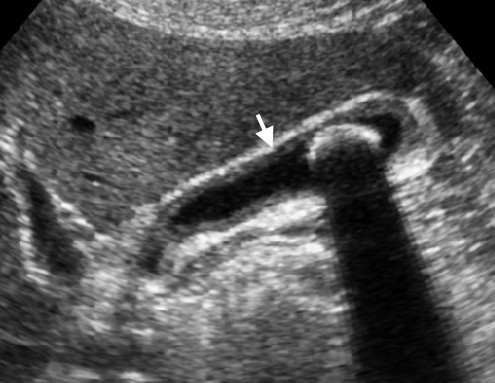
What condition is associated with the sign seen in the given USG?
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
Match the incubation periods of the following diseases: a. Syphilis b. SARS c. Hepatitis A d. Chickenpox Match with: 1. 10-21 days 2. 21 days (3 weeks) 3. 2-7 days 4. 15-50 days
Slapped cheek appearance is associated with which of the following?
Patient presented with following features: - ipsilateral loss of pain and temperature sensation in the face - Contralateral loss of pain and temperature sensation in the body - Horner's syndrome - Dysphagia and hoarseness - Ataxia and vertigo Which artery is involved in syndrome based on above clinical features?
A patient has dyspareunia, and dysmenorrhea with adnexal tenderness. What is the first step of investigation?
After delivering a baby boy, a 25 -year-old mother developed acute PPH and hypovolemic shock, and major blood transfusion occurred. All of the following are complications of blood transfusion except?
Which test is not required for Turner mosaic syndrome?
A female was given morphine sulphate during labour for pain but she developed respiratory distress. Which of the following will be the correct antidote?
Absence or mutation of SRY gene results in ?
What condition is associated with the sign seen in the given USG?

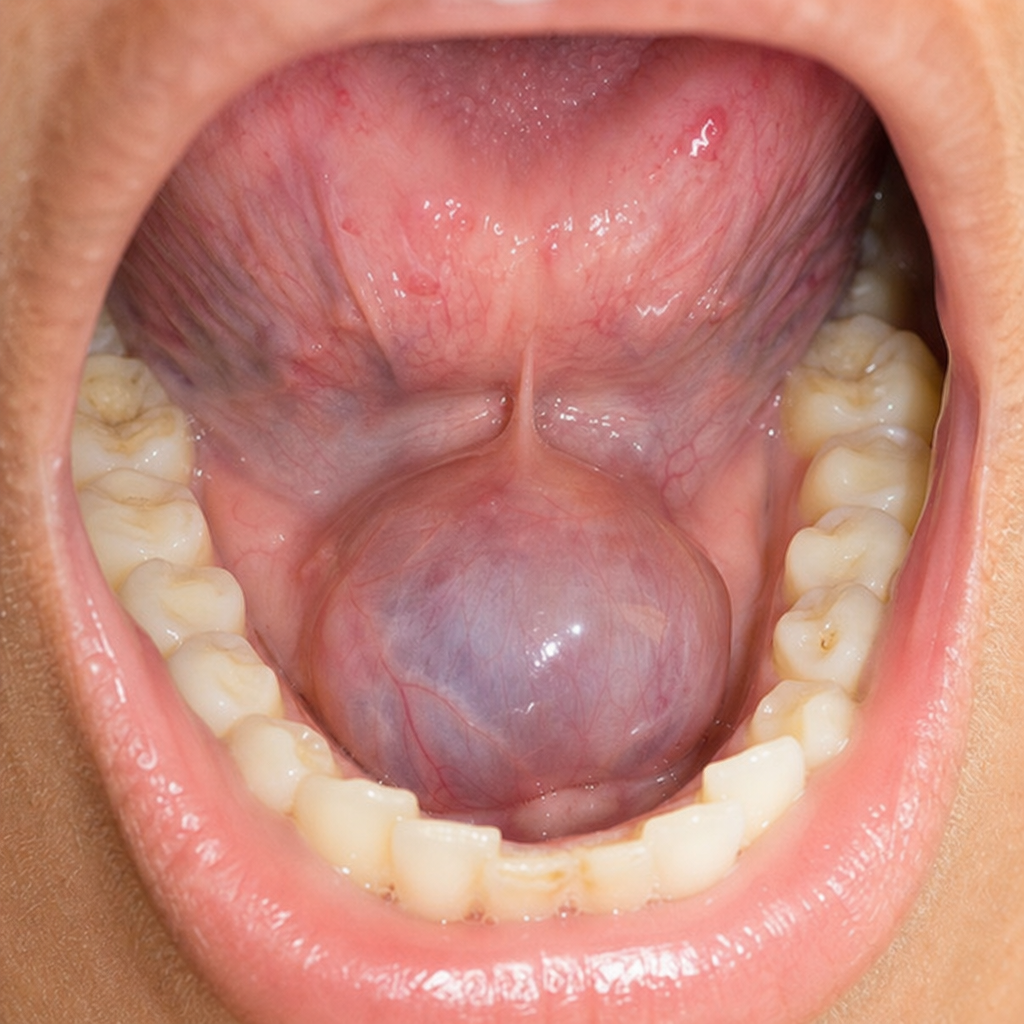
What is the likely diagnosis of the image given below?