INI-CET 2023 — Surgery
11 Previous Year Questions with Answers & Explanations
A 30-year-old male undergoes varicocele surgery to correct his left-sided varicocele. Following the procedure, the surgeon explains the postoperative changes to the patient. The patient asks, "Through which route does the venous drainage primarily occur after the surgery?" Which of the following is the correct response by the surgeon?
A patient presents with dull aching pain and tortuous veins in both lower limbs. Which test would be appropriate for evaluating saphenofemoral junction (SFJ) incompetence?
Which of the following is not a known complication associated with the procedure done in the patient?
A 53-year-old patient presents with per rectal bleeding. Which is the most appropriate investigation to evaluate for colorectal pathology?
A 45-year-old woman with early-stage breast cancer is discussing treatment options with her surgeon. Which of the following statements regarding breast conservation surgery is NOT true?
What is the most likely diagnosis for the swelling in the floor of the mouth shown in the image?
After laparoscopic cholecystectomy what should be the urine output of the patient if the renal function of the patient is normal?
What is the baseline platelet count required for surgery?
A surgeon examined a case of hernia and was able to retract the hernial sac on examination but not the contents. Identify the type of hernia depicted in the image.

What should be done as an immediate measure for ongoing bleeding in a patient with pelvic bone fracture?
INI-CET 2023 - Surgery INI-CET Practice Questions and MCQs
Question 1: A 30-year-old male undergoes varicocele surgery to correct his left-sided varicocele. Following the procedure, the surgeon explains the postoperative changes to the patient. The patient asks, "Through which route does the venous drainage primarily occur after the surgery?" Which of the following is the correct response by the surgeon?
- A. Cremasteric and deferential veins (Correct Answer)
- B. Penile veins
- C. Ectopic drainage in the iliac fossa
- D. At the usual location
Explanation: ***Cremasteric and deferential veins*** - After varicocele surgery, the **internal spermatic veins** (pampiniform plexus) are ligated or embolized, eliminating the primary drainage route. - Venous drainage then shifts to **collateral pathways**: the **cremasteric veins** (which drain to the inferior epigastric vein) and the **deferential/vasal veins** (which drain to the vesical venous plexus). - These provide adequate alternative venous outflow from the testis, preventing venous congestion post-operatively. - This is a well-established anatomical principle in varicocele surgery. *Penile veins* - Penile veins primarily drain the **penis** itself (corpus cavernosum and spongiosum), not the testis. - They are anatomically distinct from the testicular venous drainage system and do not serve as a collateral route after varicocele repair. *Ectopic drainage in the iliac fossa* - This is not a recognized anatomical pathway for testicular venous drainage. - While cremasteric veins eventually drain to the external iliac system via inferior epigastric veins, referring to this as "ectopic drainage in the iliac fossa" is anatomically imprecise and not standard terminology. *At the usual location* - The usual pre-operative drainage is through the **pampiniform plexus → internal spermatic vein** (left side drains to left renal vein, right side to IVC). - This is the pathway that is **surgically interrupted** during varicocele repair (ligation or embolization). - Post-operatively, drainage cannot occur at this location as these vessels are deliberately occluded.
Question 2: A patient presents with dull aching pain and tortuous veins in both lower limbs. Which test would be appropriate for evaluating saphenofemoral junction (SFJ) incompetence?
- A. Fegan's test
- B. Brodie Trendelenburg test (Correct Answer)
- C. Modified Perthes test
- D. Morrissey test
Explanation: ***Brodie Trendelenburg test*** - This test evaluates **venous valve competence** at the saphenofemoral junction (SFJ) by observing the rate of venous refilling after emptying the superficial veins in the supine position and then standing. - Quick refilling of veins upon standing, particularly after compression of the SFJ, suggests **SFJ incompetence**. *Fegan's test* - This test is used to locate **incompetent perforating veins** by palpating for defects in the fascia after emptying the veins and applying compression. - It does not directly assess the competence of the saphenofemoral junction. *Modified Perthes test* - The Perthes test assesses the **patency of deep veins** and the competence of perforating veins by observing the disappearance of superficial veins during exercise with a tourniquet applied. - It primarily differentiates between superficial and deep venous insufficiency, not specifically SFJ incompetence. *Morrissey test* - This test (also known as the percussion test) involves percussing an incompetent vein distally and palpating proximally to detect a transmitted thrill, indicating **venous incompetence**. - While it helps identify reflux, it is less specific for SFJ incompetence compared to the Brodie Trendelenburg test.
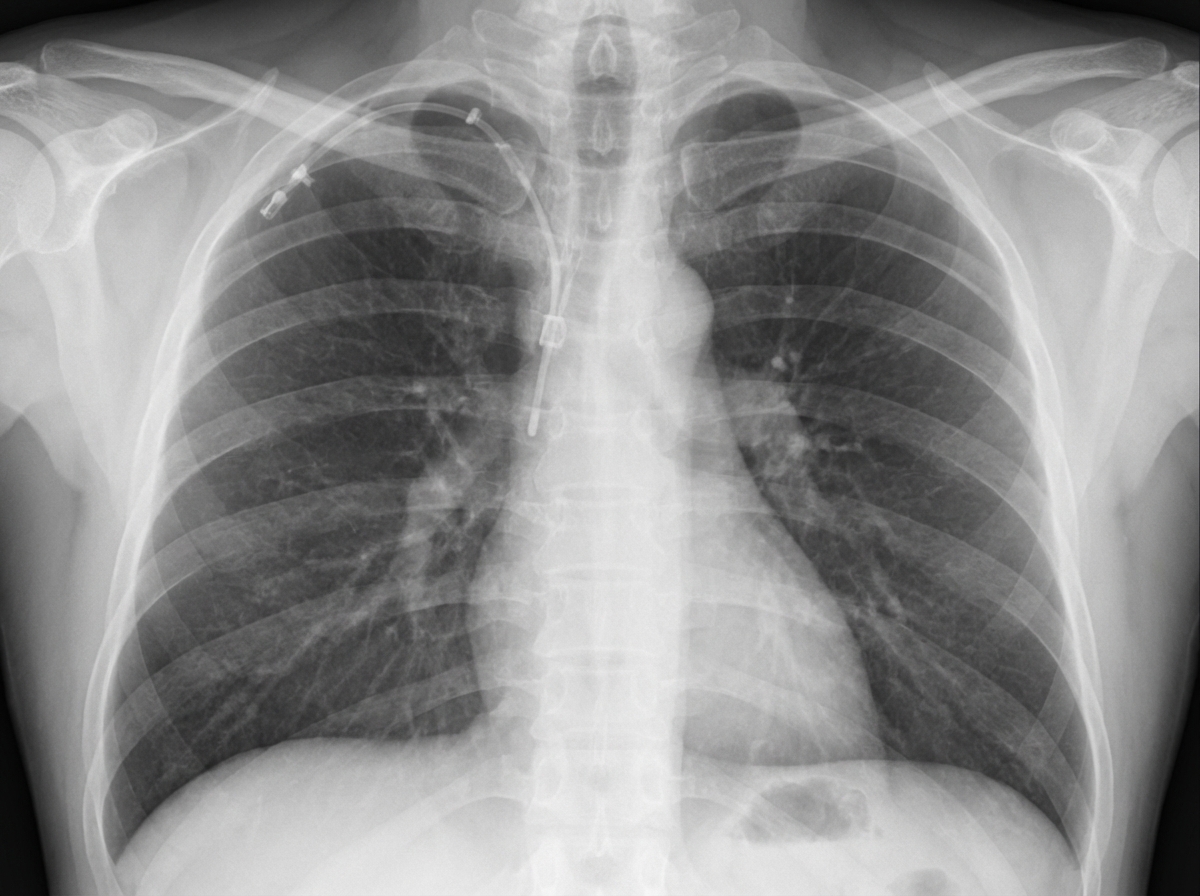
Question 3: Which of the following is not a known complication associated with the procedure done in the patient?
- A. Aspiration
- B. Pneumothorax
- C. Refeeding (Correct Answer)
- D. Arrhythmia
Explanation: ***Refeeding*** - The image shows a **central venous catheter (CVC)**, likely in the internal jugular vein. While CVCs are used for administering nutrition such as **total parenteral nutrition (TPN)**, refeeding syndrome is a metabolic complication that occurs when nutrition is reintroduced too quickly in severely malnourished patients. - **Refeeding syndrome is NOT a direct complication of the CVC insertion procedure itself**—it is a systemic metabolic complication related to the nutritional intervention (characterized by severe shifts in fluids and electrolytes, particularly hypophosphatemia, hypokalemia, and hypomagnesemia). - Therefore, refeeding is **not associated with the procedure** of CVC insertion. *Pneumothorax* - **Pneumothorax** is a well-recognized mechanical complication of central venous catheterization, particularly with subclavian and internal jugular vein approaches. - Occurs due to accidental puncture of the **pleura** during needle insertion, allowing air to enter the pleural space and causing lung collapse. - Incidence ranges from 1-6% depending on the site and operator experience. *Arrhythmia* - **Cardiac arrhythmias** are a known complication during CVC insertion when the guidewire or catheter tip inadvertently advances too far into the heart chambers (right atrium or ventricle). - Mechanical irritation of the myocardium can trigger **premature ventricular contractions (PVCs)** or other arrhythmias. - Usually transient and resolve upon withdrawing the catheter to proper position. *Aspiration* - While **aspiration** can occur in critically ill patients who require CVCs (due to altered consciousness, dysphagia, or ventilator-associated issues), it is **not a direct mechanical complication of the CVC insertion procedure itself**. - Aspiration relates to patient condition rather than the catheter placement technique, though both may coexist in the same clinical scenario.
Question 4: A 53-year-old patient presents with per rectal bleeding. Which is the most appropriate investigation to evaluate for colorectal pathology?
- A. CECT (Contrast-enhanced CT scan)
- B. CA-19-9 levels
- C. Colonoscopy (Correct Answer)
- D. CEA levels
Explanation: ***Colonoscopy*** - **Gold standard investigation** for per rectal bleeding and suspected colorectal pathology - Allows **direct visualization** of the entire colon and rectum - Enables **biopsy** of any suspicious lesions for histopathological diagnosis - Can identify various causes: **polyps, diverticula, inflammatory bowel disease, and colorectal cancer** - Therapeutic potential for polypectomy during the same procedure *CECT (Contrast-enhanced CT scan)* - Can detect large masses and assess for metastasis but not the primary diagnostic tool - Does not allow direct visualization of the mucosa or biopsy capability - Not suitable for identifying subtle mucosal lesions or early pathology - May be used as an adjunct for staging after diagnosis *CA-19-9 levels* - Tumor marker primarily associated with **pancreatic cancer** - Not routinely used for diagnosis or screening of colorectal malignancies - Lacks sensitivity and specificity for colorectal pathology - Not appropriate as initial investigation for per rectal bleeding *CEA levels (Carcinoembryonic antigen)* - Tumor marker that can be elevated in colorectal cancer - Primarily used for **monitoring treatment response** and **detecting recurrence** - Not sensitive or specific enough for initial diagnosis - Cannot replace endoscopic evaluation for per rectal bleeding
Question 5: A 45-year-old woman with early-stage breast cancer is discussing treatment options with her surgeon. Which of the following statements regarding breast conservation surgery is NOT true?
- A. Post-operative radiotherapy
- B. Axillary dissection (Correct Answer)
- C. Wide local excision
- D. Sentinel lymph node biopsy
Explanation: ***Axillary dissection*** - **Axillary dissection is NOT a routine component of breast conservation surgery** for early-stage breast cancer. - In early-stage disease, **sentinel lymph node biopsy (SLNB)** has largely replaced routine axillary dissection as it provides accurate staging with significantly less morbidity. - Axillary dissection is only performed when there is **proven extensive lymph node involvement** or when SLNB shows metastatic disease requiring further assessment. - Therefore, this statement is **NOT true** regarding routine breast conservation surgery. *Wide local excision* - **Wide local excision (lumpectomy)** is the primary surgical component of breast conservation therapy. - It involves removing the cancerous tumor along with a margin of healthy breast tissue to achieve clear margins while preserving the breast. *Sentinel lymph node biopsy* - **SLNB** is a standard procedure performed with breast conservation surgery to assess for regional lymph node metastasis. - It identifies and removes the first few lymph nodes draining the tumor, allowing accurate staging with minimal morbidity. *Post-operative radiotherapy* - **Post-operative radiotherapy** to the preserved breast is a critical and essential component of breast conservation therapy. - It significantly reduces the risk of local recurrence by treating any microscopic tumor cells that may remain after surgery.
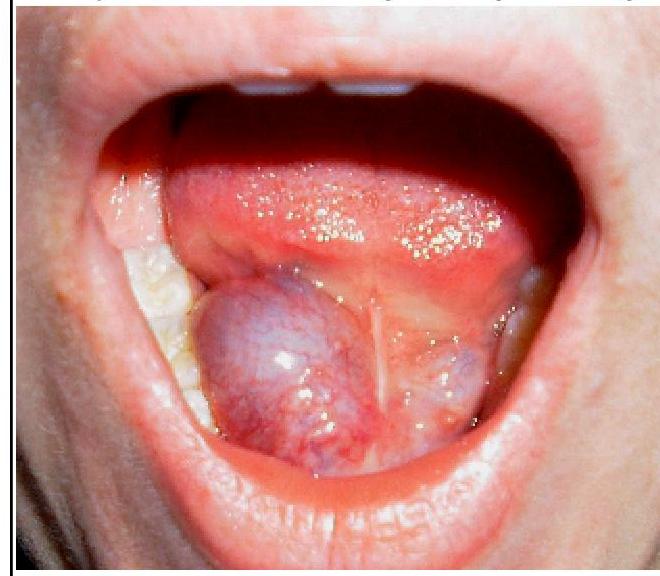
Question 6: What is the most likely diagnosis for the swelling in the floor of the mouth shown in the image?
- A. Dermoid
- B. Ranula (Correct Answer)
- C. Branchial cyst
- D. Cystic hygroma
Explanation: ***Ranula*** - The image shows a **translucent, bluish, dome-shaped swelling** in the **floor of the mouth**, consistent with a ranula. - A ranula is a **mucus extravasation cyst** caused by trauma or obstruction of the **sublingual salivary gland** duct, leading to mucus accumulation. *Dermoid* - A **dermoid cyst** in the floor of the mouth typically presents as a **firm, doughy, non-translucent swelling**, often located in the midline. - Unlike a ranula, dermoid cysts are usually **not bluish** and contain **ectodermal elements** like hair and sebaceous material. *Branchial cyst* - **Branchial cysts** are congenital abnormalities typically found in the **lateral neck**, anterior to the sternocleidomastoid muscle. - They are generally **not found in the floor of the mouth** and arise from remnants of the branchial arches. *Cystic hygroma* - A **cystic hygroma** is a **lymphatic malformation**, commonly appearing as a soft, compressible, transilluminable mass, predominantly in the **neck** and axilla. - While it can be large and cystic, its typical location and presentation are **different from a floor of mouth swelling** like a ranula.
Question 7: After laparoscopic cholecystectomy what should be the urine output of the patient if the renal function of the patient is normal?
- A. 0.5 ml/min
- B. 0.1 CC/hr
- C. 1 ml/kg/hr
- D. 0.5-1 ml/kg/hr (Correct Answer)
Explanation: ***0.5-1 ml/kg/hr*** - The standard acceptable urine output for a postoperative patient with normal renal function is **0.5-1 ml/kg/hr** (some sources extend this to 0.5-1.5 ml/kg/hr). - A minimum of **0.5 ml/kg/hr** is considered adequate renal perfusion and function, while outputs up to 1-1.5 ml/kg/hr indicate excellent hydration and renal function. - This weight-adjusted measure is the gold standard for assessing postoperative urine output and renal function. *0.5 ml/min* - This is an absolute rate (not weight-adjusted) and is inadequate as a general measure. - For a 70 kg patient, this would be only 0.43 ml/kg/hr, which is below the minimum acceptable threshold. *0.1 CC/hr* - This rate is **severely low** and indicates **oliguria** or **anuria**. - This suggests **acute kidney injury**, severe dehydration, or inadequate renal perfusion requiring immediate intervention. *1 ml/kg/hr* - While this value falls within the acceptable range, it represents only a single point rather than the **standard range of 0.5-1 ml/kg/hr**. - The range option is more comprehensive and represents the full spectrum of normal postoperative urine output.
Question 8: What is the baseline platelet count required for surgery?
- A. 50,000/µL (50 × 10^9/L) (Correct Answer)
- B. 40,000/µL (40 × 10^9/L)
- C. 20,000/µL (20 × 10^9/L)
- D. 30,000/µL (30 × 10^9/L)
Explanation: ***50,000/µL (50 × 10^9/L)*** - A platelet count of **50,000/µL** is considered the **minimum threshold** for safe surgical procedures. - This level is generally sufficient to achieve **adequate primary hemostasis** and minimize the risk of significant perioperative bleeding. *20,000/µL (20 × 10^9/L)* - A platelet count of **20,000/µL** is generally **too low** for most surgical interventions, as it significantly increases the risk of serious bleeding. - This level is often associated with a risk of **spontaneous bleeding**, particularly in mucous membranes. *40,000/µL (40 × 10^9/L)* - While closer to the safe threshold, a platelet count of **40,000/µL** might still be considered **suboptimal** for major surgeries, especially those with a high risk of blood loss. - Some surgeons and anesthesiologists may prefer a slightly higher count to ensure a wider **safety margin**. *30,000/µL (30 × 10^9/L)* - A platelet count of **30,000/µL** is generally **insufficient** for most surgical procedures and would likely necessitate **platelet transfusion** preoperatively. - Patients at this level are at an **increased risk of bleeding** during and after surgery.
Question 9: A surgeon examined a case of hernia and was able to retract the hernial sac on examination but not the contents. Identify the type of hernia depicted in the image.
- A. Reduction en masse (Correct Answer)
- B. Sliding hernia
- C. Incarcerated hernia
- D. Maydl's hernia
Explanation: ***Reduction en masse*** - This occurs when the **hernia sac** is reduced into the abdomen but the contents remain incarcerated within the sac, still outside the peritoneal cavity. The image clearly depicts the sac being pushed back, while the bowel loop within it remains constricted at the neck. - This is a dangerous situation because the **incarcerated bowel** is not visible externally, yet remains at risk of strangulation and is often unrecognized. *Sliding hernia* - A sliding hernia involves a portion of the **retroperitoneal organ** (like the colon or bladder) forming part of the posterior wall of the hernia sac. - This typically occurs gradually, and the sac itself is not mistakenly reduced without its contents while the contents remain trapped. *Incarcerated hernia* - An incarcerated hernia means the contents of the hernia sac are **trapped** and cannot be manually reduced back into the abdominal cavity. - While the image shows incarcerated contents, the specific problem here is that the *sac* has been reduced without its contents, which is a particular complication rather than just general incarceration. *Maydl's hernia* - Maydl's hernia (also known as a W-hernia) describes a scenario where **two loops of bowel** are contained within the hernia sac, with a connecting loop of bowel located within the abdominal cavity, forming a 'W' shape. - The illustration shows only one loop of bowel within the sac and does not suggest the specific 'W' configuration or intra-abdominal strangulation of the connecting segment.
Question 10: What should be done as an immediate measure for ongoing bleeding in a patient with pelvic bone fracture?
- A. Use Pelvic Binders (Correct Answer)
- B. Rapid blood transfusion
- C. External fixation
- D. Internal definitive fixation
Explanation: **Use Pelvic Binders** - **Pelvic binders** apply circumferential compression, which helps to stabilize the fracture and reduce the pelvic volume. - This mechanical stabilization significantly reduces ongoing hemorrhage from venous and bone surface bleeding in unstable pelvic fractures. *Rapid blood transfusion* - While critically important for managing **hemorrhagic shock**, blood transfusion alone does not address the source of ongoing bleeding. - It is a supportive measure, not an immediate means to stop the bleeding from an unstable pelvic fracture. *Internal definitive fixation* - **Internal definitive fixation** is a surgical procedure aimed at permanently stabilizing the fracture and would typically be performed after initial resuscitation and bleeding control. - It is not an immediate measure for **ongoing life-threatening hemorrhage** and carries procedural risks. *External fixation* - **External fixation** can stabilize an unstable pelvic fracture and helps in controlling bleeding, but applying a **pelvic binder** is a quicker and less invasive initial step. - External fixation is usually performed by a surgeon in a controlled environment, not as the very first immediate bedside measure to stop bleeding.