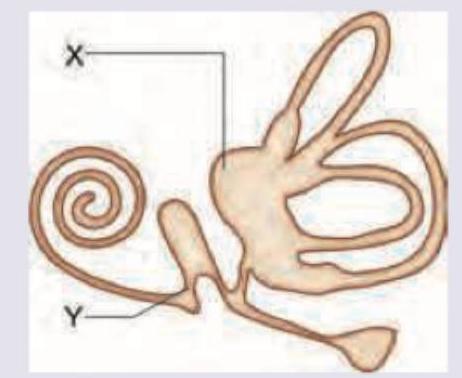
All are correct about the part marked as $X$ and $Y$ except:
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
All are correct about the part marked as $X$ and $Y$ except:

Which of the following is correct about ear speculum insertion?
The test shown below is used for the evaluation of

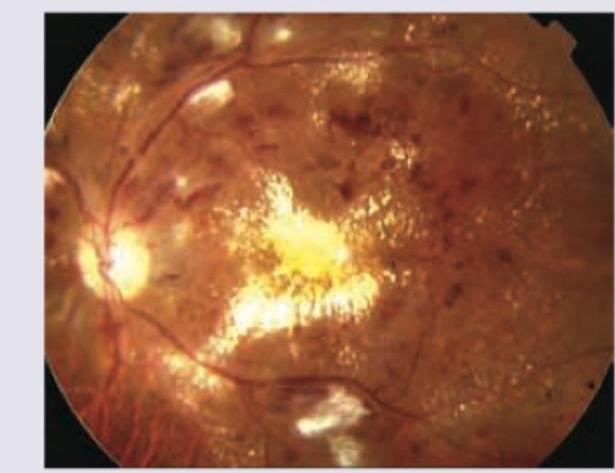
A 60-year-old patient during annual check-up had a report of HbA1C of $10 \%$. What does the given fundus examination show?
All are used for the treatment of the condition shown below except:
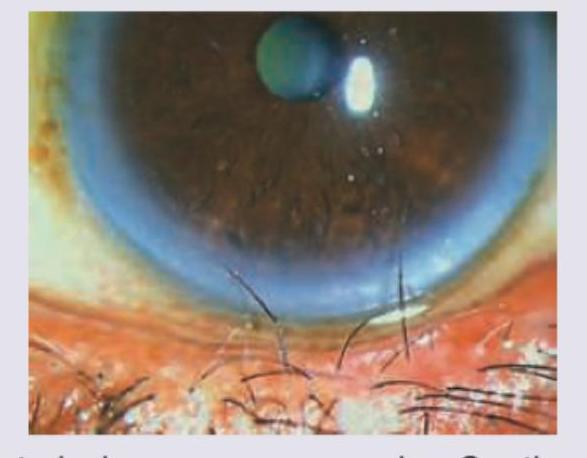
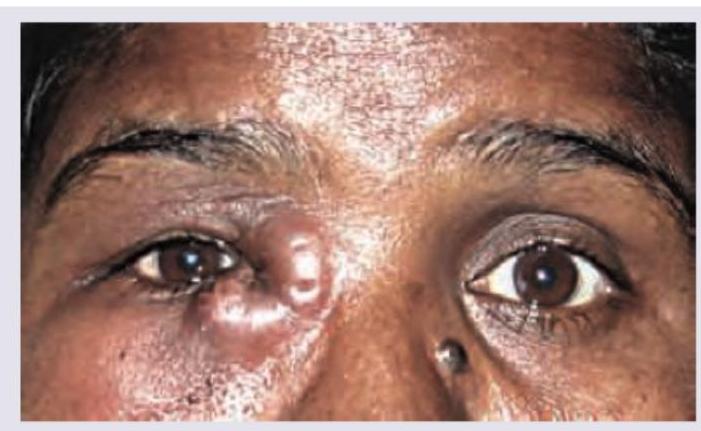
A 30-year-old woman presents with painful eye swelling. Based on the clinical photograph shown, the most likely diagnosis is:
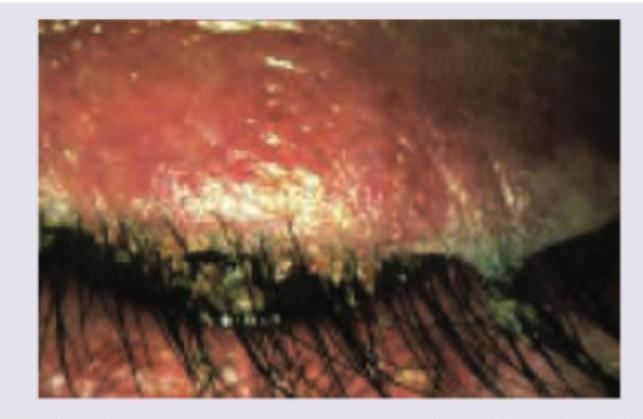
A patient presents with itching in eyes with redness of eyelids. What is correct about the image shown below? (Recent NEET Pattern 2016-17)
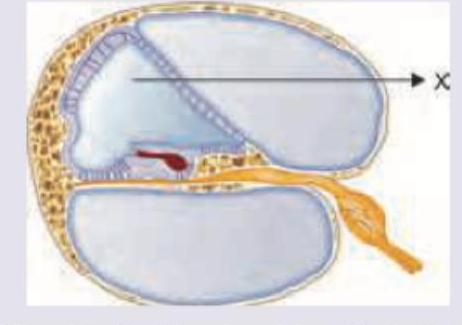
What is correct about the composition of fluid in the area marked as $X$ ?
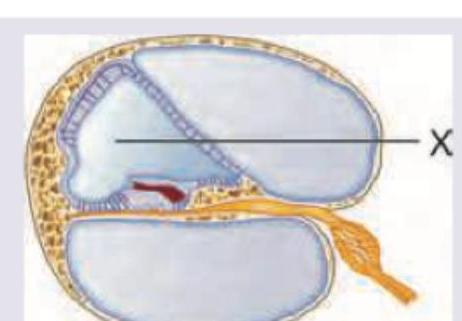
What is correct about the composition of fluid in the area marked as X?
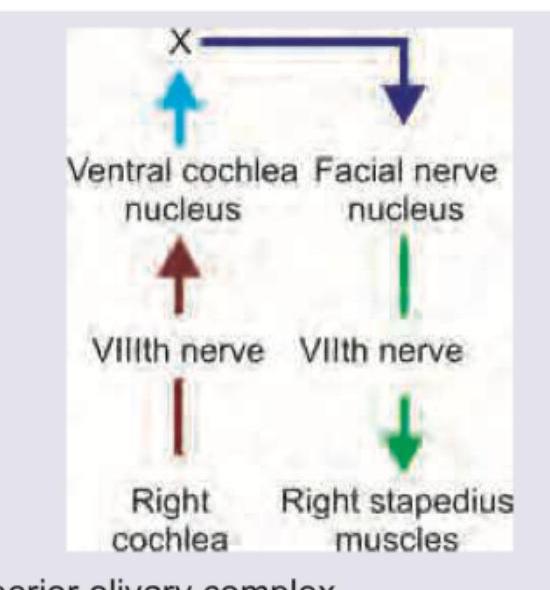
The image given below shows stapedial reflex. What does ' $X$ ' denote?