INI-CET 2023 — Pediatrics
7 Previous Year Questions with Answers & Explanations
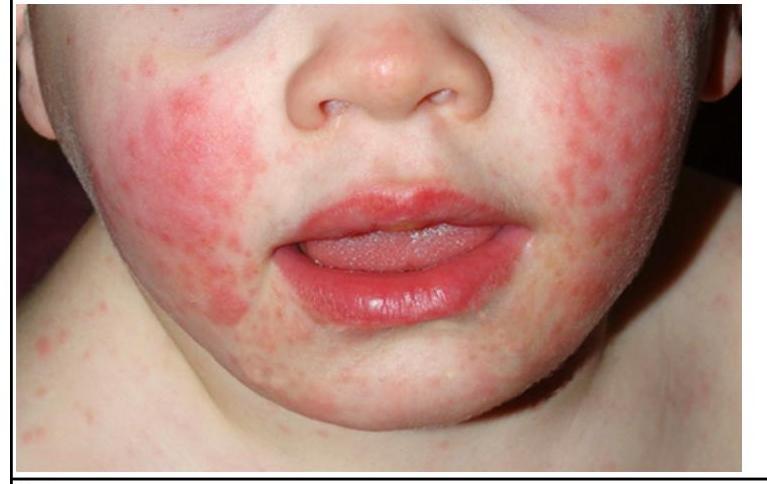
A child presenting with the following appearance is at risk of developing?
A child with fever for 6 days, strawberry tongue, conjunctival congestion with peeling of skin. What will be the treatment option for this child?
A 10-week-old baby came for vaccination. The baby had a previous history of inconsolable crying and fever (40°C) after vaccination at 6 weeks. What should be given now?
Which of the following is considered a minor clinical finding suggestive of congenital heart disease?
Which test is not required for Turner mosaic syndrome?
In which of the following disorders, vaccines are not contraindicated in the person suffering from that disease?
A 10 week old child comes for vaccination, with previous history of inconsolable cry & fever after getting vaccinated at 6 weeks. What should be done next?
INI-CET 2023 - Pediatrics INI-CET Practice Questions and MCQs
Question 1: A child presenting with the following appearance is at risk of developing?
- A. Immunodeficiency
- B. Lymphoproliferative disorder
- C. Gingivostomatitis
- D. Pure red cell aplasia (Correct Answer)
Explanation: ***Pure red cell aplasia*** - The image shows a "slapped cheek" rash, which is characteristic of **erythema infectiosum** (fifth disease) caused by **Parvovirus B19**. - Parvovirus B19 has a tropism for **erythroid progenitor cells** in the bone marrow, leading to a temporary cessation of red blood cell production, especially critical in individuals with underlying hemolytic anemias. *Immunodeficiency* - While viral infections can be more severe in immunodeficient individuals, the presented rash is specifically characteristic of **Parvovirus B19 infection**, not a general sign of immunodeficiency. - Immunodeficiency would typically involve recurrent, severe, or unusual infections, which are not directly indicated by the rash alone. *Lymphoproliferative disorder* - Lymphoproliferative disorders involve abnormal proliferation of lymphocytes and typically do not present with a "slapped cheek" rash. - Clinical signs would more likely include **lymphadenopathy**, hepatosplenomegaly, and cytopenias, not the classic facial rash seen here. *Gingivostomatitis* - **Gingivostomatitis** is an inflammation of the gums and oral mucosa, often caused by herpes simplex virus, presenting with **sores and ulcers in the mouth**. - The rash seen in the image is on the **cheeks and body**, not primarily oral, and is a classic presentation of erythema infectiosum.
Question 2: A child with fever for 6 days, strawberry tongue, conjunctival congestion with peeling of skin. What will be the treatment option for this child?
- A. Antibiotics
- B. Steroids
- C. Antipyretics
- D. IVIG (Correct Answer)
Explanation: ***IVIG*** - The constellation of **fever for 6 days (prolonged fever)**, **strawberry tongue**, **conjunctival congestion**, and **peeling skin** is highly indicative of **Kawasaki disease**. - **Intravenous immunoglobulin (IVIG) 2 g/kg as a single infusion** is the cornerstone of treatment for Kawasaki disease to reduce the risk of **coronary artery aneurysms** (from ~25% to <5%). - IVIG should be administered within **10 days of fever onset** for maximum efficacy. - **High-dose aspirin** (80-100 mg/kg/day) is given concurrently until the fever subsides, then switched to low-dose aspirin (3-5 mg/kg/day) for antiplatelet effect. *Antibiotics* - Kawasaki disease is a **vasculitis**, not a bacterial infection, so antibiotics are ineffective. - While other conditions like scarlet fever can present with strawberry tongue, the prolonged fever and other classic Kawasaki features differentiate it. *Steroids* - While steroids can reduce inflammation, they are **not the primary treatment** for Kawasaki disease and are typically used in conjunction with IVIG in **refractory cases** or for IVIG-resistant disease. - **Monotherapy with steroids** is not recommended for acute Kawasaki disease due to potential for increased aneurysm risk. *Antipyretics* - **Antipyretics** like acetaminophen can help manage the fever symptomatically. - However, they **do not treat the underlying vasculitis** or prevent the serious cardiac complications of Kawasaki disease. - Note: **NSAIDs like ibuprofen should be avoided** when high-dose aspirin is being used due to risk of drug interactions.
Question 3: A 10-week-old baby came for vaccination. The baby had a previous history of inconsolable crying and fever (40°C) after vaccination at 6 weeks. What should be given now?
- A. Don't give DPT
- B. Defer for 1 month
- C. Give DPT
- D. Give DT only (Correct Answer)
Explanation: ***Give DT only*** - The previous severe adverse reaction (**inconsolable crying** and **fever of 40°C**) is a specific contraindication to the **pertussis component** of the DPT vaccine. - According to **pediatric vaccination guidelines**, severe reactions (fever ≥40°C, inconsolable crying >3 hours) are absolute contraindications to further pertussis-containing vaccines. - The **diphtheria and tetanus toxoids** were not associated with the adverse reaction and should be safely continued. - **DT vaccine (without pertussis)** provides essential protection against diphtheria and tetanus while avoiding the problematic pertussis component. *Don't give DPT* - This option is imprecise because it doesn't specify what should be given instead. - While it correctly identifies that full DPT should be avoided, it fails to address the need for continued protection against diphtheria and tetanus. - The medically appropriate approach is to give **DT vaccine**, not to simply withhold vaccination. *Defer for 1 month* - Deferring vaccination does not address the core issue that the **pertussis component specifically** caused the severe reaction. - This approach would unnecessarily **delay protection** against diphtheria and tetanus, which the baby can safely receive immediately as DT vaccine. - The problem is not timing but the vaccine component itself. *Give DPT* - Administration of the full DPT vaccine is **absolutely contraindicated** given the history of severe adverse reactions (fever ≥40°C and inconsolable crying). - Repeating DPT risks another severe reaction and potential permanent neurological complications. - This would be a dangerous and inappropriate management decision.
Question 4: Which of the following is considered a minor clinical finding suggestive of congenital heart disease?
- A. Low BP
- B. Systolic murmur grade-3
- C. Abnormal 2nd heart sound (Correct Answer)
- D. Diastolic murmur
Explanation: ***Abnormal 2nd heart sound*** - An abnormal (loud, soft, split, or single) **second heart sound (S2)** is a minor clinical finding that can suggest congenital heart disease (CHD). - This reflects abnormalities in the **pulmonary** or **aortic valve closure**, common in various CHDs. *Low BP* - **Low blood pressure** is a general sign of circulatory compromise and is not a specific or minor clinical finding for congenital heart disease itself. - It might indicate severe heart failure or shock, which are major, late-stage complications of CHD, rather than an early suggestive sign. *Systolic murmur grade-3* - A **systolic murmur of grade 3 or higher** is generally considered a **major clinical finding** and often indicates significant structural heart disease. - Minor findings are typically less intense or specific signs that still warrant further investigation. *Diastolic murmur* - The presence of **any diastolic murmur** is considered a **major clinical finding** that is highly suggestive of significant heart disease, as it often implies structural valve abnormalities or abnormal blood flow during diastole. - This is not a "minor" finding as it virtually always indicates pathology.
Question 5: Which test is not required for Turner mosaic syndrome?
- A. Audiometry
- B. Oral glucose tolerance test
- C. Echo
- D. ANA (Correct Answer)
Explanation: ***ANA*** - **Antinuclear antibody (ANA)** testing is primarily used for diagnosing autoimmune diseases like **systemic lupus erythematosus** and is not routinely required for the management of Turner mosaic syndrome. - While autoimmune conditions can rarely co-occur, ANA is not a standard screening or diagnostic test for the common complications of Turner syndrome. *Audiometry* - **Audiometry** is recommended for Turner syndrome patients due to an increased risk of **hearing loss**, particularly **sensorineural hearing loss**. - Regular monitoring helps detect and manage hearing impairments early, which can affect development and quality of life. *Oral glucose tolerance test* - Patients with Turner syndrome have an increased risk of developing **glucose intolerance** and **type 2 diabetes mellitus**. - An **oral glucose tolerance test (OGTT)** is important for screening and early detection of these metabolic abnormalities. *Echo* - **Echocardiography** is crucial for evaluating potential **cardiovascular abnormalities**, which are common in Turner syndrome. - These can include **bicuspid aortic valve**, **coarctation of the aorta**, and other structural heart defects.
Question 6: In which of the following disorders, vaccines are not contraindicated in the person suffering from that disease?
- A. Digeorge syndrome
- B. Wiskott Aldrich syndrome
- C. Ataxia telangiectasia
- D. Complement deficiency disorders (Correct Answer)
Explanation: ***Complement deficiency disorders*** - While patients with **complement deficiencies** are susceptible to certain infections (especially by encapsulated bacteria), their adaptive immune system is generally intact. - Therefore, most vaccines, including **live attenuated vaccines**, are not contraindicated; in fact, vaccination is crucial for preventing infections in these patients. *Digeorge syndrome* - This syndrome involves **thymic hypoplasia or aplasia**, leading to severe **T-cell immunodeficiency**. - **Live attenuated vaccines** (e.g., MMR, varicella) are contraindicated due to the risk of uncontrolled replication of the vaccine strain in immunocompromised individuals. *Wiskott Aldrich syndrome* - This is an **X-linked immunodeficiency** characterized by immunodeficiency, eczema, and thrombocytopenia, involving defects in both T and B cell function, and **platelet dysfunction**. - Due to profound immune defects, particularly in T-cell function, **live attenuated vaccines** are contraindicated. *Ataxia telangiectasia* - This is an autosomal recessive disorder causing **progressive cerebellar ataxia**, telangiectasias, and severe **combined immunodeficiency (SCID)-like features** affecting both T and B cells, as well as an increased risk of malignancy. - Due to the severe immunodeficiency, **live attenuated vaccines** are contraindicated.
Question 7: A 10 week old child comes for vaccination, with previous history of inconsolable cry & fever after getting vaccinated at 6 weeks. What should be done next?
- A. Give DT (Correct Answer)
- B. Defer for 1 month
- C. Administer antibiotics
- D. Give DPT vaccination
Explanation: ***Correct Option: Give DT*** - **Inconsolable crying** (typically defined as crying ≥3 hours) following pertussis-containing vaccine is classified as a **precaution** for subsequent doses per IAP, CDC, and WHO guidelines - When a **precaution** exists, the pertussis component should be **withheld** from future doses - **DT vaccine** (diphtheria-tetanus without pertussis) ensures continued protection against diphtheria and tetanus while avoiding repeat exposure to the pertussis antigen that likely caused the reaction - This represents appropriate **risk-benefit assessment** in immunization practice *Incorrect: Give DPT vaccination* - Continuing DPT after inconsolable crying ignores established AEFI (Adverse Events Following Immunization) guidelines - While fever alone is not a contraindication, **inconsolable crying is a recognized precaution** that warrants modification of the vaccination schedule - Repeating the same vaccine risks recurrence of the adverse event *Incorrect: Defer for 1 month* - Simply deferring without changing the vaccine type doesn't address the underlying issue - The child would still receive the pertussis component later, risking another adverse reaction - Unnecessary delay in protection against diphtheria and tetanus when DT is available *Incorrect: Administer antibiotics* - **Post-vaccination fever and crying** are inflammatory responses to vaccine antigens, not bacterial infections - Antibiotics have no role in managing vaccine-related reactions - This approach doesn't address the need for continued immunization protection