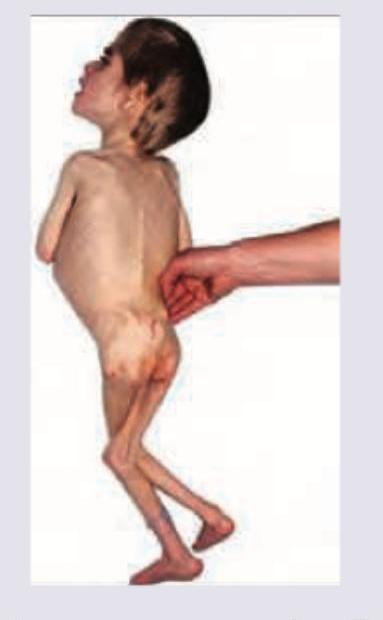
Comment on the diagnosis in the patient shown below?
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
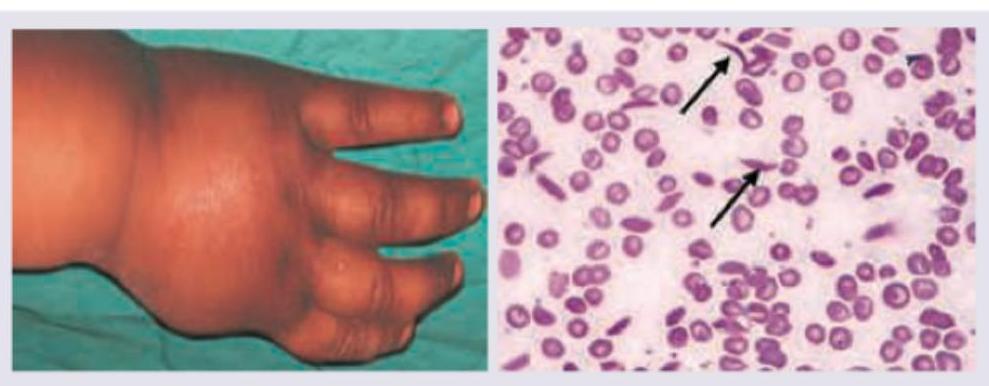
Comment on the diagnosis in the patient shown below?

The child is having skeletal abnormality in arms and hands. Which possible heart disease is seen in this condition?
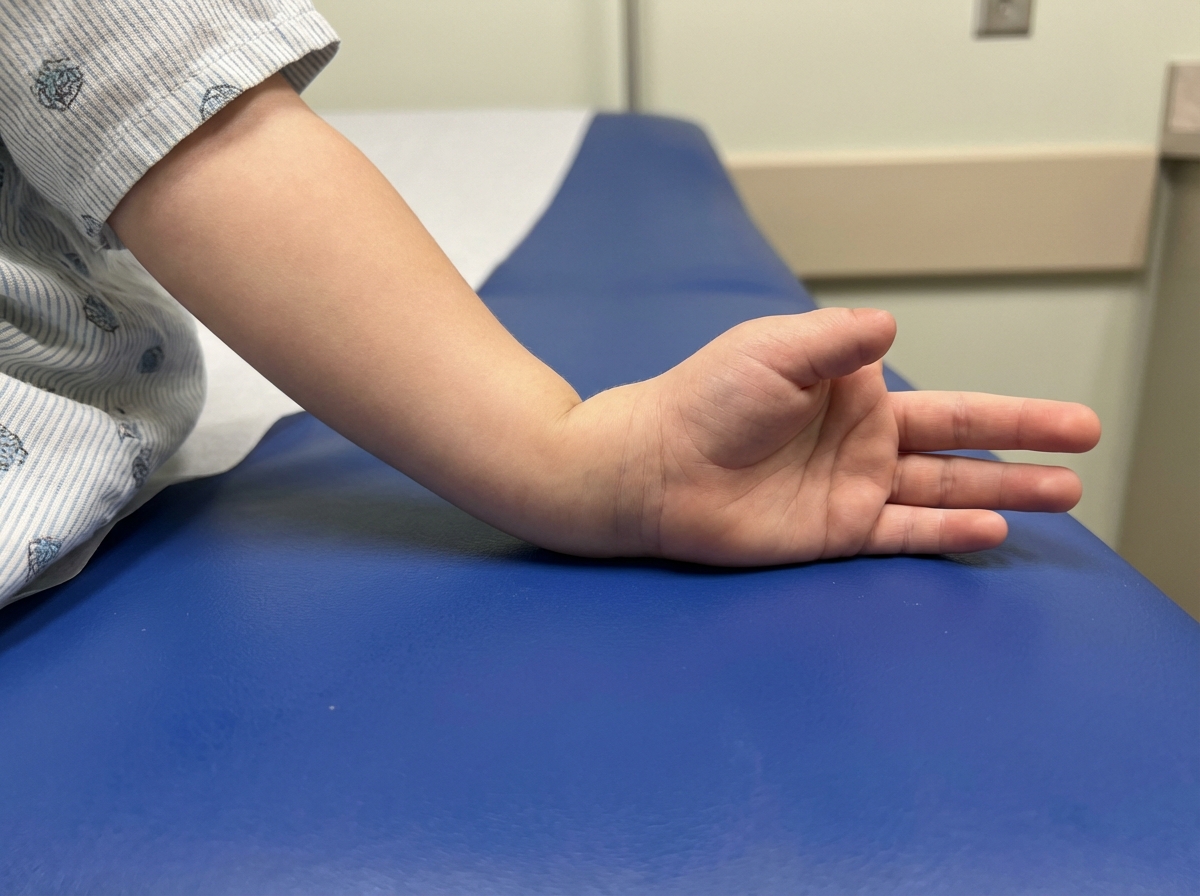
A pregnant woman undergoes a routine antenatal ultrasound scan in the second trimester. The sonologist notes an abnormal appearance of the fetal skull. What is the sign demonstrated in the given antenatal USG image?
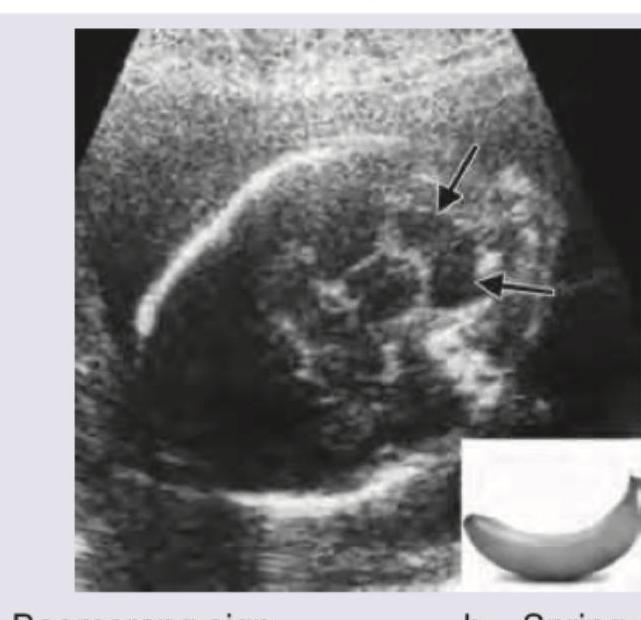
A 3-year-old child presents with sudden onset generalized petechiae and bruise on forehead. Sternal tenderness is absent and liver and spleen are not palpable. Bone marrow aspiration is normal. Probable cause is? (Recent NEET Pattern 2016-17)
A 6-month-old child brought by parents for diffuse ecchymosis on extremities and trunk. Probable diagnosis is? (Recent NEET Pattern 2016-17)
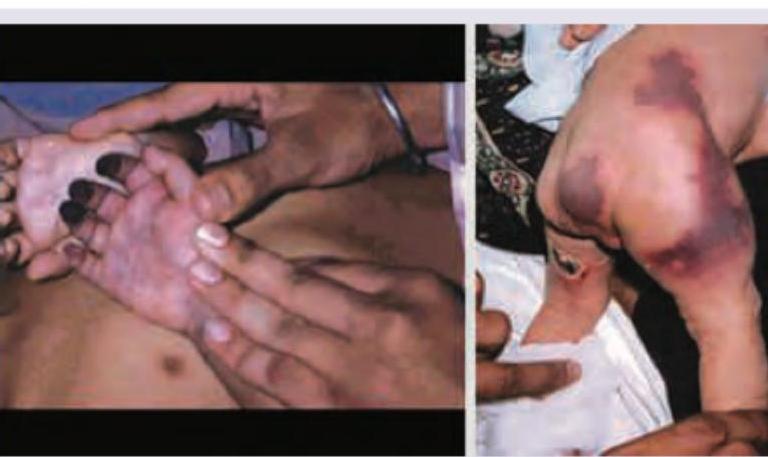
A 3-year-old child presents with bleeding from nose and Periorbital Ecchymosis. Sternal tenderness and bone pain is present. Peripheral smear shows presence of fragmented RBC and helmet cells. The most probable diagnosis is? (Recent NEET Pattern 2016-17)
A 2-year-old child presents with growth retardation, pallor, bruising and has palpable spleen 5 cm below left costal margin. Bone marrow examination is shown below. Which is incorrect about the clinical diagnosis? (Recent NEET Pattern 2016-17)
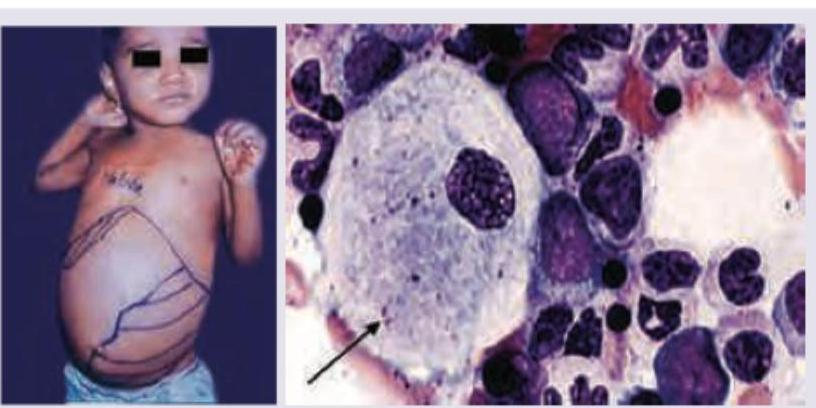
A 6-month-old infant with a progressively increasing abdominal lump. Investigations revealed a stage IVs neuroblastoma. All are correct about the condition except:
A 3-year-old girl brought with swelling in left eye which had shown rapid growth in last 4 weeks. On examination it is a bulbous fleshy mass about 5 x 4 cm arising from lower eyelid. No organomegaly or was noted and lymph node examination was unremarkable. The Complete blood counts are normal. Probable diagnosis is?
All are true about the child shown in the image except: