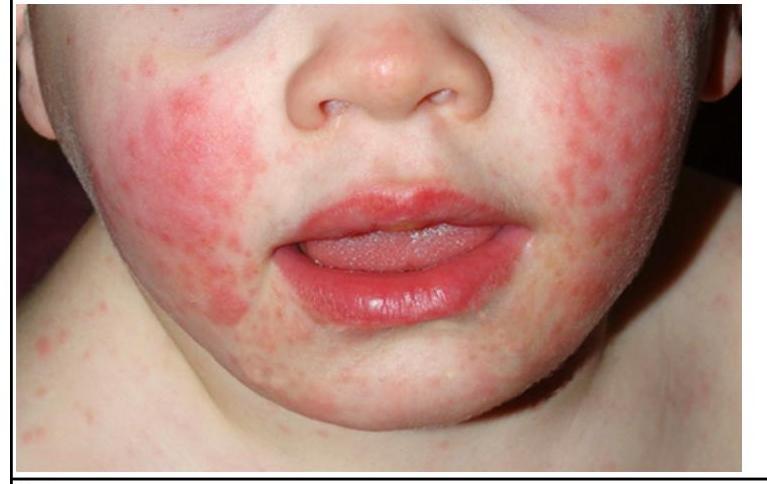
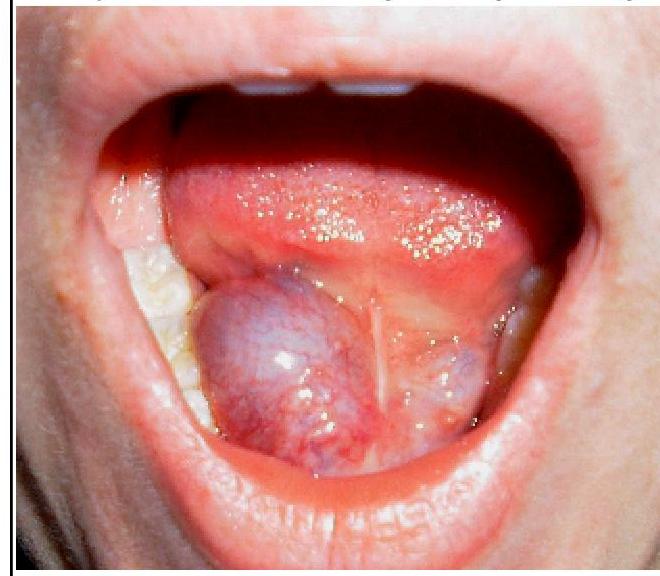
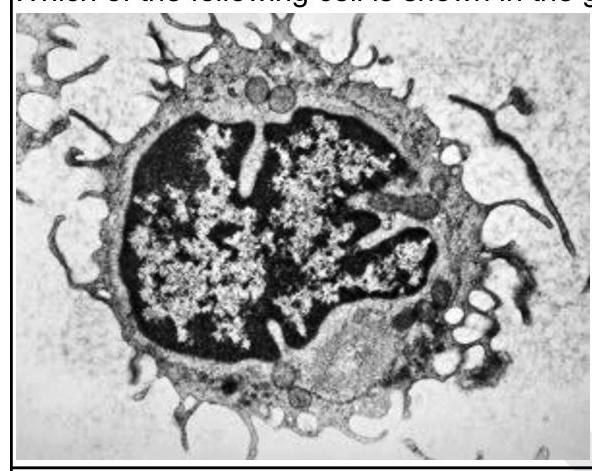
Which of the following cells is shown in the given image?
Match the following? a. Trisomy 13 1. Huntington disease b. Trisomy 18 2. Patau syndrome c. Trinucleotide repeat sequence 3. Sickle cell disease d. Hb point mutation of glutamate to valine 4. Edward syndrome