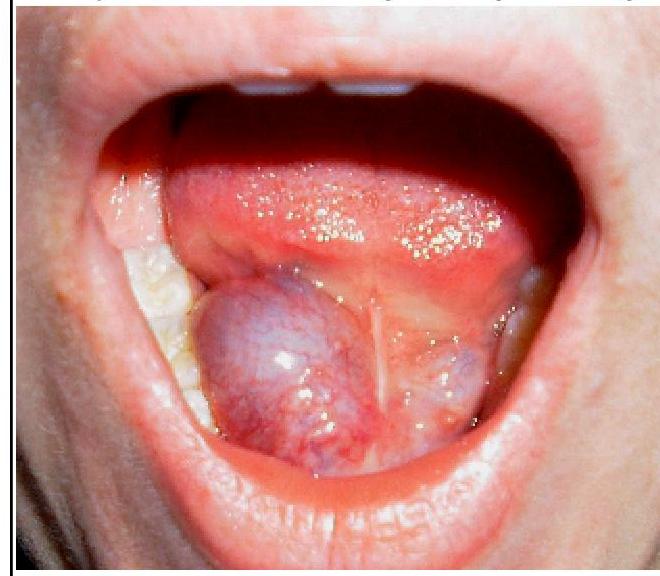
What is the most likely diagnosis for the swelling in the floor of the mouth shown in the image?
After laparoscopic cholecystectomy what should be the urine output of the patient if the renal function of the patient is normal?
What is the baseline platelet count required for surgery?