INI-CET 2023 — Ophthalmology
4 Previous Year Questions with Answers & Explanations
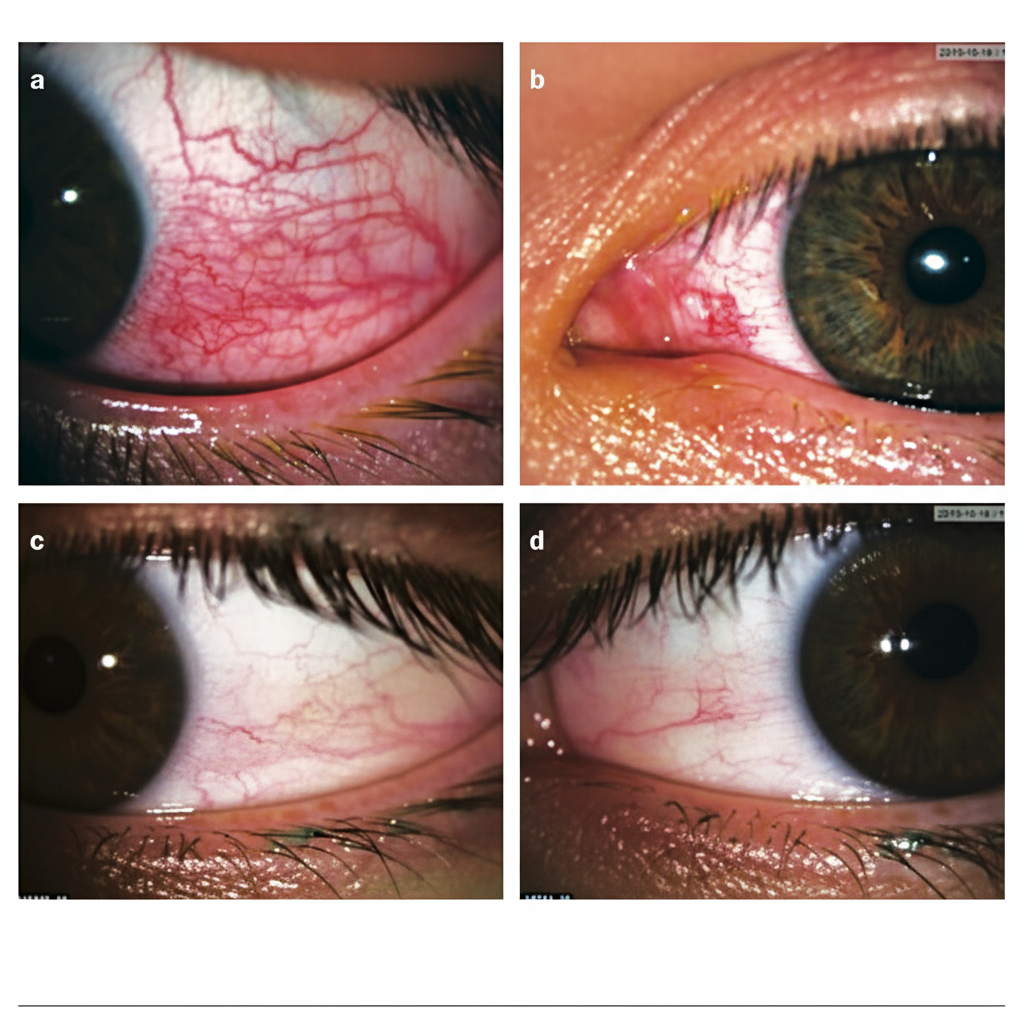
The given image shows blanching of vascularity after the phenylephrine use. What is the likely diagnosis?
Which of the following lens is used in direct gonioscopy?
Identify the correct sequence of staining in dry eyes? 1. Fluorescein stain 2. Lissamine green 3. Rose Bengal stain
What is the earliest change in glaucoma on perimetry?
INI-CET 2023 - Ophthalmology INI-CET Practice Questions and MCQs
Question 1: The given image shows blanching of vascularity after the phenylephrine use. What is the likely diagnosis?
- A. Nodular scleritis
- B. Nodular episcleritis (Correct Answer)
- C. Conjunctivitis
- D. Anterior uveitis
Explanation: ***Nodular episcleritis*** - The image shows a **nodule** on the episclera with surrounding injection that significantly **blanches** after phenylephrine application, which is characteristic of episcleritis. - Episcleritis involves the **superficial episcleral vessels** which respond to topical vasoconstrictors like **phenylephrine (2.5% or 10%)**, leading to blanching. - This is a benign, self-limiting condition that typically presents with **mild discomfort** rather than severe pain. - The **phenylephrine test** is positive in episcleritis (vessels blanch) and helps differentiate it from scleritis. *Nodular scleritis* - Scleritis involves the **deep scleral vessels** which do NOT blanch with phenylephrine application. - Presents with **severe boring pain** that radiates to the forehead, jaw, and face, often waking the patient at night. - The condition is associated with **systemic autoimmune diseases** in 50% of cases (rheumatoid arthritis, SLE, Wegener's granulomatosis). - Requires **systemic treatment** with NSAIDs or immunosuppressives, unlike episcleritis which is self-limiting. *Conjunctivitis* - Presents with **diffuse conjunctival injection** rather than a localized nodule. - Characterized by **discharge** (purulent, mucopurulent, or watery) and typically no pain. - Vessels blanch with phenylephrine, but the clinical presentation lacks the nodular appearance seen in episcleritis. - Associated with symptoms like **itching, foreign body sensation**, and eyelid matting in morning. *Anterior uveitis* - Presents with **circumcorneal (perilimbal) injection** rather than episcleral nodules. - Characterized by **photophobia, blurred vision**, and cells in the anterior chamber on slit-lamp examination. - The injection pattern is **deep ciliary injection** which does not blanch with phenylephrine. - Associated with **hypopyon** in severe cases and requires urgent treatment to prevent complications.
Question 2: Which of the following lens is used in direct gonioscopy?
- A. Koeppe (Correct Answer)
- B. Goldmann
- C. Richardson
- D. Zeiss
Explanation: ***Koeppe*** - The **Koeppe lens** is designed for direct gonioscopy, providing a wide-angle view of the **anterior chamber angle**. - It is typically used with the patient in a **supine position** and requires a coupling solution to be placed directly on the cornea. *Goldmann* - The **Goldmann lens** (3-mirror lens) is used for **indirect gonioscopy** and is characterized by mirrors that reflect the image of the angle. - It is used at a **slit lamp** and provides a magnified view as the light is reflected through the mirrors. *Richardson* - The **Richardson-Shaffer lens** is another direct gonioscopy lens, similar to the Koeppe lens. - However, the question asks for "**the**" lens used in direct gonioscopy, and **Koeppe** is the most commonly recognized and frequently used direct gonioscopy lens. - Richardson-Shaffer is less commonly used in modern practice compared to Koeppe. *Zeiss* - The **Zeiss lens** (4-mirror lens) is used for **indirect gonioscopy** and allows a rapid 360-degree view of the angle. - It is commonly used with a **slit lamp** and requires minimal or no coupling fluid due to its small contact surface.
Question 3: Identify the correct sequence of staining in dry eyes? 1. Fluorescein stain 2. Lissamine green 3. Rose Bengal stain
- A. i, iii, ii
- B. i, ii, iii
- C. ii, iii, i
- D. iii, ii, i (Correct Answer)
Explanation: ***iii, ii, i*** - The correct order for staining in dry eyes is **Rose Bengal, Lissamine Green, and then Fluorescein**. This sequence minimizes the discomfort and potential interference between the dyes. - **Rose Bengal** and **Lissamine Green** stain devitalized or damaged epithelial cells and mucus, while **Fluorescein** stains areas where the epithelium is absent, indicating corneal or conjunctival abrasions or erosions. *i, iii, ii* - This sequence is incorrect because applying fluorescein first could mask the interpretation of epithelial damage by Lissamine Green or Rose Bengal, as it highlights epithelial defects rather than devitalized cells. - The dyes should be applied in an order that optimizes the visualization of different aspects of ocular surface health. *i, ii, iii* - Applying **Fluorescein** first is generally not recommended as it can spread over the ocular surface and potentially interfere with the specific staining patterns of other vital dyes like Lissamine Green or Rose Bengal. - This order does not follow the standard clinical practice for efficient and accurate dry eye assessment. *ii, iii, i* - While Lissamine Green can be used before Fluorescein, placing Rose Bengal after Lissamine Green but still before Fluorescein is not the optimal sequence. - The standard practice aims to assess different layers or types of damage sequentially for a comprehensive evaluation.
Question 4: What is the earliest change in glaucoma on perimetry?
- A. Complete field loss
- B. Isopter contraction + baring of blind spot (Correct Answer)
- C. Tunnel vision defect
- D. Complete vision loss
Explanation: ***Isopter contraction + baring of blind spot*** - Early glaucomatous damage often manifests as an **isopter contraction**, meaning the **visual field narrows** for a given stimulus intensity. - **Baring of the blind spot** occurs when the isopter for a small target contracts inwards, leaving the physiological blind spot exposed to targets that would normally be seen. *Complete field loss* - This is indicative of **very advanced glaucoma**, representing extensive damage to the optic nerve. - It would be preceded by numerous earlier, more subtle visual field defects. *Tunnel vision defect* - **Tunnel vision** is a severe form of visual field constriction, characteristic of **advanced glaucoma** where only the central field of vision remains. - It is not the earliest change as it implies significant peripheral field loss has already occurred. *Complete vision loss* - **Complete vision loss** in an eye signifies end-stage disease, far beyond the earliest changes seen in glaucoma. - It means there is no light perception, indicating total destruction of the optic nerve fibers.