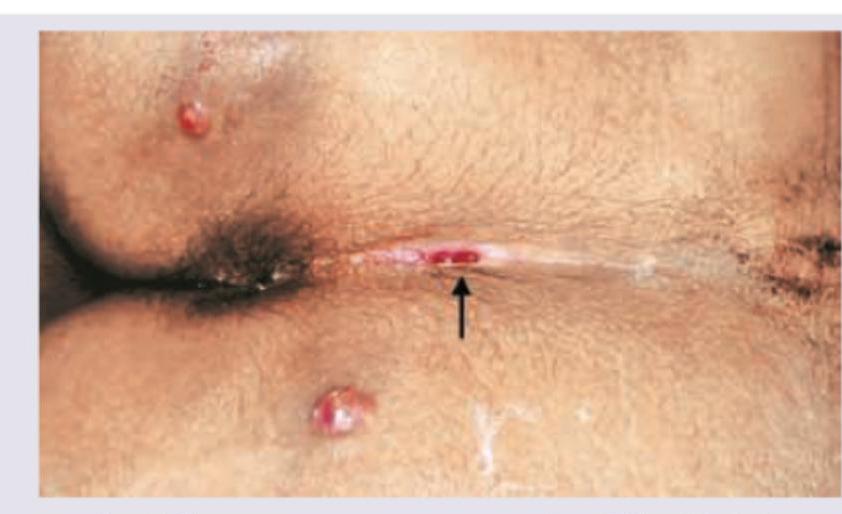
A 30-year-old AIDS patient presents with complaints as shown below. All are true about the condition except?
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
A 30-year-old AIDS patient presents with complaints as shown below. All are true about the condition except?

A patient presents with abdominal pain, diarrhea and weight loss. He gives past history of pulmonary TB. Barium film of the patient indicates which of the following condition?
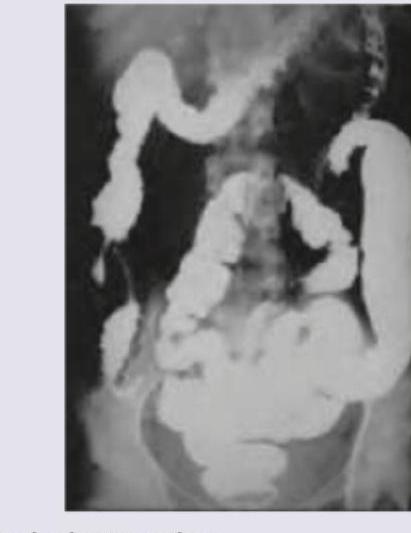
Which of the following is true regarding this condition?
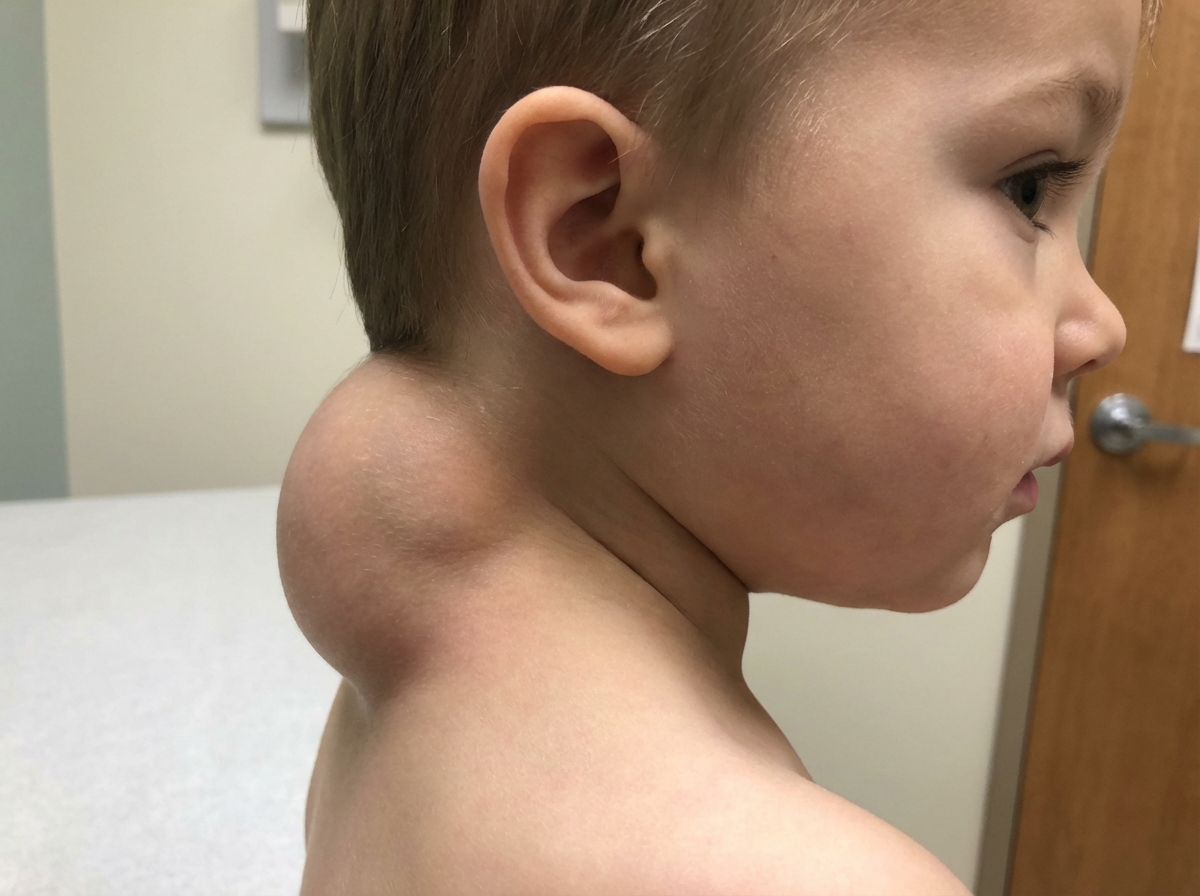
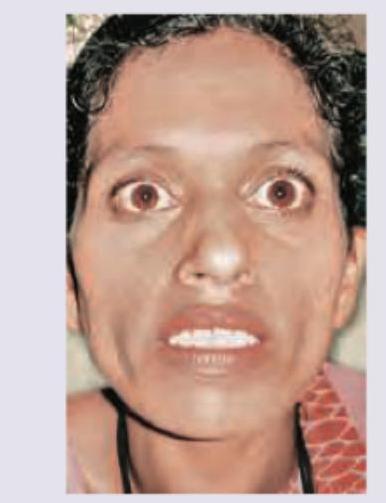
A 51-year-old woman presents with complaints of nervousness and weight loss. She reveals that she has been feeling her heart racing often. On examination, she has a fine tremor, and a large mass in the front of her neck that moves when she swallows. What is the definite treatment of choice for this condition?
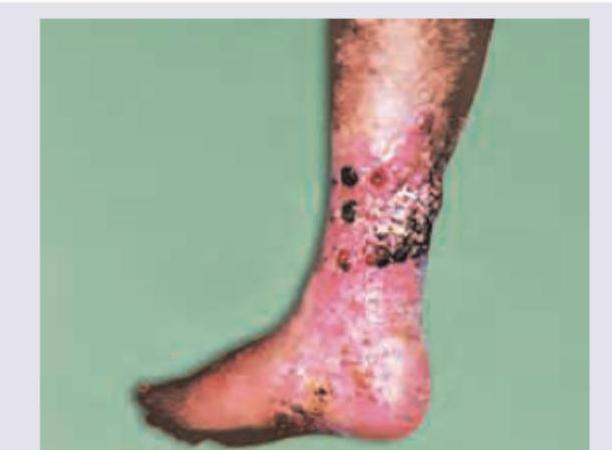
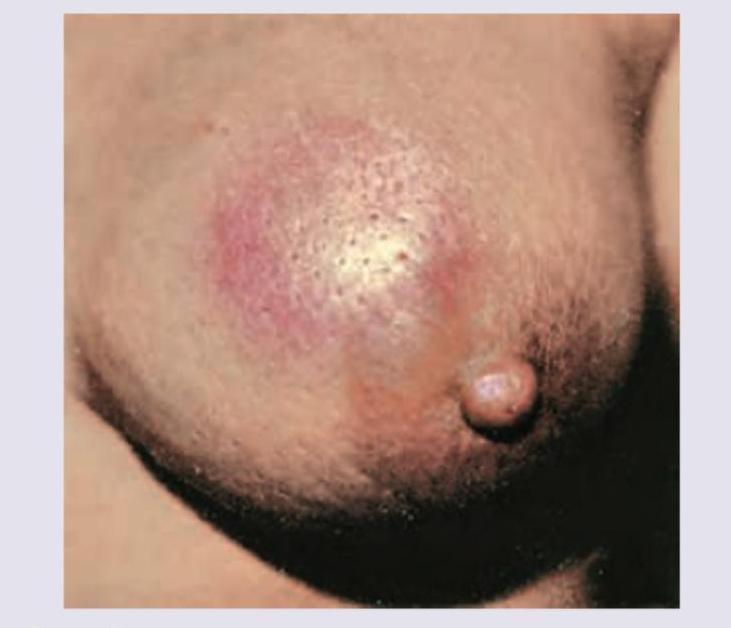
All are true about the condition shown in the image except:
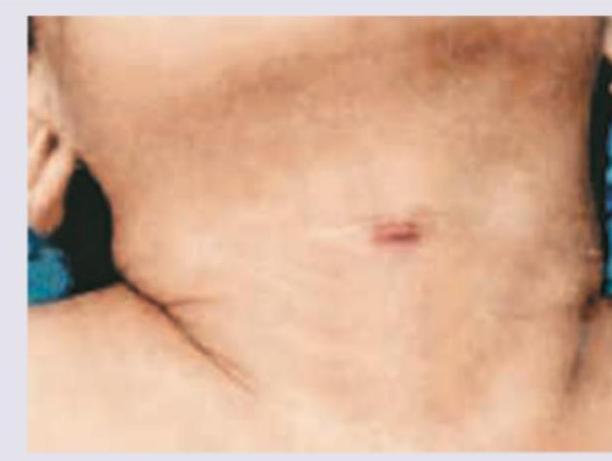
A 22-year-old female patient complains of discharge from the neck along with a previous history of midline neck swelling. Image of the patient is given below. All the statements regarding this patient are true except:
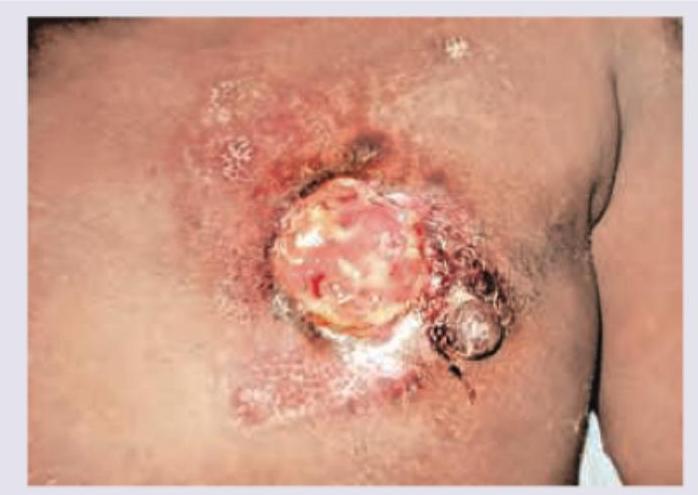
All of the following are true regarding this picture except: (Recent NEET Pattern 2016-17)
A splenorenal shunt procedure may be required for treatment of:
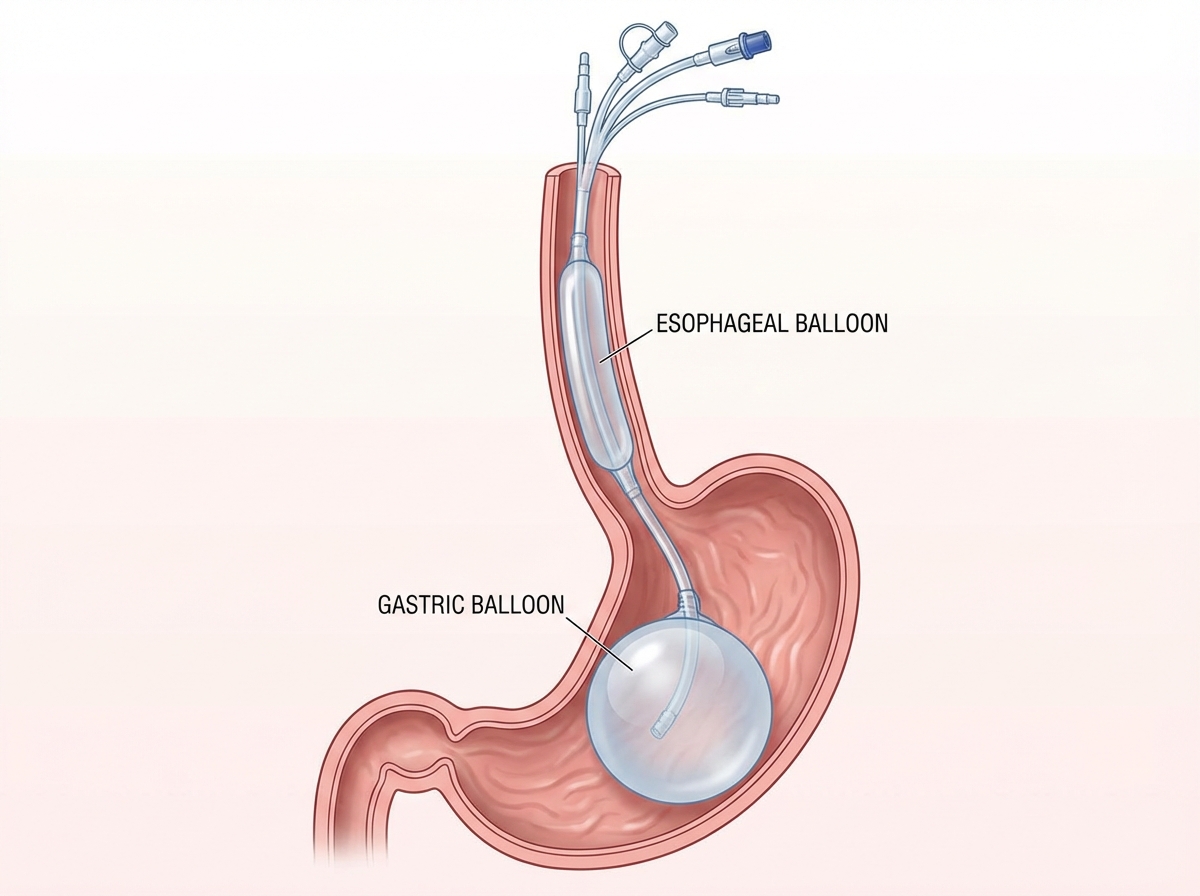
A 12-year-old patient with esophageal varices is managed by the procedure shown in the image. All of the following statements regarding this condition are true except:
A 29-year-old male who is a doctor by profession, gives a history of prolonged sitting in his OPD hours and presents with discharge and pain. Clinical presentation of the patient is given in the image. What is the most likely diagnosis?