Arrange the following parts of sarcomere from periphery to center. 1. Z line 2. M line 3. A band 4. H zone
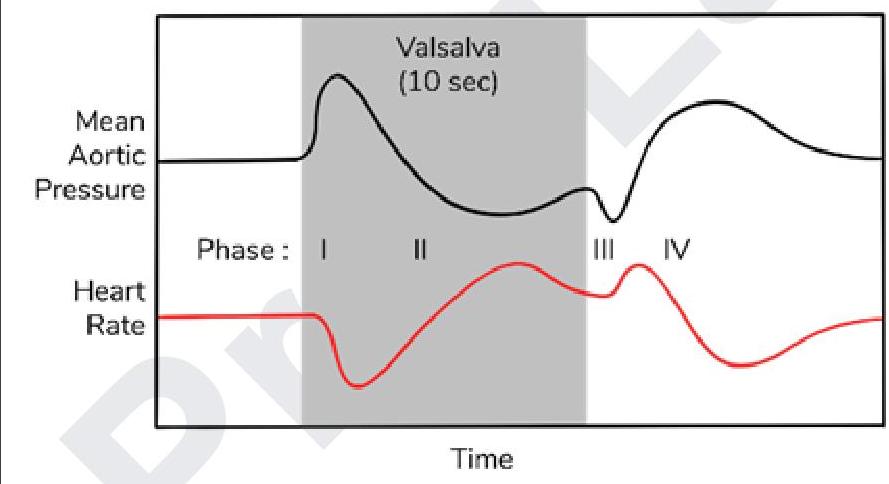
Blood pressure changes in radial artery were measured. Which of the following is the reason for initial rise in BP while performing Valsalva maneuver?
Assertion: RMP depends on proteins and phosphate ions. Reason: Diffusion potential can be calculated using nernst equation. Choose the best statement regarding the assertion and reason.
CO poisoning causes which type of hypoxia?