All (353)Anatomy (30)Anesthesiology (8)Biochemistry (8)Community Medicine (15)Dermatology (23)ENT (17)Forensic Medicine (18)General Medicine (2)Internal Medicine (22)Internal Medicine (5)Microbiology (39)Obstetrics and Gynecology (15)Ophthalmology (16)Orthopaedics (10)Pathology (14)Pathology (10)Pediatrics (24)Pharmacology (5)Physiology (15)Radiology (31)Surgery (4)Surgery (22)
Q151
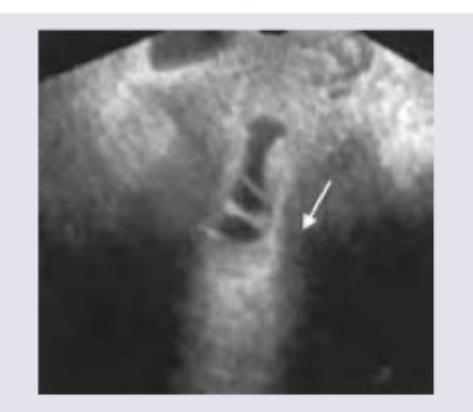
Transvaginal saline infusion sonographic evaluation shows:
Q152
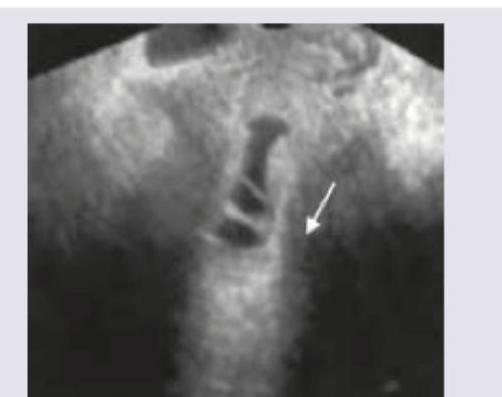
What is the best treatment for the condition shown below?
Q153
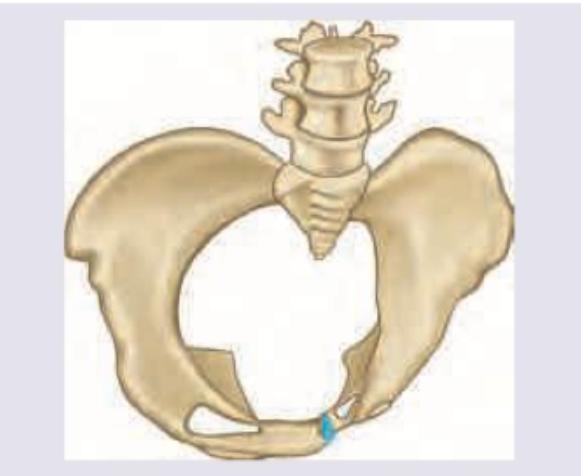
A 25-year-old lady had tubal rupture due to ectopic pregnancy at 6 weeks. The most common site of rupture of ectopic pregnancy amongst the following is:
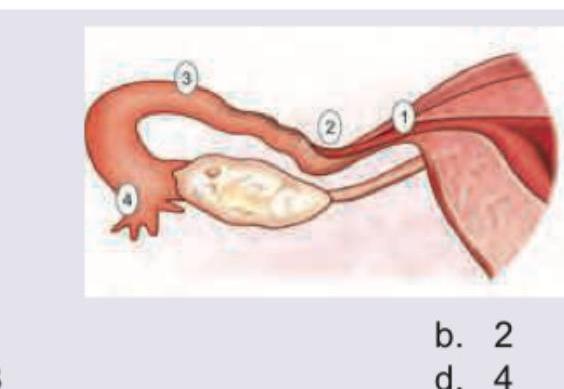
Q154
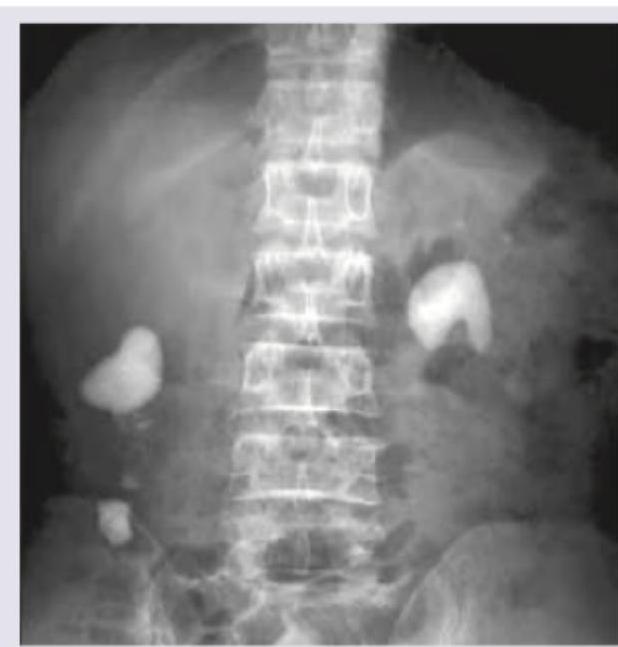
The image shows:
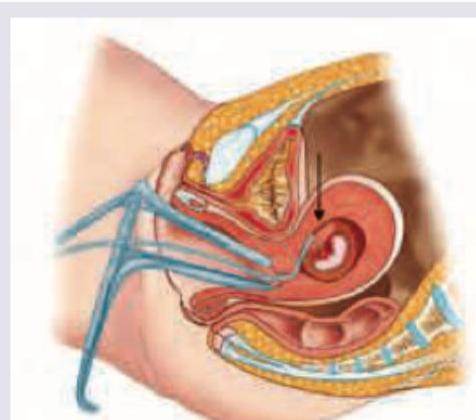
Q155
Which is incorrect about the presentation shown below?
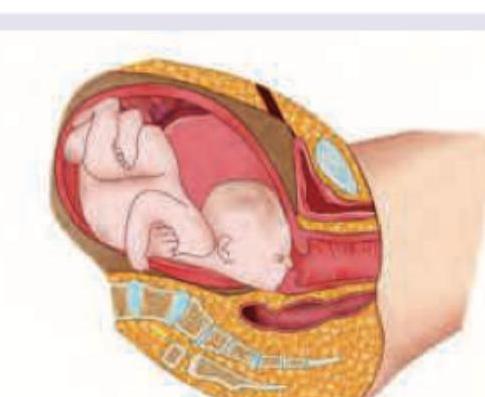
Q156
Which is the least common type of pelvis out of the types shown below?
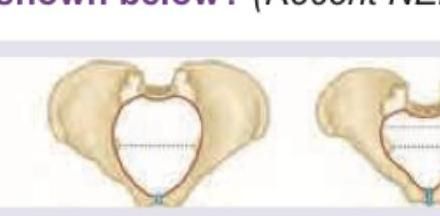
Q157
Which of the following is correct about the placenta shown below? (Recent NEET Pattern 2016-17)
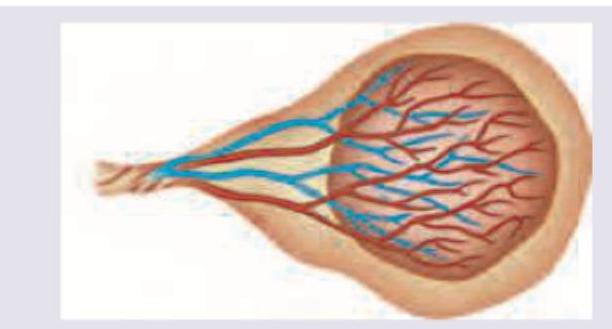
Q158
What is the type of placenta previa shown below?
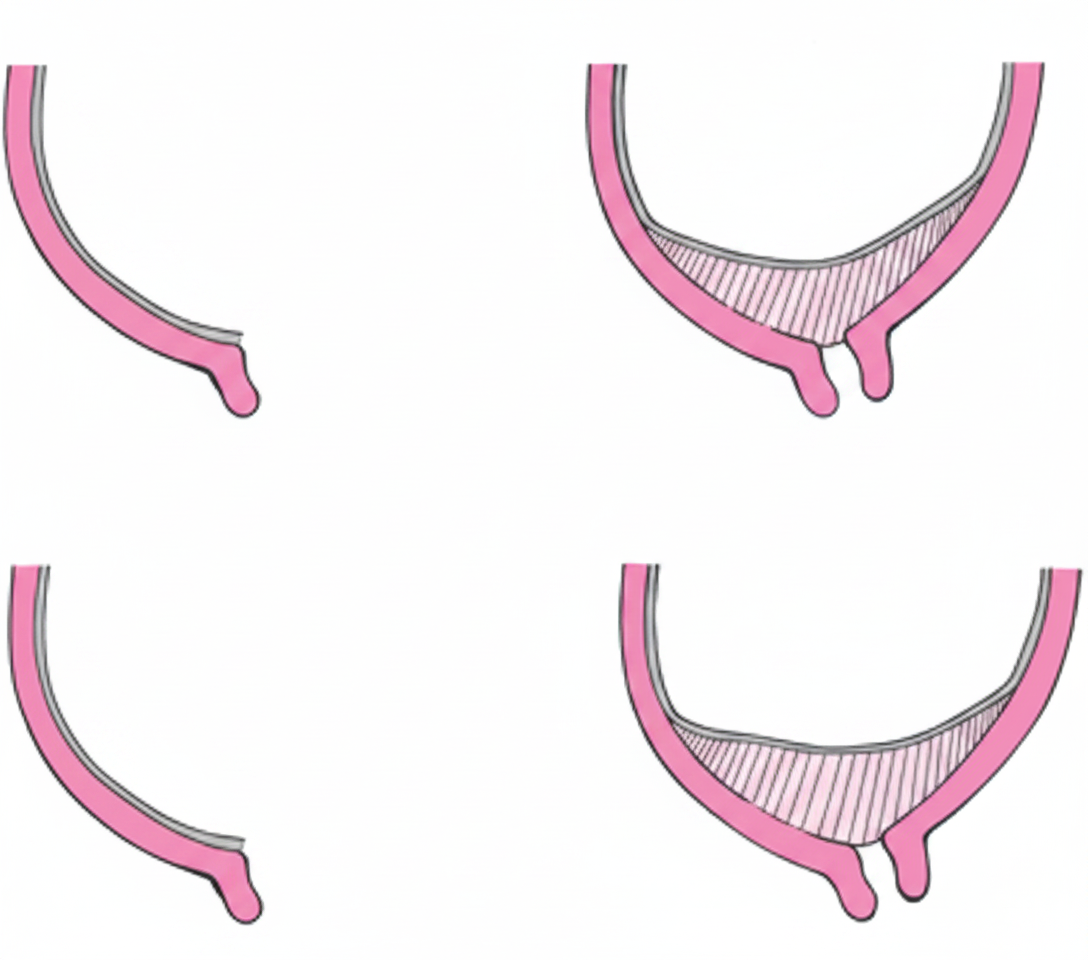
Q159
The image shows: