INI-CET 2023 — Dermatology
7 Previous Year Questions with Answers & Explanations
Slapped cheek appearance is associated with which of the following?
A man presents with a rash on his flank with itching for the past 2 weeks. The patient has tried several over-the-counter medications, including lotrimin and hydrocortisone, without any improvement. In physical examination, the rash is seen on his palms and the sole of one foot, but no oral lesions are found. What is the likely diagnosis?
Match the following woods lamp findings: 1. Erythrasma, 2. Pityriasis versicolor, 3. Tinea capitis, 4. Vitiligo || a. Yellow b. Coral red fluorescence c. Pink d. Green e. Milky white
Non-scarring alopecia is associated with all except?
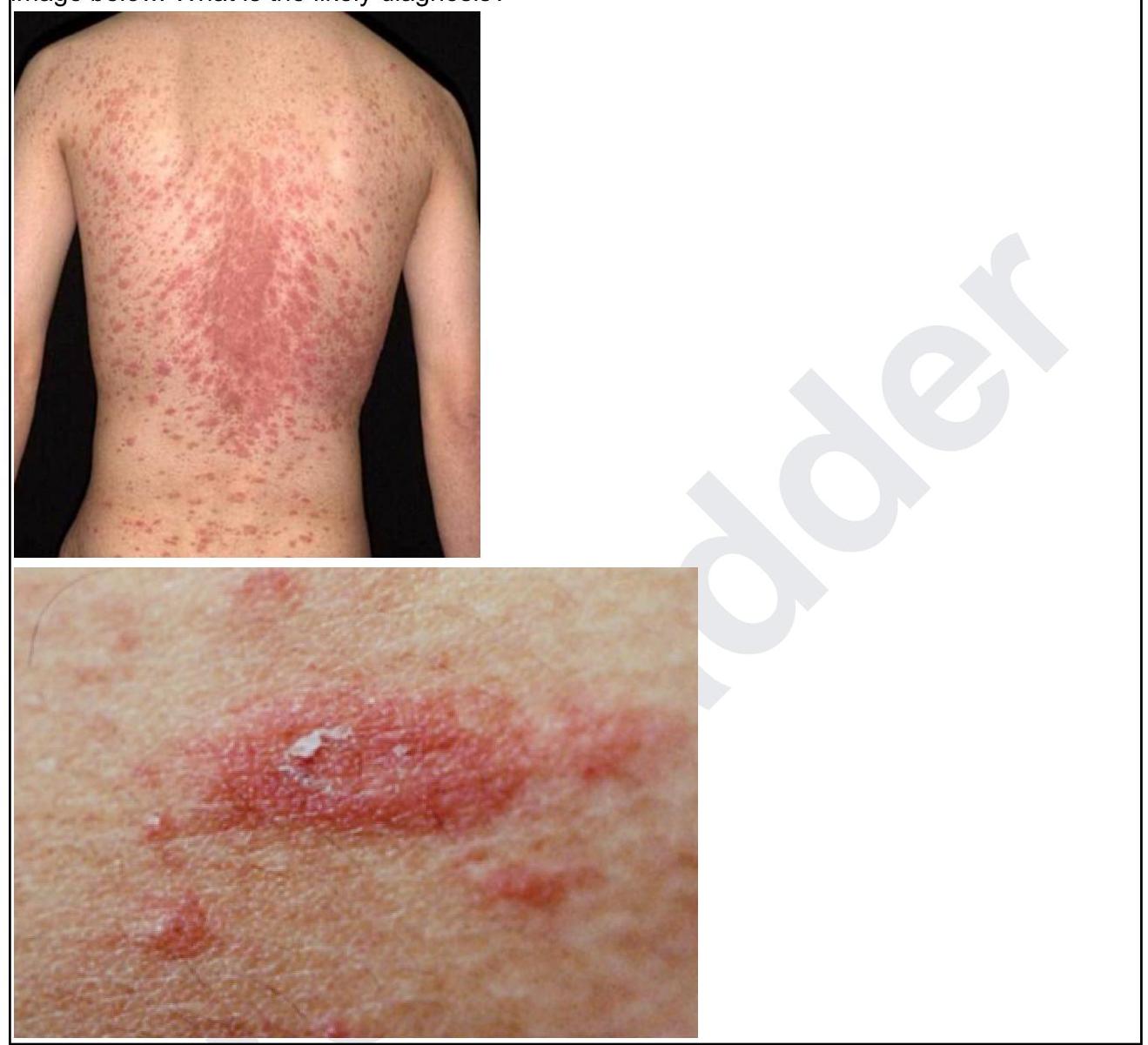
A 24-year-old male presents with asymptomatic scaly lesions over the body as shown in the image below. What is the likely diagnosis?
Statement 1 - A 59-year-old patient presents with flaccid bullae. Histopathology shows a suprabasal acantholytic split. Statement 2 - The row of tombstones appearance is diagnostic of Pemphigus vulgaris.
A 60-year-old female presents with eczematous itching lesions. Biopsy revealed a subepidermal cleft with Direct Immunofluorescence showing Linear C3 & IgG deposition along the basement membrane zone. What is the likely diagnosis?
INI-CET 2023 - Dermatology INI-CET Practice Questions and MCQs
Question 1: Slapped cheek appearance is associated with which of the following?
- A. Herpes zoster
- B. Parvovirus B19 infection (Correct Answer)
- C. Molluscum contagiosum
- D. Kaposi sarcoma
Explanation: ***Parvovirus B19 infection*** - **Parvovirus B19** infection, also known as Fifth Disease or **Erythema Infectiosum**, classically presents with a **slapped cheek rash** on the face. - This characteristic facial rash is usually followed by a **lacy, reticular rash** on the trunk and extremities. *Herpes zoster* - **Herpes zoster** (shingles) presents as a painful, vesicular rash that follows a **dermatomal distribution**. - It does not cause a **slapped cheek appearance**; its rash is typically unilateral and confined to a single dermatome. *Molluscum contagiosum* - **Molluscum contagiosum** is characterized by small, flesh-colored, **umbilicated papules** with a central dimple. - These lesions can occur anywhere on the body but do not produce a diffuse facial rash like the **slapped cheek appearance**. *Kaposi sarcoma* - **Kaposi sarcoma** is a vascular tumor that manifests as **purple, brown, or reddish skin lesions**, often seen in immunocompromised individuals. - It is not associated with a **widespread facial rash** or the characteristic distribution of a slapped cheek appearance.
Question 2: A man presents with a rash on his flank with itching for the past 2 weeks. The patient has tried several over-the-counter medications, including lotrimin and hydrocortisone, without any improvement. In physical examination, the rash is seen on his palms and the sole of one foot, but no oral lesions are found. What is the likely diagnosis?
- A. Tinea corporis
- B. Pityriasis rosea
- C. Secondary syphilis (Correct Answer)
- D. Contact dermatitis
Explanation: ***Secondary syphilis*** - The rash presenting on the **palms and soles** is highly characteristic of **secondary syphilis**, which helps differentiate it from many other dermatological conditions. - The lack of improvement with antifungal (Lotrimin) and corticosteroid (hydrocortisone) treatments further supports a diagnosis other than a fungal infection or inflammatory dermatitis. *Tinea corporis* - This fungal infection typically presents as an **annular (ring-shaped) rash** with central clearing and well-demarcated borders, often on the trunk or limbs. - It would likely show some improvement, even if partial, with **Lotrimin (an antifungal medication)**, which is not the case here. *Pityriasis rosea* - This condition is characterized by an initial **"herald patch"** followed by smaller, oval, pinkish-red patches that often align along skin cleavage lines in a **"Christmas tree" pattern** on the trunk. - It typically spares the palms and soles, which are involved in this patient's presentation. *Contact dermatitis* - This is an inflammatory skin reaction due to contact with an allergen or irritant, presenting as **pruritic (itchy) erythematous (red) patches, possibly with vesicles or bullae**, limited to exposed areas. - While hydrocortisone might offer some relief, the presentation on palms and soles without clear exposure and the lack of response to treatment make it less likely.
Question 3: Match the following woods lamp findings: 1. Erythrasma, 2. Pityriasis versicolor, 3. Tinea capitis, 4. Vitiligo || a. Yellow b. Coral red fluorescence c. Pink d. Green e. Milky white
- A. 1-d, 2-a, 3-c, 4-e
- B. 1-b, 2-a, 3-d, 4-e (Correct Answer)
- C. 1-a, 2-c, 3-e, 4-d
- D. 1-b, 2-d, 3-a, 4-c
Explanation: ***1-b, 2-a, 3-d, 4-e*** - **Erythrasma** is caused by *Corynebacterium minutissimum* and produces **porphyrins** that fluoresce **coral red** under a Wood's lamp [1]. - **Pityriasis versicolor** is caused by *Malassezia furfur* and typically fluoresces **yellow to yellowish-green** [2]. - **Tinea capitis** (especially due to *Microsporum* species) shows **green fluorescence** of infected hairs. - **Vitiligo** lesions, due to a complete absence of melanin, appear as **milky white** or bright white areas under a Wood's lamp [3]. *1-d, 2-a, 3-c, 4-e* - This option incorrectly states that Erythrasma fluoresces green. Green fluorescence is characteristic of *Microsporum* species causing **Tinea capitis**. - Additionally, Tinea capitis is incorrectly associated with pink fluorescence, which is not a typical finding. *1-a, 2-c, 3-e, 4-d* - This option incorrectly states that Erythrasma fluoresces yellow. Yellow fluorescence is associated with **Pityriasis versicolor** [2]. - It also incorrectly assigns milky white fluorescence to Tinea capitis and green fluorescence to Vitiligo. *1-b, 2-d, 3-a, 4-c* - This option incorrectly associates Pityriasis versicolor with green fluorescence. While some variations exist, **yellow** is the more characteristic finding [2]. - It also incorrectly links Tinea capitis to yellow fluorescence and Vitiligo to pink, which are not typical Wood's lamp findings for these conditions.
Question 4: Non-scarring alopecia is associated with all except?
- A. Telogen effluvium
- B. Androgenetic alopecia
- C. Alopecia areata
- D. Frontal fibrosing alopecia (Correct Answer)
Explanation: ***Frontal fibrosing alopecia*** - This condition is a form of **lichen planopilaris**, which causes **scarring alopecia** due to destruction of hair follicles and replacement with fibrous tissue. - It results in a **receding hairline** and eyebrow loss, with irreversible hair loss. *Telogen effluvium* - This is a common cause of **non-scarring alopecia**, characterized by diffuse hair shedding triggered by various stressors like illness, stress, or medications. - The hair follicles enter the **telogen phase** prematurely, leading to increased shedding but typically regrowth once the trigger is removed. *Androgenetic alopecia* - Often referred to as **male or female pattern baldness**, this is a form of **non-scarring alopecia** driven by genetic predisposition and androgens. - It causes a progressive miniaturization of hair follicles, leading to thinning hair, but the follicles remain present and capable of producing hair. *Alopecia areata* - This is an **autoimmune condition** that causes **non-scarring hair loss** in patches on the scalp or other parts of the body. - The hair follicles are attacked by the immune system but are not permanently destroyed, allowing for potential regrowth.
Question 5: A 24-year-old male presents with asymptomatic scaly lesions over the body as shown in the image below. What is the likely diagnosis?
- A. Atopic Dermatitis
- B. Lichen planus
- C. Seborrheic Dermatitis
- D. Pityriasis Rosea (Correct Answer)
Explanation: ***Pityriasis Rosea*** - The image shows numerous **scaly, erythematous plaques** distributed over the trunk, with a characteristic "Christmas tree" pattern often observed in Pityriasis Rosea. - The lesions are described as **asymptomatic**, which is consistent with Pityriasis Rosea, although mild pruritus can occur. *Atopic Dermatitis* - Typically presents with **intensely pruritic, erythematous, and eczematous lesions** often found in flexural areas (e.g., antecubital and popliteal fossae). - While it can be widespread, the morphology of the lesions (eczematous vs. scaly plaques) and the absence of pruritus make this less likely. *Lichen planus* - Characterized by **pruritic, violaceous, polygonal papules** and plaques, often appearing on the flexor surfaces of wrists, ankles, and oral mucosa. - The appearance of the lesions in the image does not match the typical morphology of lichen planus. *Seborrheic Dermatitis* - Primarily affects areas with a high density of sebaceous glands, such as the **scalp, face (nasolabial folds, eyebrows), and chest**. - Presents with **greasy, yellowish scales** on an erythematous base, which is distinct from the dry, scaly plaques seen in the image.
Question 6: Statement 1 - A 59-year-old patient presents with flaccid bullae. Histopathology shows a suprabasal acantholytic split. Statement 2 - The row of tombstones appearance is diagnostic of Pemphigus vulgaris.
- A. Statements 1 & 2 are correct, 2 is not explaining 1 (Correct Answer)
- B. Statements 1 and 2 are correct and 2 is the correct explanation for 1
- C. Statements 1 and 2 are incorrect
- D. Statement 1 is incorrect
Explanation: ***Correct: Statements 1 & 2 are correct, 2 is not explaining 1*** **Analysis of Statement 1:** - A 59-year-old patient with **flaccid bullae** and **suprabasal acantholytic split** on histopathology is the classic presentation of **Pemphigus vulgaris** - The flaccid (easily ruptured) nature of bullae distinguishes it from tense bullae seen in bullous pemphigoid - The suprabasal location of the split (just above the basal layer) with acantholysis (loss of cell-to-cell adhesion) is pathognomonic - **Statement 1 is CORRECT** ✓ **Analysis of Statement 2:** - The **"row of tombstones" or "tombstone appearance"** is indeed a diagnostic histopathological feature of Pemphigus vulgaris - This appearance results from basal keratinocytes remaining attached to the basement membrane while suprabasal cells separate due to acantholysis - The intact basal cells standing upright resemble a row of tombstones - **Statement 2 is CORRECT** ✓ **Does Statement 2 explain Statement 1?** - Statement 2 describes a **histopathological appearance** (tombstone pattern) that is a **consequence** of the suprabasal split - However, it does NOT explain the **underlying cause** of the flaccid bullae or the suprabasal split - The true explanation involves **IgG autoantibodies against desmoglein 3 (and desmoglein 1)**, which attack intercellular adhesion structures (desmosomes), causing **acantholysis** - Therefore, **Statement 2 does NOT explain Statement 1** ✗ *Incorrect: Statement 2 is the correct explanation for Statement 1* - While both statements describe features of Pemphigus vulgaris, the tombstone appearance is a descriptive finding, not an explanatory mechanism *Incorrect: Statements 1 and 2 are incorrect* - Both statements are medically accurate descriptions of Pemphigus vulgaris features *Incorrect: Statement 1 is incorrect* - Statement 1 correctly describes the cardinal clinical and histopathological features of Pemphigus vulgaris
Question 7: A 60-year-old female presents with eczematous itching lesions. Biopsy revealed a subepidermal cleft with Direct Immunofluorescence showing Linear C3 & IgG deposition along the basement membrane zone. What is the likely diagnosis?
- A. Pemphigus foliaceus
- B. Pemphigus Vulgaris
- C. Dermatitis herpetiformis
- D. Bullous Pemphigoid (Correct Answer)
Explanation: ***Bullous Pemphigoid*** - The presence of **eczematous itching lesions**, a **subepidermal cleft**, and **linear C3 and IgG deposition along the basement membrane zone** on direct immunofluorescence (DIF) are classic diagnostic features of Bullous Pemphigoid. - This autoimmune blistering disease typically affects older individuals and is characterized by antibodies targeting components of the **hemidesmosomes**, specifically BP180 and BP230. *Pemphigus foliaceus* - This condition involves **intraepidermal blistering**, specifically within the granular layer, rather than a subepidermal cleft. - DIF in Pemphigus foliaceus shows **intercellular IgG deposition** in the epidermis, not linear deposition along the basement membrane zone. *Pemphigus Vulgaris* - Pemphigus Vulgaris is characterized by **intraepidermal blistering** above the basal cell layer (**suprabasal clefting**), leading to fragile bullae that rupture easily. - DIF typically reveals **intercellular IgG and C3 deposition** in a "chicken wire" pattern throughout the epidermis, which differs from the linear pattern seen in this case. *Dermatitis herpetiformis* - While Dermatitis herpetiformis is also an autoimmune blistering disease with itching lesions, its characteristic DIF finding is **granular IgA deposition** in the dermal papillae, not linear C3 and IgG at the basement membrane zone. - Histopathology in Dermatitis herpetiformis shows **subepidermal vesicles** with neutrophil infiltration in the dermal papillae, but the direct immunofluorescence pattern is distinct.