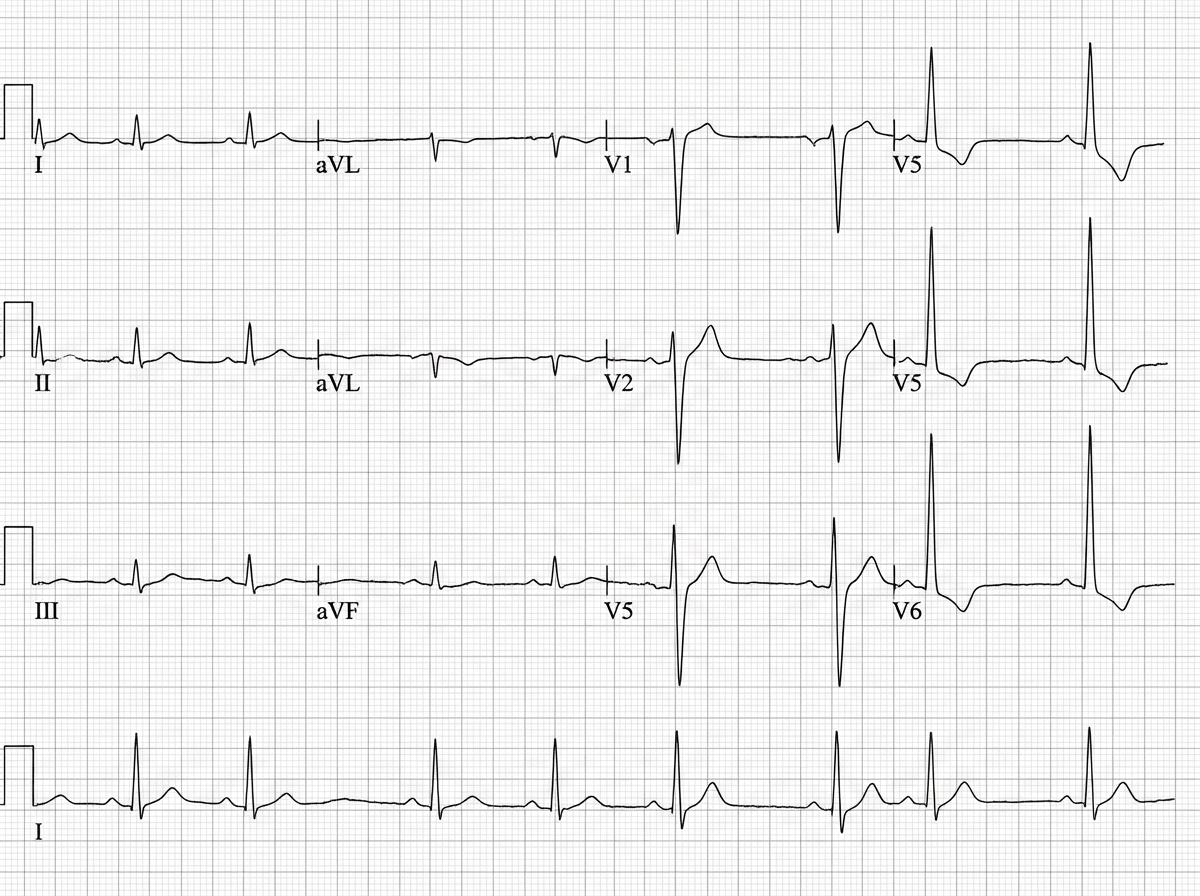
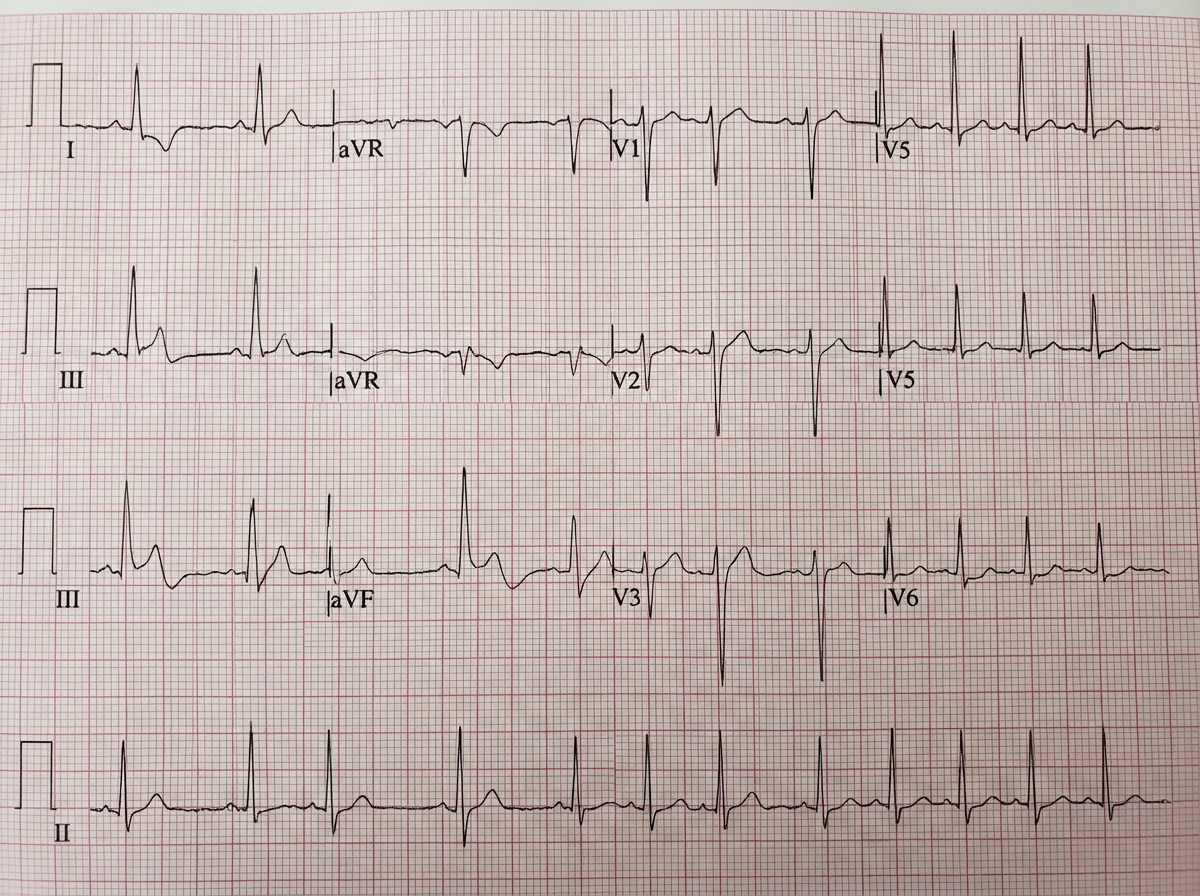
A 50-year-old smoker comes with complaints of ankle edema for last 3 months. The ECG shows all except: (Recent NEET Pattern 2016-17)
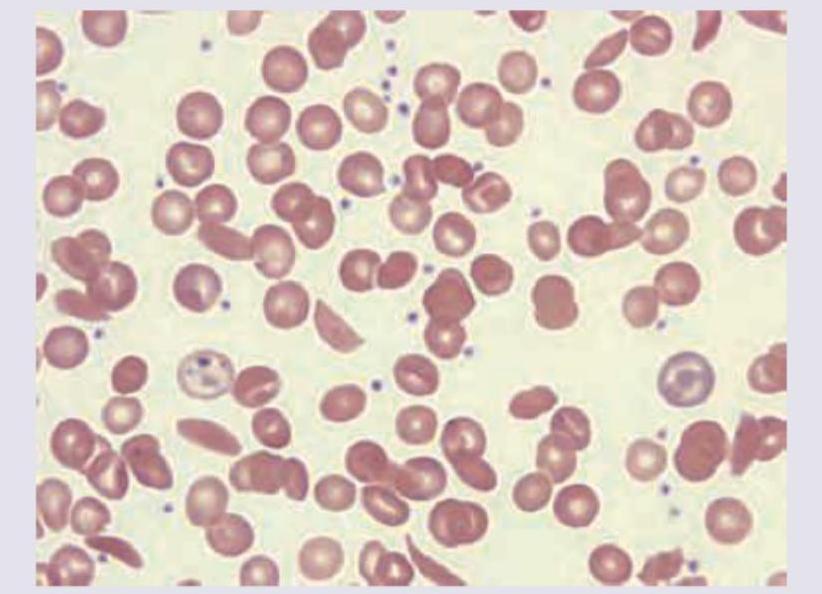
A 70-year-old man presents with painless cervical lymphadenopathy with progressive pallor and petechiae on ankles. Peripheral smear shows presence of:
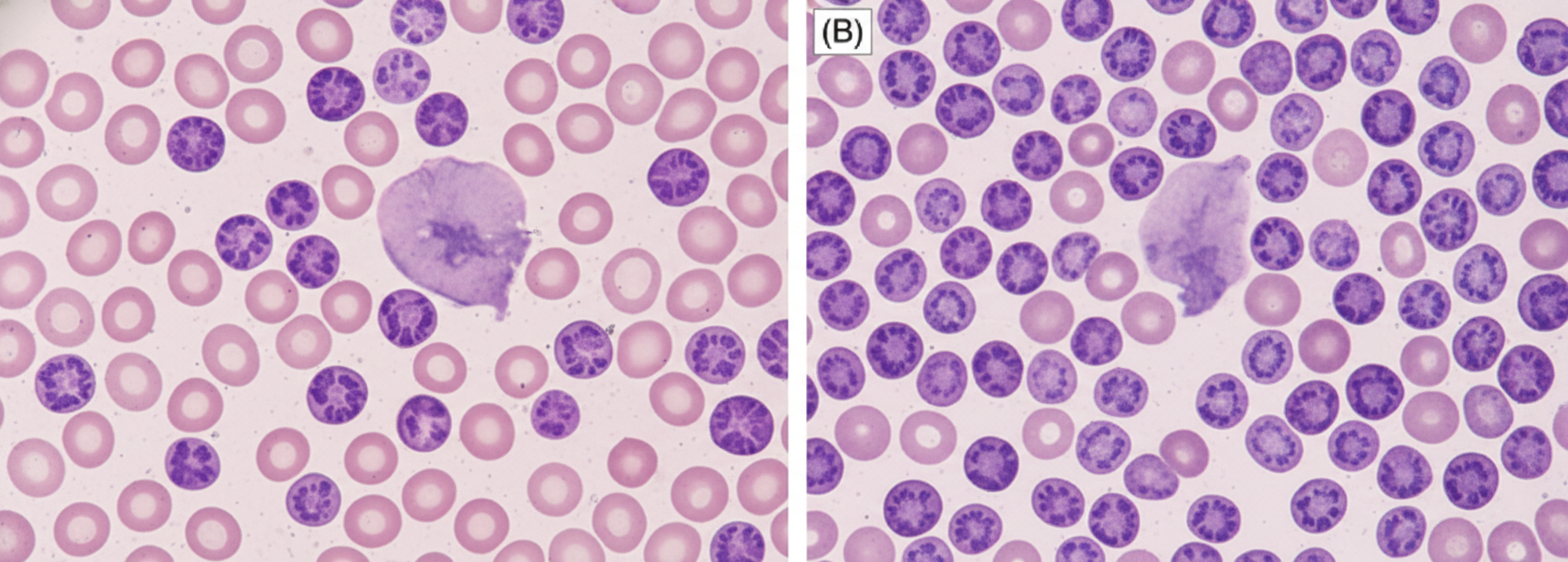
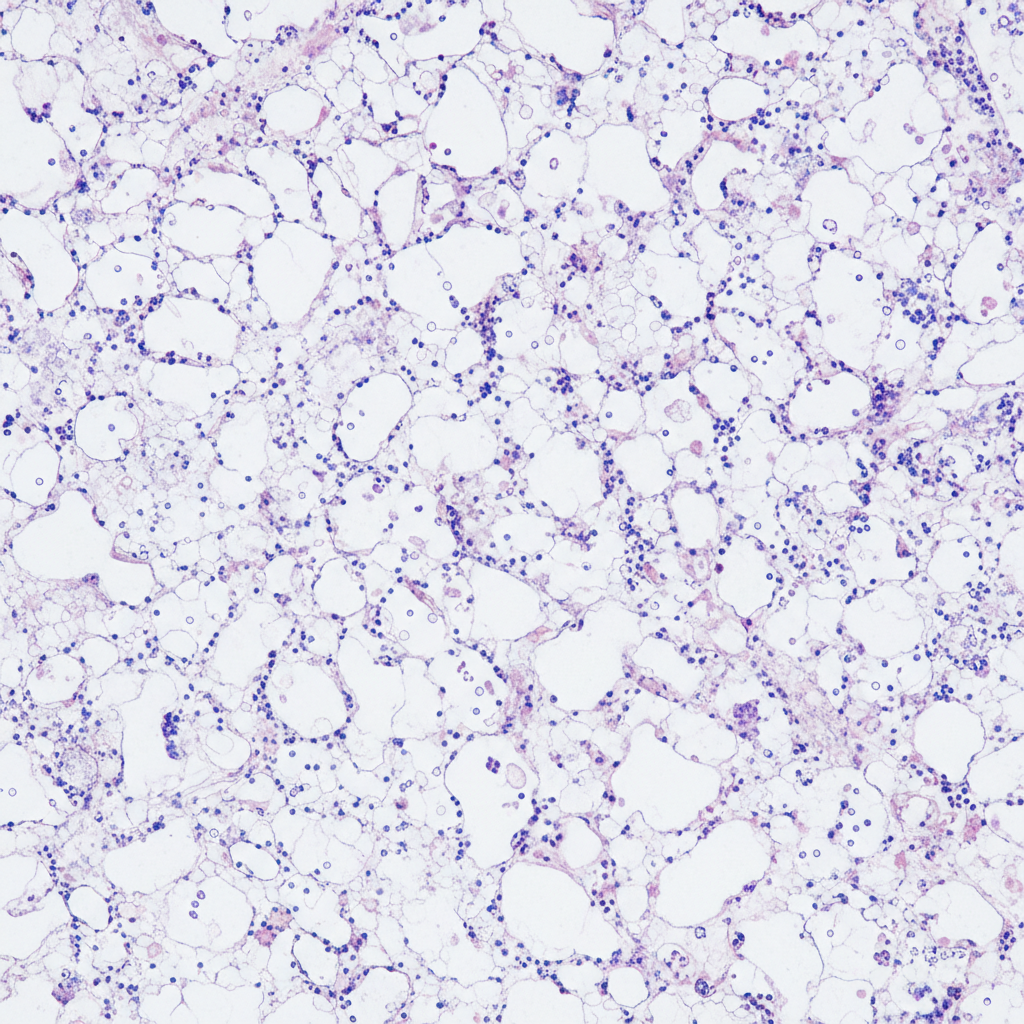
The following bone marrow specimen is suggestive of diagnosis of:
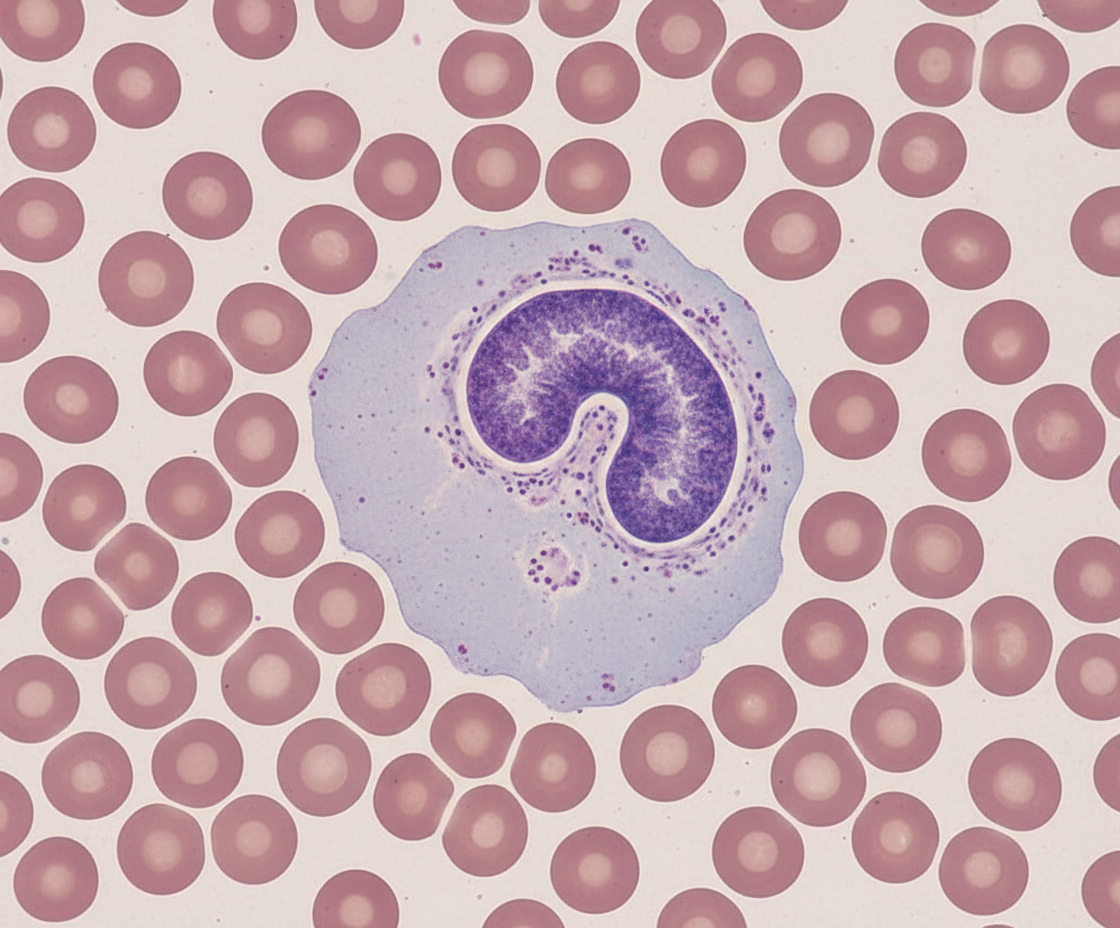
Identify the cell.
Name the test given.

Name the anticoagulant used in the following method.

A 32-year-old male with a history of klebsiella infection presents with right upper quadrant pain and on performing cholecystectomy the following stones were seen. All the following statements are true regarding this condition except: (Recent NEET Pattern 2016-17)

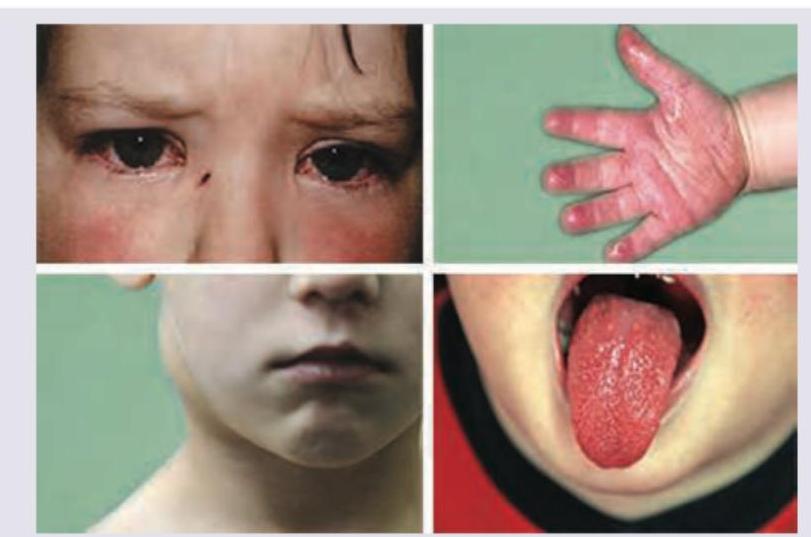
A 3-year-old child presents with the clinical features shown in the image. What is the most likely diagnosis?