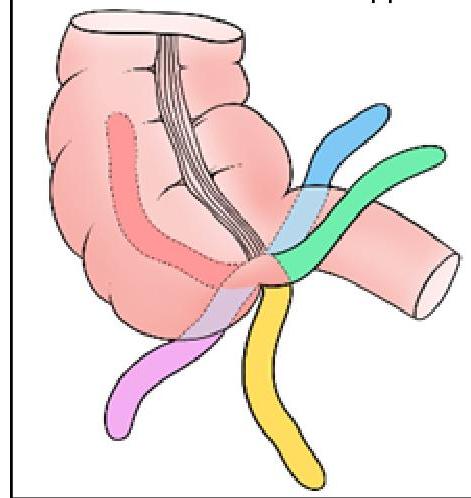
Identify the position of the appendix marked in BLACK in the given image:
What is the incorrect statement?
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
Identify the position of the appendix marked in BLACK in the given image:

What is the incorrect statement?
History of a woman with skin features like limited cutaneous systemic sclerosis (scleroderma) was given. What is the most specific marker?
Which type of amyloidosis is seen in the patients going through dialysis?
CD40 deficiency in a person signifies?
A woman presents with painless ulcers on the vulva, she gives a history of having multiple sexual partners and has had a stillbirth at 28 weeks in the past. What is the next best step of investigation?
All are the causes of non-immune hydrops except?
Which of the following is an Anti-apoptotic gene?
Which of the following are characteristic laboratory findings in Iron Deficiency Anemia (IDA)? 1. Low serum ferritin 2. Low transferrin saturation 3. Low serum iron 4. Increased TIBC
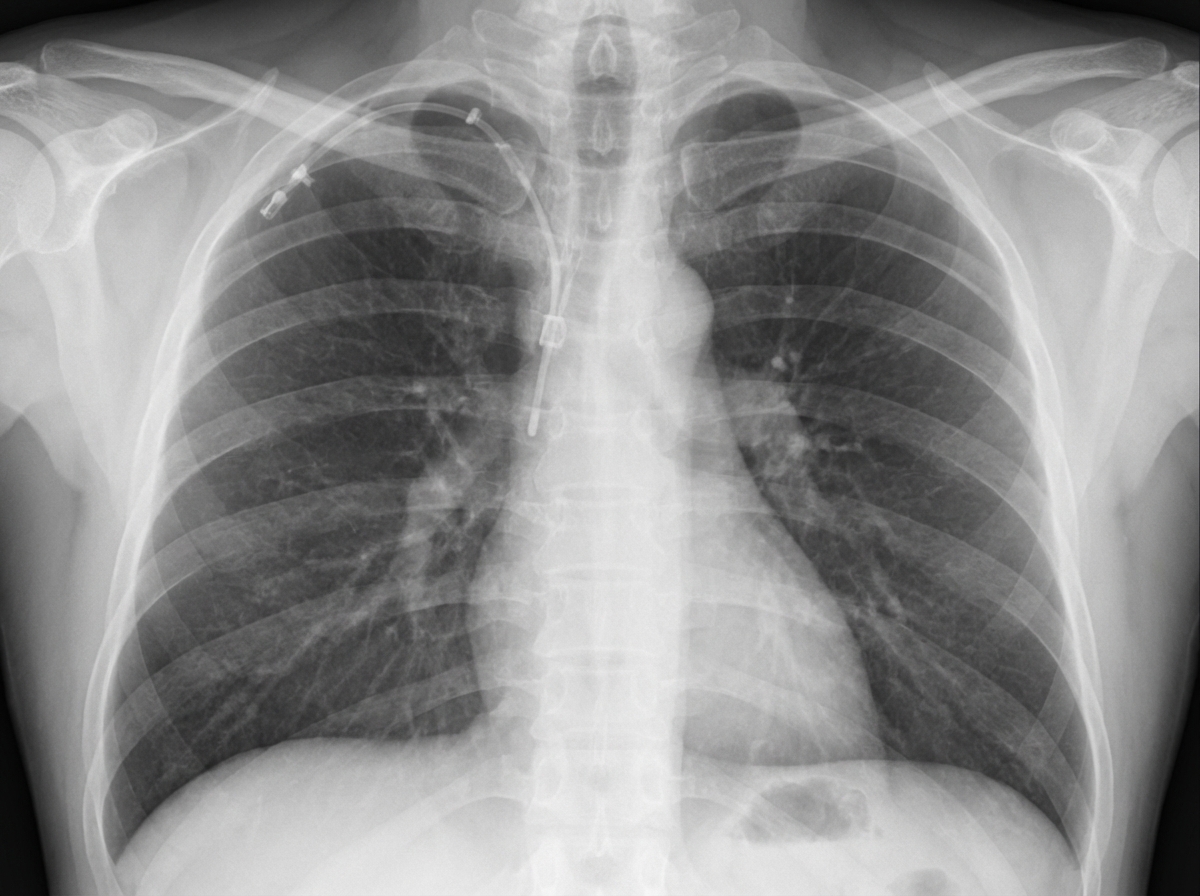
Which of the following is not a known complication associated with the procedure done in the patient?