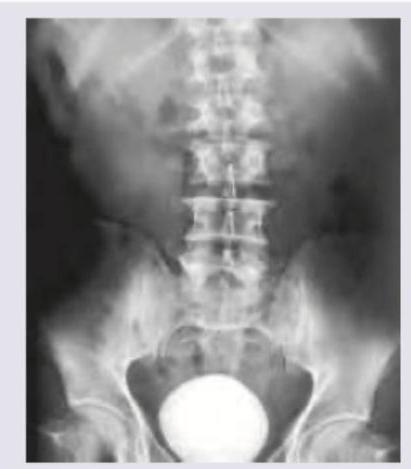
Hernia that is depicted in the image usually occurs at:
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
Hernia that is depicted in the image usually occurs at:

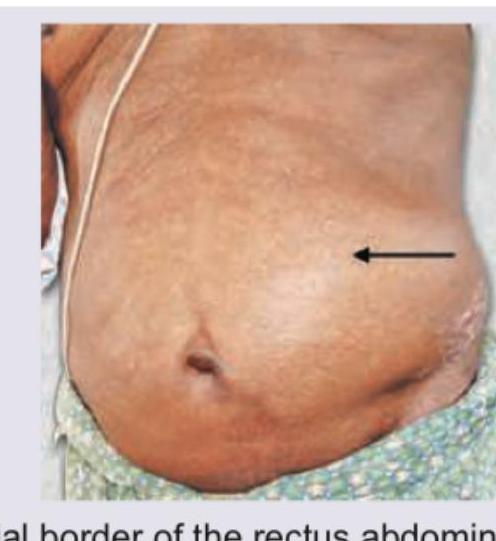
All of the following statements regarding this picture are true except:
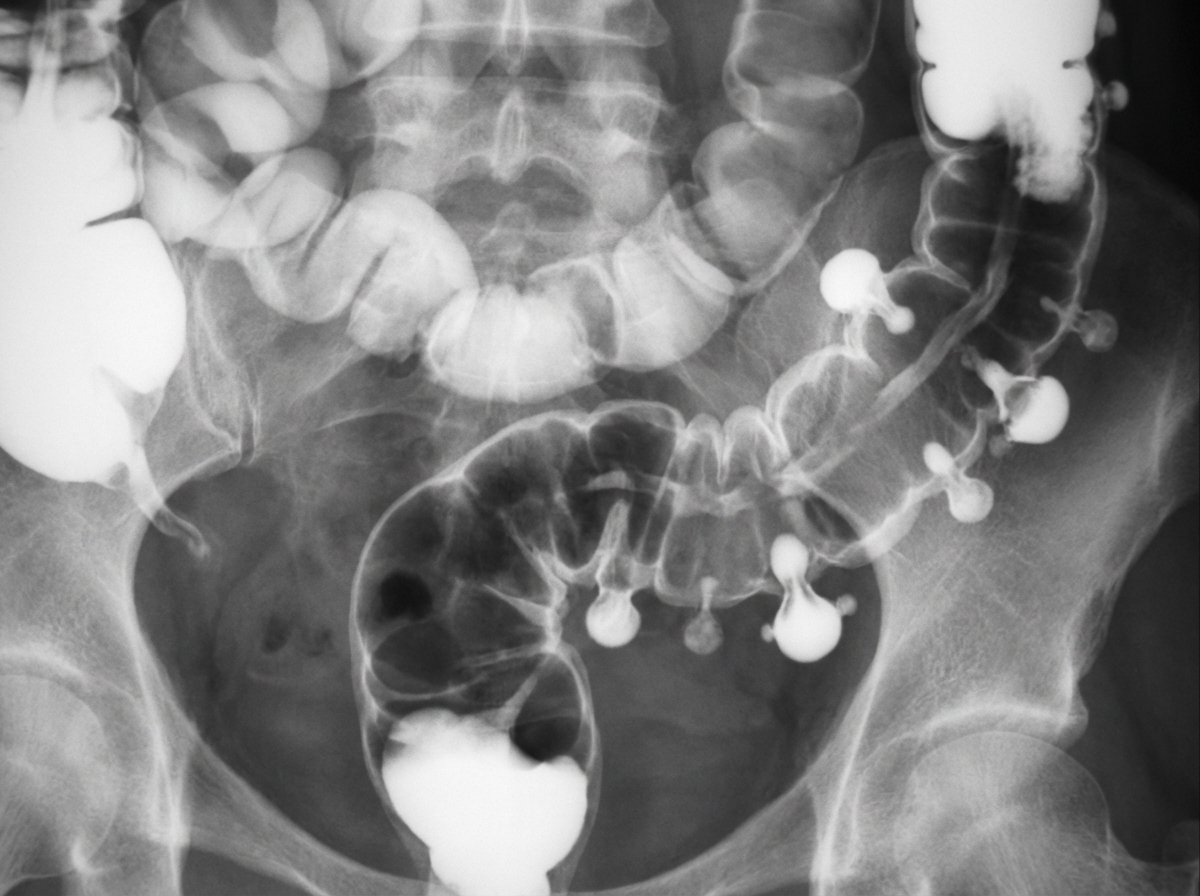
A 32-year-old woman with a history of multiple hamartomas scattered throughout the small intestine presents to a physician for follow-up. All are true about her diagnosis except?
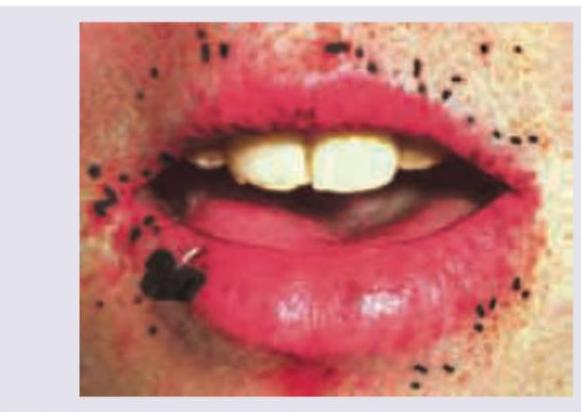
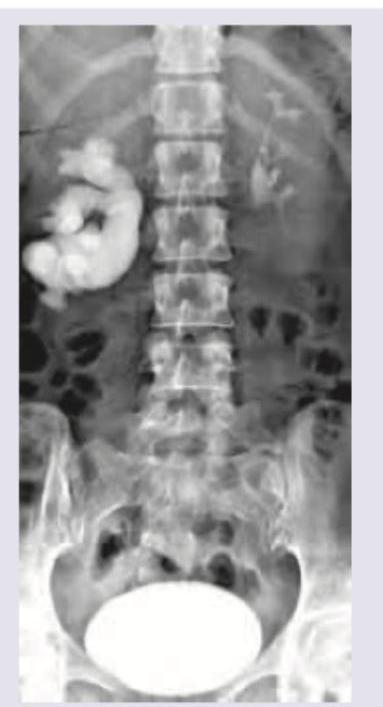
The given IVU shows:
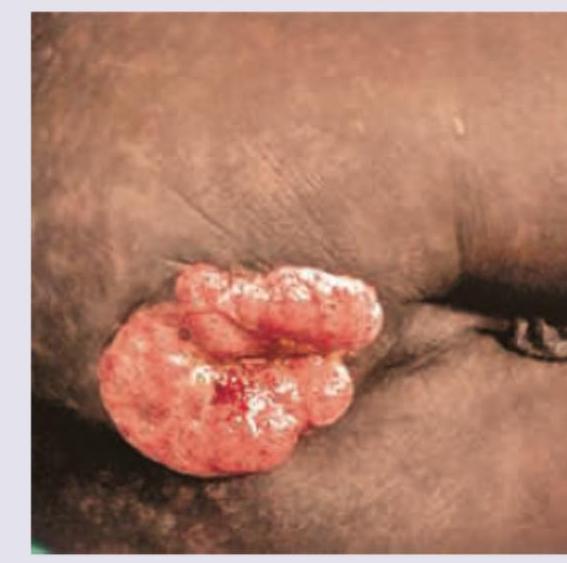
What is the preferred treatment for the shown lesion?
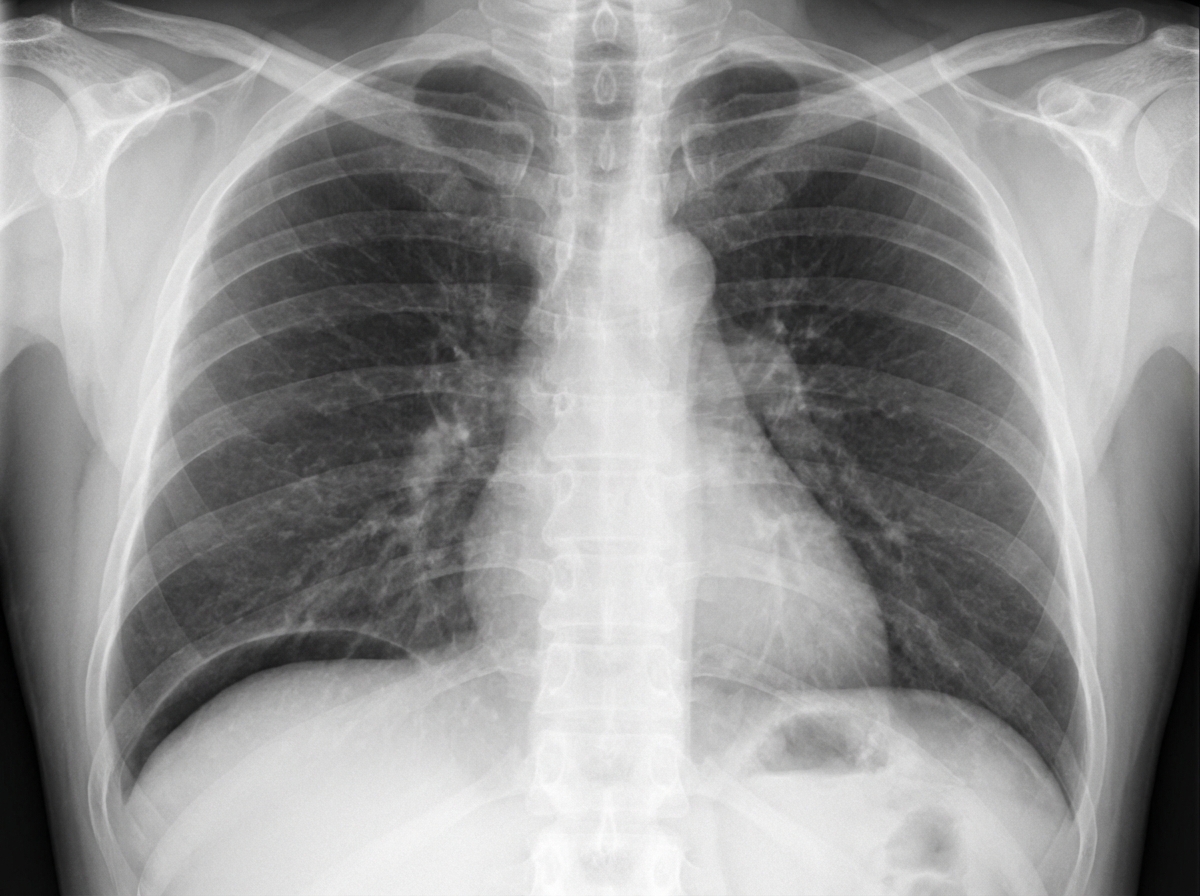
A 34-year-old male patient complains of sudden severe epigastric pain along with vomiting, tenderness, guarding. On examination there is abdominal rigidity and tachycardia. He admits to taking NSAIDs for pain. The radiological examination of the patient is given below. All statements given below are true except?
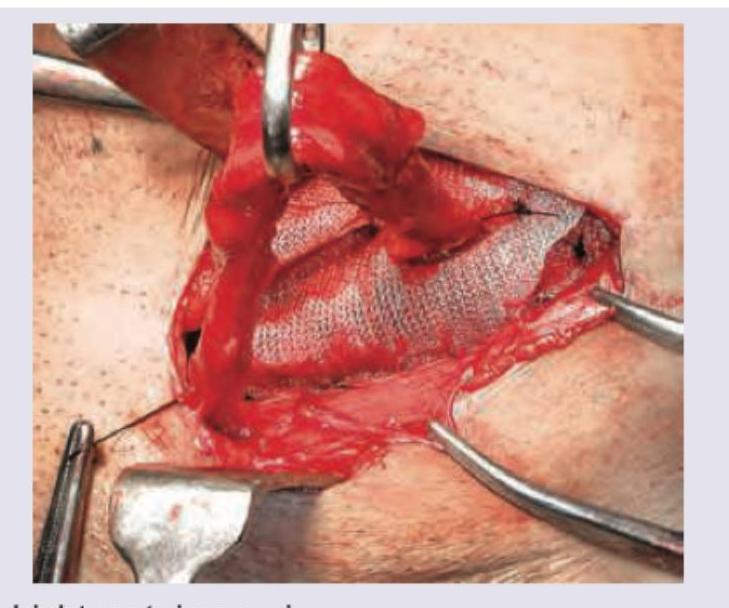
Which hernia repair procedure is shown in the image? (Recent NEET Pattern 2016-17)
A multiparous female presents with the condition shown in the image. This condition can be managed by: (Recent NEET Pattern 2016-17)
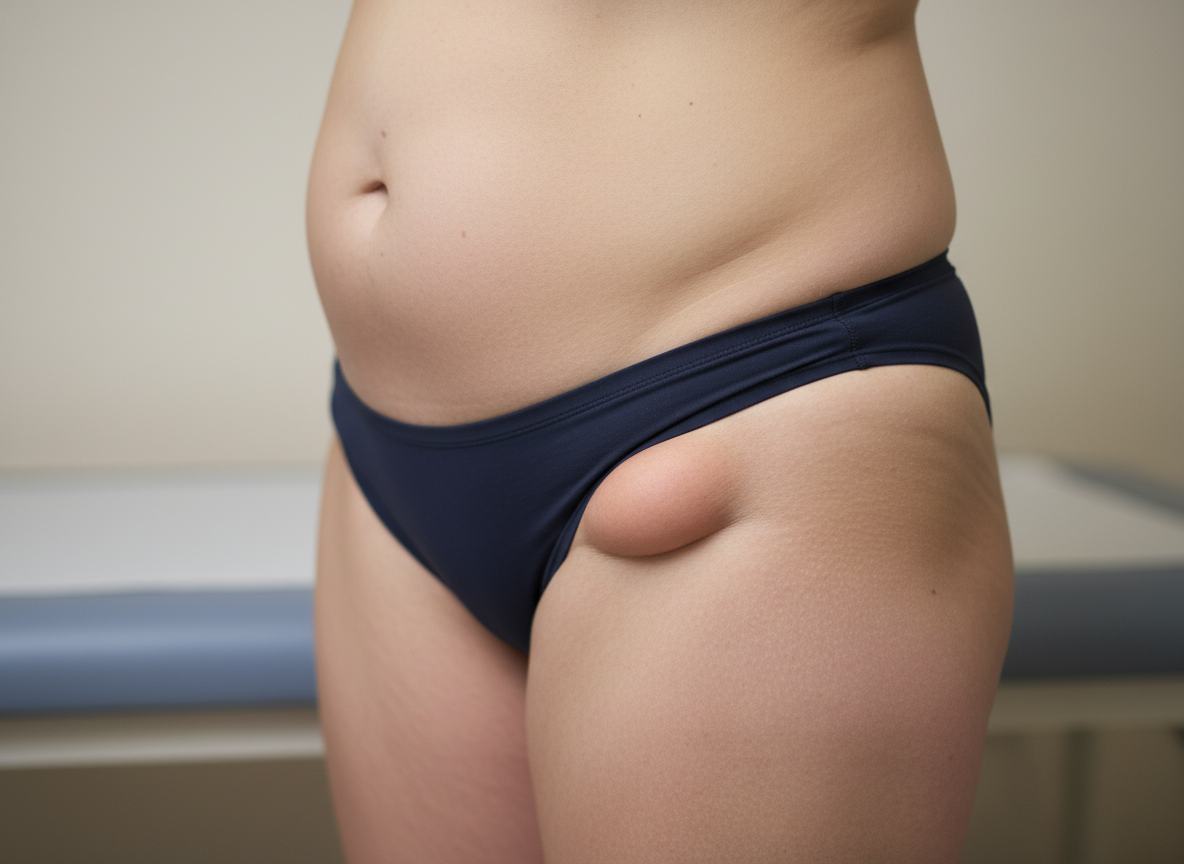
All of the following conditions are visible in the image except: (Recent NEET Pattern 2016-17)
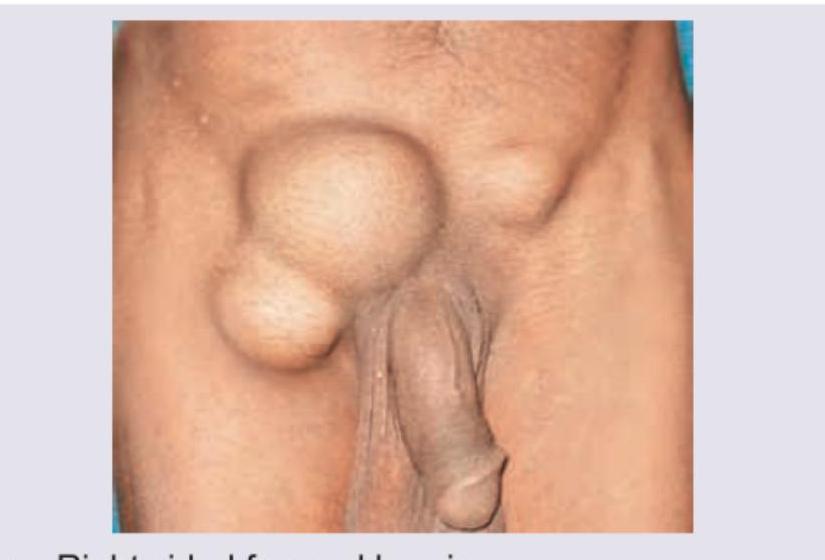
All are true about the conditions shown in the figure except?