All SubjectsAnatomy (9)Anesthesiology (2)Biochemistry (9)Community Medicine (4)Dermatology (7)ENT (1)Forensic Medicine (3)Internal Medicine (18)Microbiology (7)Obstetrics and Gynecology (12)Ophthalmology (4)Pathology (14)Pediatrics (7)Pharmacology (17)Physiology (11)Psychiatry (3)Radiology (3)Surgery (11)
Q11
Order of drawing blood in vacutainers should be in the following sequence to prevent contamination?
Q12
All of the following are tests done for Turner mosaic screening except?
Q13
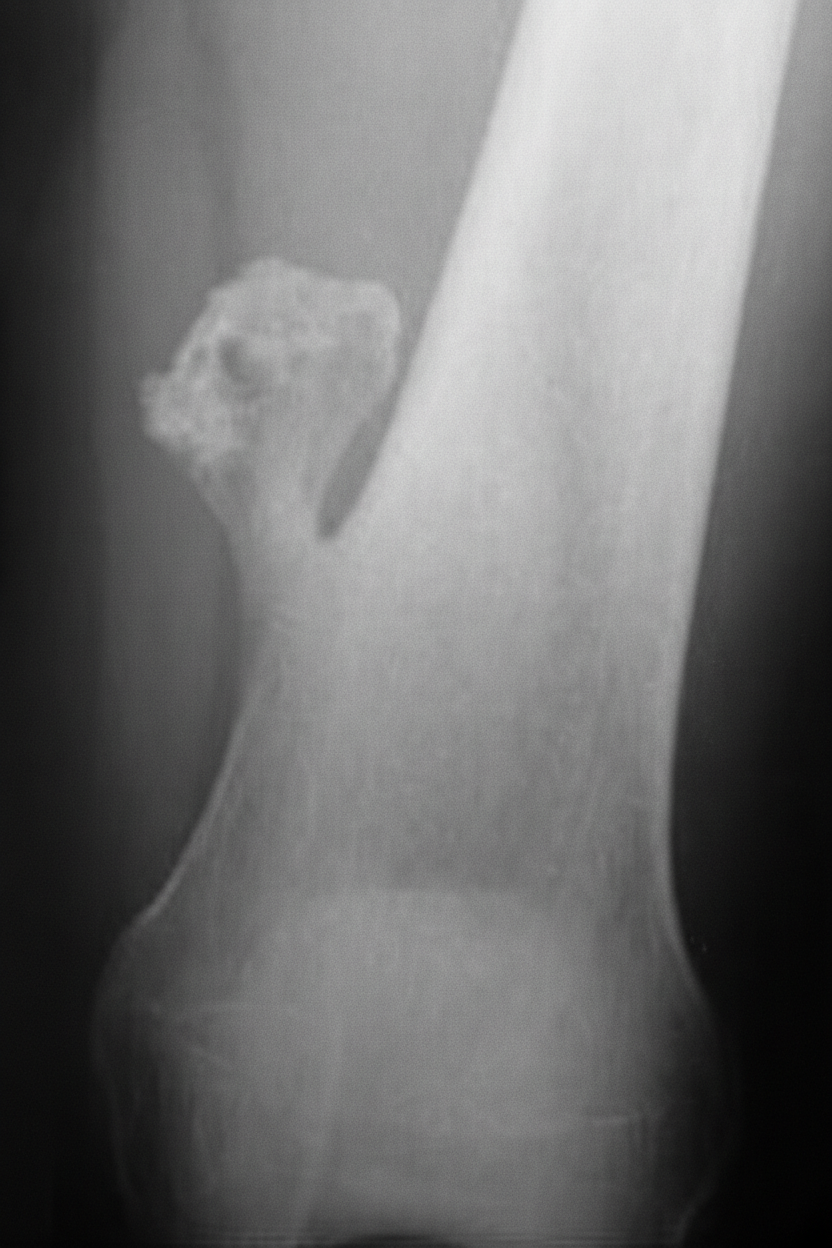
A 14 year old male presents with mushroom like tumor in the distal femur for past 2 years. Which of the following features suggest malignant transformation?
Q14
Abnormal accumulation of misfolded protein is seen in?