What is the possible cause of irreversible dementia?
What is the correct order for cardiac auscultation on the left side, from superior to inferior? a. Pulmonary b. Tricuspid c. Mitral
Match the following: A) Caplan syndrome- 1) Found first in coal worker B) Asbestosis- 2) Upper lobe predominance C) Mesothelioma- 3) Involves lower lobe D) Sarcoidosis- 4) Pleural effusion is seen
A patient presented with complaints of pain in the flank region with hematuria. On investigation, X-ray shows multiple calcification (stones) in both kidneys. What is the probable diagnosis?
KEYNOTE-189 trial for pembrolizumab is done for?
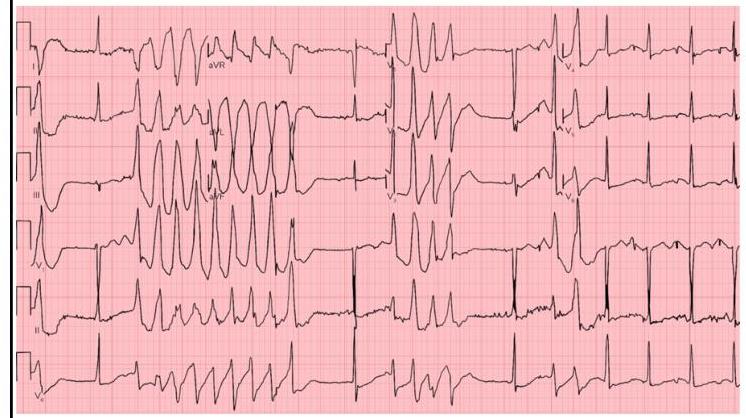
Identify the ECG given below?
Which of the following describes aortic regurgitation murmur?
All of the following are the causes of High output cardiac failure, except?